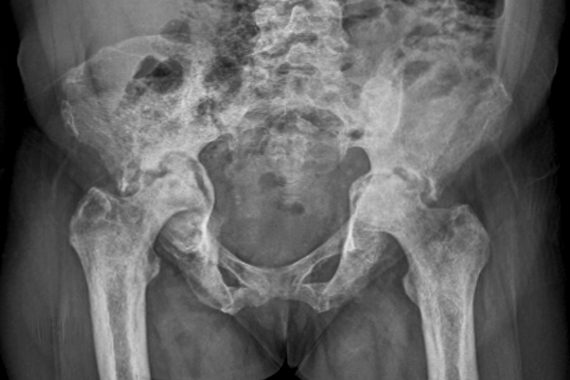
Case
A 30-year-old man presents with persistent diffuse pain around his right buttock, groin and upper thigh. There is mild discomfort when weight-bearing and performing extreme movements of the hip. X-rays and blood tests are normal. The GP knows that anyone presenting with unexplained hip pain with the symptoms listed above, particularly those using high-dose steroids, should be suspected as having avascular necrosis (AVN).
The problem
Avascular necrosis (AVN), or osteonecrosis of the femoral head, is caused by an episode of inadequate blood supply that leads to the death of bone cells within all or part of the femoral head. If the affected area is relatively large, this commonly leads to collapse of the femoral head, resulting in articular deformity, incongruity of the joint and subsequent secondary degenerative change.
It is one of the most common causes of hip arthritis in young adults and is often rapidly progressive, leading to joint replacement at a young age. While most cases arise idiopathically, it can be associated with:
- Corticosteroid use
- Fractures and dislocations of hip joint
- Surgery around the hip
- Chronic alcohol intake
- Embolic and thrombolic disorders
- Autoimmune disease
- Immunosuppression
- Pregnancy
- HIV infection
In non-traumatic cases, bilateral presentation is frequently seen in around 55% of patients within two years of the initial presentation, with males more commonly affected.
Features
AVN should be considered in any adult presenting with persistent unexplained hip pain, particularly in patients who are systemically well with normal blood tests and X-rays. The early symptoms are unfortunately non-specific, and many early cases are asymptomatic. The most common presentation is in the third to fifth decade of life, with males more commonly affected than females, and 50% of cases being bilateral.
Pain presents as an insidious and chronic onset mild pain in the groin, radiating to the thigh or buttock. Patients usually suffer with a limp, and experience pain on the extremes of movement, particularly on rotation. Deep hip pain in the absence of localised tenderness over the trochanter or tendinous end of the hamstrings, adductors and abductors will distinguish between AVN and bursitis, groin strains and chronic tendinopathies, to some extent.
The assessment of a physiotherapist can be helpful, but a high index of suspicion is vital given the non-specific symptoms in the early stages of the condition and the other potential cause of pain around the hip. As the degree of femoral collapse increases so does the pain and symptoms of clicking, catching and giving way develop, in the final stages the patient presents with a picture of established osteoarthritis of the hip.
Classifications are based around radiological appearance:
- Stage 1 – normal X-ray
- Stage 2 – normal head sphericity with sclerosis or cysts
- Stage 3 – flattening or collapse of the head
- Stage 4 – established arthritis of the joint
Ironically, in terms of management, radiographs on their own are unhelpful, as they are normal, or near normal, in the early – and potentially treatable – stages of the disease. However, they are useful to exclude other diagnosis, such as early osteoarthritis, other intraosseous pathology, and stress fractures.
Diagnosis
The investigation of choice is an MRI scan, and should be performed early in the history, particularly in the presence of a normal radiograph with persisting hip pain. Radioisotope bone scanning is slightly less sensitive, it being cold in the early avascular stage and hot in the revascularising and remodeling stages, and while it may have a role where multiple joint AVN is suspected, it has the disadvantage of unnecessary radiation exposure compared to MRI.
Access to investigation modalities can vary across general practice. If MRI scanning is not available, it is important to make clear that AVN is suspected when ordering an X-ray of the hip, so the radiology department can direct additional appropriate investigations. It may, however, be necessary to refer suspected cases early and directly to orthopaedic services, depending on local arrangements for assessment, investigation and treatment. All cases of AVN of the hip diagnosed should be referred for specialist assessment and possible treatment with relative urgency.
If there is any question that joint infection may be suspected as part of the differential diagnosis, then this requires immediate emergency referral to hospital without delay.
Management
Because the treatment of AVN is relatively poor in preventing the progression of the disease, a number of treatment options have been developed, although the results are variable, and further research is needed.
Treatment modalities in AVN of the hip
Non-invasive
- NSAIDs
- Simple analgesics
- Rest, with limited weight bearing to prevent collapse, potentially for months
- Exercise, avoiding high impact to preserve a range of movement
- Osteoporosis drugs like bisphosphonates, if attempting to prevent later bone collapse
- Cholesterol-lowering drugs, in the presence of high levels of lipids
- Anticoagulants and antithrombotics, in cases with hypercoagulability disorders
- Electrical and magnetic stimulation to encourage bone growth
Invasive
- Core decompression to attempt to revascularise the femoral head
- Bone graft transplant that may be micro-vascularised
- Osteotomy
- Joint replacement
- Regenerative medicine treatment, stimulate vessel or bone growth in the affected area
Treatment options are dependent on the stage of the disease at diagnosis.
ANV is unfortunately often diagnosed late on, during stages 3 and 4, where the treatment is – as for any one with arthritis of the hip – lifestyle changes and analgesia. There are occasionally indications for osteotomy of the femoral neck, to increase the congruity of the weight-bearing area of the joint, but this is not commonly performed.
The vast majority of patients in these groups who progress to joint replacement surgery are often relativity young and active patients, who will require subsequent revision surgery over the years.
For stages 1 and 2, where bone collapse has not yet occurred, treatment is aimed at preserving the sphericity of the femoral head. The evidence that reduced weight-bearing alone is an effective treatment remains inconclusive, and unfortunately has to be prolonged for months until there is evidence of bone healing.
However, in the absence of a single definitive effective treatment, and given the consequences of subsequent femoral head collapse, partial weight-bearing is often employed in combination with other treatments. The use of bisphosphonate drugs to inhibit osteoclast activity – while theoretically attractive – is also limited in its effect, improving radiological appearances in the medium-term, but ultimately not often resolving the process clinically. Attempts to stimulate bone healing, including extracorporeal shock therapy, magnetic and electrical field stimulation, are largely ineffective to date.
Surgical intervention to revascularise and support the area surrounding the necrotic bone is the most commonly employed treatment. The simplest and most frequently performed procedure is core decompression, involving drilling into the avascular necrotic or cystic area of the femoral head, under X-ray control, to produce a channel to allow revascuralisation to occur. This can be combined with a vascularised bone graft or a porous metal implant, to not only allow revascularisation, but also support the femoral subchondral bone to help prevent collapse of the joint surface. These techniques can also be augmented biologically with the insertion of bone or stem cells at the same time to stimulate bone healing. The risks of these procedures are subsequent femoral fracture at the entry point of drilling, and infection. Early diagnosis is the key and research in this area continues.