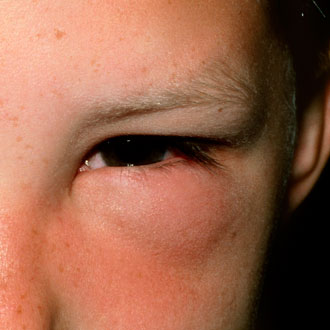
1. Food allergies are common in childhood
Food allergy affects 6% to 8% of children and is potentially, albeit rarely, life threatening. The prevalence of food allergy is highest in infants and toddlers, with 2.5% of infants suffering from cow’s milk allergy and up to 8% of children below the age of three years affected. The most common food allergies are to cow’s milk, egg, peanut, tree nuts, fish, shellfish, sesame, soya and wheat.
2. IgE-mediated symptoms occur rapidly
Symptoms usually occur within minutes of food ingestion and no more than two hours later. They can affect various body systems including the skin (pruritus, urticaria, angioedema), the gastrointestinal tract (abdominal pain, nausea, vomiting, diarrhoea), and in severe reactions, the respiratory tract (stridor, cough, wheeze) and the cardiovascular system (hypotension, collapse). The symptoms occurring in IgE-mediated food allergy are always reproducible and happen every time the allergenic food is eaten.
3. Know the common risk factors for food allergies
The presence of severe, early-onset eczema (before six months of age) is a known risk factor for food allergy. Atopic family history is also important. For example, a child with a parent or sibling with peanut allergy has a seven-fold increase in the risk of developing peanut allergy. The presence of one food allergy increases the likelihood of another. For example, egg allergy is also associated with an increased risk of developing peanut allergy and peanut allergy with an increased risk of tree nut and sesame allergy.
4. Not all food allergies present in the same way
Non-IgE mediated (delayed type) food allergies usually present with gastrointestinal symptoms, including gastroesophageal reflux (unresponsive to usual medication), colic, diarrhoea, blood-streaked stools, abdominal pain, constipation, food aversion and faltering growth. Non-IgE mediated food allergies are often delayed, with symptoms presenting several hours to days after food ingestion, causing difficulty in diagnosis. Ongoing consumption of the problem food, typically milk in infancy, will present with persistent, chronic symptoms as opposed to distinct reactions.
5. If food allergy is suspected, arrange for appropriate testing
Skin prick testing or food-specific IgE are useful tests for the diagnosis of IgE-mediated food allergy, but they must be supported by a convincing clinical history. Allergy tests have good sensitivity (>95%) but they lack specificity (around 50%). Therefore, a positive test merely indicates that a child is sensitised to a particular food and often requires further investigation to confirm the diagnosis (i.e. a convincing clinical history or a food challenge), whereas a negative test practically rules out IgE-mediated food allergy. There are no validated diagnostic tests for non-IgE mediated food allergy.
6. Food allergy is not always for life
Certain food allergies are outgrown in childhood and not usually carried onto adult life. The majority of children will outgrow their cow’s milk, egg, soya and wheat allergy. Other allergies such as nut, fish and shellfish are rarely outgrown. Only in 20% of children is peanut allergy expected to resolve, and the percentage is even lower for tree nut allergy, at approximately 10%.
7. Avoidance and an emergency management plan are the basis of treatment
Following a diagnosis of food allergy, all children should be given advice on how to avoid the relevant allergen, as well as a management plan with information on how to deal with allergic reactions, if they occur. Emergency medication should also be provided. Antihistamines are given to all children with food allergy. Adrenaline is usually also provided if the initial reaction was severe, if the child reacted to very small amounts of the allergen and in cases of children with significant asthma.
8. Dietitian input is important in the child with food allergy
A full nutritional assessment and clear, comprehensive advice on avoidance diet should be provided by a trained dietitian. Advice on reading food labels and on choosing alternative products is of great value to families with food-allergic children. The dietitian plays a key role as part of a multidisciplinary management of the food-allergic child, especially in infants during early life and in children with multiple/complex food allergies.
9. Know which alternatives are suitable in milk avoidance diets
For infants diagnosed with cow’s milk allergy, a hypoallergenic formula is usually suggested as an alternative. It is important to remember that soya milk is not suitable for infants below six months. Goat’s milk and sheep milk are not appropriate choices either, as there is a lot of cross-reactivity between these species and the child is likely to react. Guidelines are available, for example, the MAP guideline, to guide choice of hypoallergenic formula. Calcium supplements may be required for some cow’s milk allergic children.
10. Food allergy is associated with various comorbidities
Children with food allergy usually have a background of eczema and are likely to develop allergic rhinitis and asthma, both known comorbidities. All four conditions are part of the ‘allergic march’ – the gradual acquisition of overlapping allergic diseases that commonly begins in early childhood – which often begins with atopic dermatitis in early life and continues with the development of food allergy, allergic rhinitis and asthma. These conditions also impact on each other – rhinitis worsens asthma, asthma predisposes to more severe food allergic reactions etc so holistic management of all allergic comorbidities is key.
Dr Adam Fox is a consultant in paediatric allergy, and Dr Katherine Anagnostou is a specialist registrar in paediatric allergy, both based at Guy’s and St Thomas’ Hospitals NHS Foundation Trust
Further reading
NICE clinical guideline 116 – Food allergy in children and young people. National Institute for Health and Clinical Excellence (2011).Diagnosis and assessment of food allergy in children and young people in primary care and community settings. London: National Institute for Health and Clinical Excellence. Available from: www.nice.org.uk/guidance/CG116
Venter C, Brown T, Walsh J, Shah N, Fox AT. Diagnosis and management of non-IgE-mediated cow’s milk allergy in Infancy – a UK Primary Care practical guide. British Journal of General Practice 2014;.64(618):48-49.
Ludman S, Shah N, Fox AT. Managing Cow’s Milk Allergy in Children. British Medical Journal 2013;347:f5424.
Fox AT, Lloyd K, Arkwright PD, Bhattacharya D, Brown T, Chetcuti P, East M, Gaventa J, King R, Martinez A, Meyer R, Parikh A, Perkin M, Shah N, Tuthill D, Walsh J, Waddell L, Warner JO. Royal College of Paediatric and Child Health (RCPCH) care pathway for food allergy in children: an evidence and consensus based national approach to caring for children with allergies. Arch Dis Child 2011;96:i25-i29.