In Lancashire North, we are proud of our recent achievements in end-of-life care, as we have worked hard to steadily increase the proportion of our patients dying in their usual place of residence. This was achieved partly by universal adoption of the GSF (Gold Standard Framework) Going for Gold quality improvement programme.
We have also worked hard to develop a local Electronic Palliative Care Co-ordination System (EPaCCs), whereby records held on the GP system (EMIS Web) are shared appropriately using the medical interoperative gateway (MiG). We are mindful that the duty to share information can be as important as the duty to protect patient confidentiality .
There is strong evidence that EPaCCs supports patient choice, shared decision making, individual care planning and integration of care across sectors.
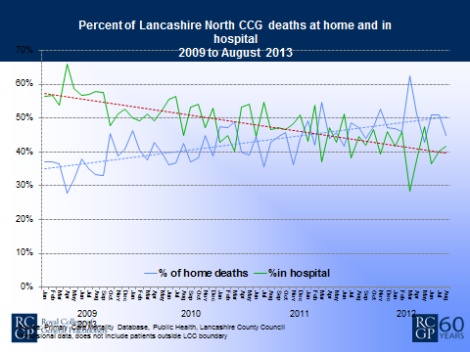
Many areas have already implemented or are in the process of implementing EPaCCSs across localities. Available data suggests that their use helps people to die in their preferred place of death, decreases the percentage of hospital deaths and increases the percentage of deaths at home and in hospices.
The system in Lancashire North is shown diagrammatically here, UHMB being the local hospital:
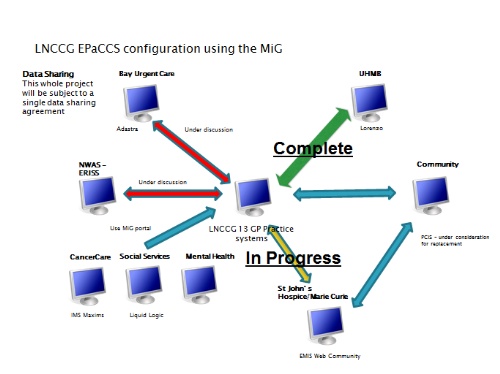
Having worked to establish sharing of our palliative care registers by making the information on our Palliative Care Templates, which are EPaCCs compatible, available to share, we had great concerns that the new English Unplanned admissions DES would cause problems as. It was initially hard, given current pressures, to see GPs and their staff completing both a template for the 2% on the new DES and also the 1% on our palliative care registers.
We have found a solution and this is the Lancashire North plan:
- We are renaming palliative care registers to make them fit the DES requirement of case management registers. They are now called supportive care registers. This acknowledges that for many of our patients (GSF code blue), we know that they are in the last years of life but it is increasingly difficult with co-morbidities to know when someone is in the last year of life. It is also much easier to let people know that they are on a register to protect them from unplanned admissions than to discuss end of life issues when people could have many years to live, although offering high quality Advance Care planning is encouraged as soon as the patient wants it.
- We have developed a single EMIS template that has all the DES and EPaCCs codes built into it. We can then use the computer to quickly generate a care plan to give to the patient to fulfil the DES requirement. Our local GP federation (North Lancashire Medical Services) produced this template.
- Our monthly palliative care meetings are now in effect ‘GSF plus’ and called supportive care meetings. We link to long term conditions and mention the relatively few patients with mental health, asthma or other issues that make them vulnerable to unplanned admissions. Staff then complete the template entries when required. To make this all manageable in a one-hour meeting, the patients to discuss are prioritised using RAG (red amber green) coding for our 1%. The ‘blues’, the majority of our patients with possibly years to live, but who are vulnerable giving us our required 2%. GSF ‘Going for Gold’ training helped with this prioritisation process.
- We are asking for derogation from the local area team of NHS England to hopefully give the GP practices time to produce high quality and useful plans rather than a large quantity of lower quality plans. I understand that Local Area teams have been instructed to stick to the detail of the agreed DES, but asking for some flexibility in the interpretation of rules may still be worthwhile.
I hope these ideas may be of use in your area.
Dr Peter Nightingale is joint Marie Curie and RCGP national clinical lead for end of life care
For more information contact rcgp@mariecurie.org.uk
















