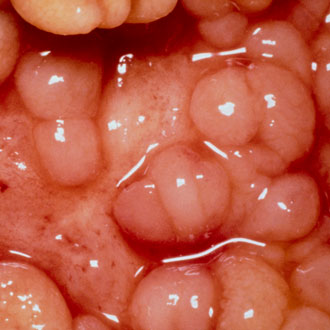
1. The presentation of Crohn’s disease is varied
Crohn’s disease is a chronic inflammatory disease that can affect any part of the gastronintestinal tract from mouth to anus. The area most commonly affected is the terminal ileum followed by the perineum. Terminal ileal Crohn’s disease can mimic acute appendicitis. In this situation, there is often a preceding history of vague abdominal pain. A perianal abscess is a common presentation in general and distinguishing idiopathic perianal abscess from Crohn’s can be very difficult. In some situations, it can take a few years to make the diagnosis of Crohn’s disease.
In addition to these, patients can also present with fatigue, weight loss, and non-specific abdominal pain or even some change in bowel habit. In some situations the diagnosis may be confused with anorexia. The onset of symptoms may precede concrete evidence of bowel inflammation leading to difficulty making the diagnosis
2. Distinguishing Crohn’s disease from irritable bowel syndrome can be difficult
In most patients with luminal Crohn’s disease, the initial presentation is most often with a long history of vague abdominal pain, bloating and a change in bowel habit. These symptoms can be similar to IBS and often diagnosing Crohn’s can be difficult, as even colonoscopy can be inconclusive. In some situations, making the diagnosis can be difficult as the signs of inflammation may not appear until later in the course of the disease. Faceal calprotectin is a simple test that can be very useful in distinguishing between Crohn’s and IBS (see next tip).
3. A faecal calprotectin value of less than 60μg/g can exclude Crohn’s
In the absence of any red flag symptoms, this test has a good sensitivity and specificity to distinguish between inflammatory and non-organic causes. The major advantage is that unnecessary colonoscopy can be avoided, leading to a large cost saving. A faecal calprotectin value of less than 60μg/g of stool could be used to exclude both colonic and small bowel Crohn’s with 96% and 91% negative predictive value, respectively. The type of stool (i.e. diarrhoea) does not have an impact on the result.
4. Management of Crohn’s disease is multidisciplinary
The management of Crohn’s disease requires input from multiple specialities. The medical gastroenterologist forms the core of the decision making unit, but the patient will require support from the inflammatory bowel disease nurses, psychologists, dietitians and surgeons. GPs should also be adequately informed of the patient’s conditions and should form an integral part of the treatment pathway. Difficult cases will be discussed at a multidisciplinary meeting.
5. Most patients with Crohn’s disease will require some form of surgery
Approximately 70% of patients with Crohn’s will require surgery during their lifetime, and about 25% of these patients will require redo surgery. The decision to progress to surgery should be discussed in a multidisciplinary meeting, but the patient should form an integral part of decision making process. Patients’ anxieties relating to surgery should be addressed and the surgery should usually be performed by colorectal surgeons with considerable experience and interest in IBD surgery.
6. The physical location of inflammation is important in determining treatment
Crohn’s disease can affect any part of the body, from the mouth to the anus. The medical and surgical treatment is determined by the primary location of the disease. The main aim of any treatment is to improve a patient’s quality of life and this has to be taken into account in any treatment decisions. The risks of medical treatment have to be worked against any risk of surgery.
7. There are many treatment options for Crohn’s disease and disease activity determines treatment
The main aim of treatment in Crohn’s disease is to achieve mucosal healing, but in most situations this may not be achievable and reducing the disease burden is another aim of disease treatment. Mild disease can be treated with aminosalicylates, and treatment can be escalated to immunomodulators or anti-TNF therapy. Treatment is usually escalated based on disease activity and sometimes surgery is required to treat symptoms. Post-operative treatment is based on the disease activity before surgery.
Anti-TNF therapy is reserved for severe disease. The treatments are effective in most situations, but as the treatments suppress immune function, there are risks associated with the treatments and these should be discussed with the patient. For example, the increased risk of opportunistic infections and the small increased risk of malignancies should be discussed.
8. Treatment for Crohn’s disease can be monitored by calprotectin
Treatment for Crohn’s disease can be monitored by symptoms, inflammatory markers and calprotectin. Calprotectin is very useful for assessing inflammatory burden and response to treatment. The use of calprotectin can reduce the need for radiology and endoscopy. This has the benefit of reducing exposure to invasive procedures and radiation.
9. NSAIDs should be avoided in the management of flares
Early treatment of flares can be associated with a better chance of remission. Flares can present with increasing pain, obstruction, rectal bleeding or a combination of symptoms. Symptomatic management as well as disease management is required to manage a flare. In most situations, steroids can be very successful in treating flares. The dosage of steroids depends on the individual, but 5-10mg daily maybe a good starting dose and this can be escalated if required. Referral to a rapid access IBD clinic may also be beneficial. Dietary modification with low residue or liquid diet can help reduce pain associated with obstruction.
NSAIDs should be avoided in any circumstance. NSAIDS are associated with increasing the severity of the disease, but the exact mechanism is unclear. If started, a plan for reducing the dose of steroids at the appropriate time should be set in place.
10. Smoking cessation is the most important aspect to maintaining remission and reducing flares in Crohn’s disease
Smoking can be associated with increased flare-ups, and in the post-operative setting it is associated with reducing the time to recurrent disease, so smoking cessation is paramount. The pain and stress associated with severe disease can make quitting smoking very difficult. Nonetheless, patients should be offered all possible support to quit smoking and to maintain their some free status.
Mr Janindra Warusavitarne is a consultant colorectal surgeon at The London Clinic and St Marks Hospital