GP beware – vascular
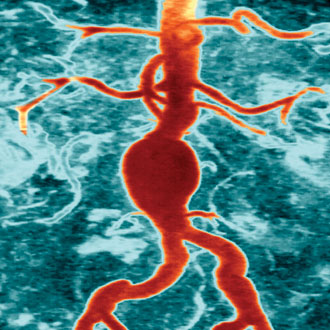
Case 1
Mr H is a 72-year-old with a background history of hypertension, smoking and sciatica, the latter for which he had been treated 20 years ago. He had seen his GP previously for on-and-off back pain that has been treated with oral diclofenac.
On this occasion, he called his GP complaining of the pain being somewhat more severe and not alleviated by anti-inflammatory medication. It was a fairly sudden onset and occurred while he was making breakfast. The GP attended later on in the day, but examination was tricky as the patient was quiet overweight and was unable to lie flat for any length of time.
The GP diagnosis was that of exacerbated lower back pain, and the patent was prescribed co-codamol along with his diclofenac. He was advised that if there was no improvement over the next few days, then he was to call the GP to organise a formal referral to the orthopaedic service.
Over the next 24 hours the pain deteriorated and the patient admitted himself to the local hospital’s A&E department, following which he was transferred to a tertiary vascular service for surgery.
GP’s diagnosis
Musculoskeletal back pain
Actual diagnosis
Leaking abdominal aortic aneurysm
Clues
The patient’s pain was of worsening severity and different in nature from what he had previously experienced with sciatica. In addition, the patient has a background of hypertension, which is the single most important independent risk factor for abdominal aortic aneurysms.
Take home message
Severe back pain in an elderly patient, without any history of injury and with a background of hypertension, should be investigated as a possible symptomatic or leaking abdominal aortic aneurysm, particularly when clinical assessment is thought to be suboptimal. Contained leaks of AAA can linger for days and the patient may not necessarily look systemically very unwell from the outset.
Case 2
Mr G is a 66-year-old ex-smoker, insulin-dependent with diabetes, hypertension and ischaemic heart disease. Over a four-day period he noticed erythema and swelling over his right big toe. In the last 24 hours, the toe has become more swollen and he has been feeling slightly unwell with an episode of cold sweats.
He made an appointment and attended his local GP practice. He was examined by his GP and the toe was identified to be red and swollen, which also included the first metatarsal phalangeal joint. The peripheral pulses were palpable.
The diagnosis of gout was made and the patient had a number of blood tests taken, including uric acid, and was prescribed anti-inflammatories. A further appointment was made for the patient to re-attend the practice in a week.
Over the next 24 hours, the patient experienced a couple of episodes of vomiting and worsening cold sweats, and therefore went to A&E, where he was admitted in hospital for two weeks and received intravenous antibiotics.
GP’s diagnosis
Gout
Actual diagnosis
Diabetic foot sepsis
Clues
The patient has a background of diabetes and had experienced episodes of rigors, which would suggest bacterial sepsis. The fact that he had palpable peripheral pulses does not preclude diabetic foot sepsis.
Take home message
Diabetic foot sepsis should always be considered in patients with diabetes mellitus and inflammatory changes in their feet.
Case 3
Mrs C a 78-year-old lady who developed severe cramp in her right calf while out shopping. The pain radiated into her foot and the symptoms were alleviated when she sat down. The patient went home and found that her symptoms improved when at rest with her foot on the floor, so she decided not to visit the GP.
However, through the night she found that the pain in her foot had become increasingly worse and she ended up sleeping in a chair. By the following morning the foot had become somewhat oedematous and she made an appointment for the GP.
On examination, she was found to have slight tenderness in her calf with weak but present pulses in her foot and reduced movement in her toes. She had a background of ischaemic heart disease and sciatica, for which she was successfully treated before. The diagnosis of musculoskeletal leg pain was made, possibly exacerbated by recurrence of the sciatica, and the patient was offered anti-inflammatory medication and sent home.
Over the next 24 hours, the patient observed the right foot becoming more swollen and much weaker in terms of power. She reached a stage where she was unable to confidently weight bear, and called the emergency services and was taken to the local A&E department. She underwent a number of surgeries, ending with an above knee amputation, and was discharged to the local rehabilitation unit three weeks later.
GP’s diagnosis
Musculoskeletal calf pain, sciatica
Actual diagnosis
Acute leg ischaemia
Clues
The patient is a known arteriopath who experienced sudden-onset pain in the foot with an associated degree of discolouration and reduction in movement. In addition, her symptoms were worsened by the leg being elevated in bed at night (nocturnal rest pain) and alleviated by dependency.
The calf pain on palpation was a sign of acute ischaemia to the calf musculature, as was the reduced movement. Pedal pulses can be very difficult to palpate and the examining physician should always check their own radial pulse, while examining the foot pulses, to ensure that they are not misleading themselves by perceiving transmitted pulses from their fingertips as the patient’s pulses.
Take home message
Acute-onset calf pain in a known arteriopath with or without a history of nocturnal rest pain should be urgently investigated as an acute ischaemic event.
Mr Constantinos Kyriakides is a consultant vascular surgeon at The London Clinic and Barts Health NHS Trust
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









