Non-Covid clinical crises: Very severe eczema in children
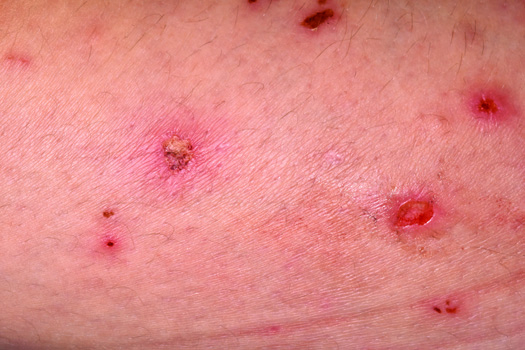
Children (and their families) with very severe eczema are typically desperate and miserable.
Firstly, when managing the condition, it is important to get the basics right. This includes:
- A tepid bath for 10-15 mins every day which can be soothing, distracting and hydrates the skin
- Make sure to avoid ALL detergents (no soap, shower gel, bubble bath or shampoo at all)
- Balneum Plus bath emollient (two capfuls in 8 inches of water) can be soothing and helps to relieve itching
- Wash with any emollient, gently stroking onto skin before getting into water). Parents should be made aware that emollients can make the bath/shower/child very slippery
- After the bath dab the skin gently dry (don’t rub) and apply more emollient by stroking it gently down the body and limbs)
- Apply emollient of choice at least two to three times a day remembering that the whole skin is abnormal, not just the apparently affected areas
- Avoid contaminating ointments by extracting from pot with fingers and instead use a spoon
Treatment
It is worth starting with a potent topical steroid ointment applied to all the affected areas, just once a day (ideally at bedtime). For example, starting with clobetasol proprionate (Dermovate) for a day or two if very severe but dropping down the steroid ladder as the condition improves to Elocon for one to two weeks followed by Eumovate, etc.
If you find the eczema is settling, be careful not to stop abruptly but taper off gradually. One option is to use weekend therapy applying a topical corticosteroid to affected skin on just two days a week (usually Saturday and Sunday) for two to four weeks after the eczema has settled.
Consider giving advice using fingertip units – one unit of ointment (0.5gms) covers the area of two adult palms and ensure patients have sufficient quantities and know how much to apply.
The child may need different potency ointments for different areas, for example, mild to moderate on face but moderate or potent for the body.
Ideally there should be a 30-minute interval between applying emollient and topical steroids.
Topical immune modulators (Elidel or Protopic) are excellent but can sting initially. Use should be discussed with a dermatologist.
Infection
All flares of eczema are infected. Infection also often triggers a flare. But unless the child is ‘ill’, or has widespread crusty lesions, do not use antibiotics orally or topically.
Antiseptics can be helpful, for example washing with Dermol lotion and leaving some Dermol cream on as a leave-on emollient. But DO NOT continue this for more than a few days.
Be aware of eczema herpeticum (sudden appearance of small, similar looking punched-out eroded areas, usually on the face). Patient can become ‘ill’ quickly. Discuss with a dermatologist and consider early use of aciclovir.
Itch
This is the nightmare for patients and their families and treating the eczema is the best treatment.
Antihistamines usually don’t help and non-sedating antihistamines are very unlikely to be helpful. If sleep is a massive problem, sedation may give everyone a break, but a sedating antihistamine, eg, chlorpheniramine or hydroxyzine won’t relieve much itch.
Balneum Plus cream or E45 itch relief cream are worth a try and Adex gel would also be a sensible choice.
Oral treatments
Oral steroids could provide relief, but usually are usually only used short term. Discuss with a dermatologist who may also recommend methotrexate etc. This needs monitoring regularly and neither of these is a great option during COVID-19 pandemic.
Given that children with severe eczema are vitamin D deficient, oral vitamin D supplementation is a really good idea. It has been shown that this can help bring severe eczema back under control.
If it is not settling, review
Is the patient not adhering to your treatment? Consider an allergy including ongoing allergic stimulus or even new allergy to treatments? Is the diagnosis wrong? What about infection?
Dr George Moncrieff is a GP with a special interest in dermatology based in Oxford
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.










