Exclusive Prescriptions for vitamin D have risen 40% over the past four years in England, leading some experts to warn that testing and treatment is ‘out of control’, a Pulse investigation has revealed.
The rise has happened since the Government’s chief advisor sent out a warning that one in four people are deficient in vitamin D and that GPs should advise certain at-risk groups to take a daily supplement.
This is despite experts questioning the effectiveness of putting people on vitamin D, warning that it is risks overmedicalising the population.
A Pulse analysis of official figures show that GP prescriptions for vitamin D have risen steadily year on year from 14 million items in 2012, to 20 million items in 2015.
The cost to the NHS has shot up accordingly, from a stable cost of around £4.8m a month before 2012 to £7.1m in the latest figures from last November.
The total NHS spend on vitamin D last year was around £85m.
GP experts said the publicity around vitamin D has driven some of the rise in GP prescribing and warned that in some cases it was uncertain whether it would be better to simply advise people to get out more in the sun and eat a better diet.
Dr Andrew Green, chair of the GPC’s clinical and prescribing subcommittee, said: ‘There has to be some concern that patients are being medicated when lifestyle changes may be more appropriate.’
However leading GP critics also warned a sharp rise in testing for vitamin D levels for non-specific symptoms was leading to pressure on GPs to prescribe more and more vitamin D even though there was no evidence it would offer any benefit.
In line with this, data obtained by Pulse through Freedom of Information requests showed that requests for vitamin D testing – which can cost as much as £20 each time – have increased by up to 115% in some trusts over the four-year period.
Dr Alun Cooper, a GPSI in osteoporosis in Sussex and a member of the National Osteoporosis Society Scientific Committee and the National Osteoporosis Guideline Group, said: ‘The prescribing of vitamin D seems to have gone out of control.
‘We need to prescribe when clinically indicated, for example in osteomalacia, and not just treat a blood test result.’
But Dr Sally Hope, a recently retired GP from Oxford who works as an associate specialist for Oxford University Hospitals’ osteoporosis service at the Nuffield orthopaedic centre, said she believes that despite the rise in prescriptions there are still not enough people receiving vitamin D supplements – particularly the elderly and those diagnosed with osteoporosis.
She said: ‘I actually don’t think it’s anywhere nearly enough prescribing in older people. Virtually every person that comes in with a fractured hip to hospital is vitamin D deficient.’
Government experts recently indicated they want more blanket advice on boosting vitamin D, raising the potential for even more use of vitamin D pills.
However, it remains unclear what their final recommendation will be and whether a strategy to expand supplementation would include offering advice and prescriptions via GPs, or focus on food fortification schemes.
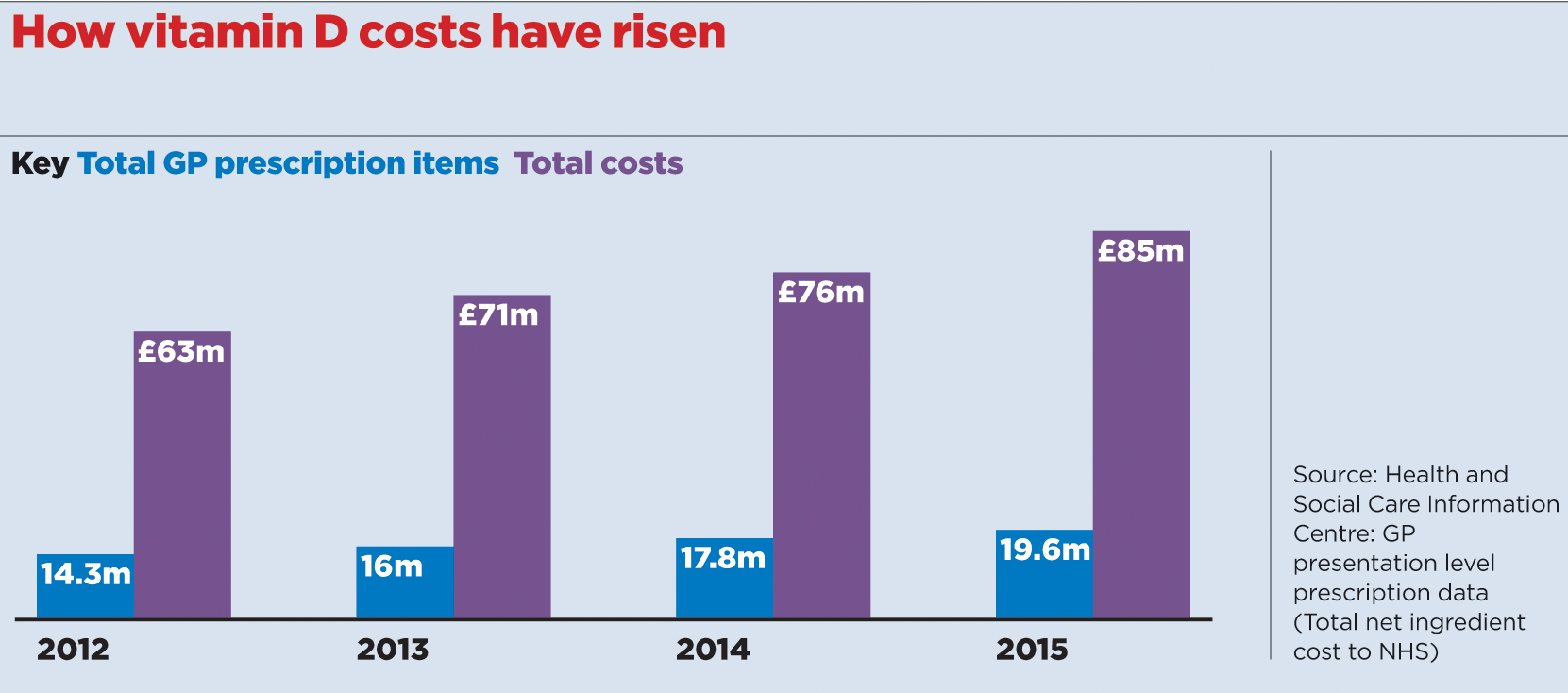
Vitamin D investigation figures
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.











