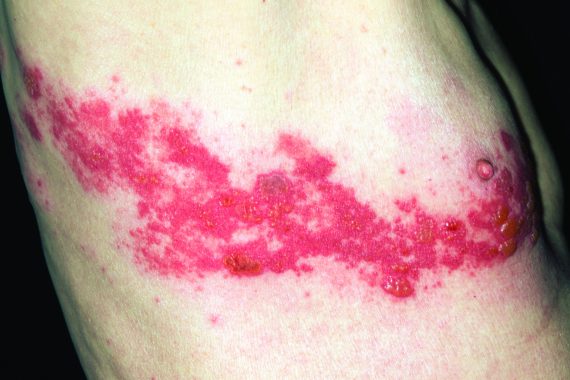
Shingles vaccine cuts cases by a third
Public Health England has urged GPs to encourage eligible patients to have the shingles vaccine after a study showed the vaccine cut cases by a third between 2013 and 2016.
The study looked at patients registered at a geographically representative selection of GP surgeries. It found the incidence of shingles reduced by 35% in the three years following the introduction of the vaccine in 2013 for those aged 70, with incidence of postherpetic neuralgia falling by half. This corresponded to 17,000 fewer cases of shingles and 3,300 fewer cases of postherpetic neuralgia between 2013 and 2016.
The paper concludes: ‘Given the demonstrated impact of the programme on herpes zoster and postherpetic neuralgia, the benefits of the programme need to be effectively communicated to health professionals and the public to maximise protection from this potentially debilitating condition in those most at risk.’
PHE has reported a decrease in uptake of the vaccine since its introduction in 2013, and has urged GPs to encourage eligible patients to be vaccinated.
GP screen ‘could avert 28% of hip fractures’
Screening for osteoporosis in GP practices could prevent more than a quarter of hip fractures in older women, according to a UK-wide study.
The study involved just under 12,500 women aged 70-85 and found that the FRAX questionnaire, combined with bone density measurements for some, helped GPs identify those at risk of hip fracture and allowed patients to be targeted for treatment. This led to a 28% reduction in hip fractures over five years.
Of those screened, treatment was recommended for one in seven women deemed at high risk. GPs acted on the recommendations and more than three-quarters of those women were on osteoporosis medication within six months of screening.
The study suggests one hip fracture could be prevented for every 111 women screened, and early results indicate the approach is likely to be cost effective.
Lead researcher Professor Lee Shepstone, from the University of East Anglia’s Norwich Medical School, said: ‘This is the first trial to show that a community-screening approach based on the FRAX fracture risk tool is both feasible and effective… the results of this study potentially have important public health implications.’
The Lancet 2017, online 15 Dec
Genetic risk scoring ‘may help PSA screen’
A personalised genetic score has been developed for predicting a man’s risk of developing aggressive prostate cancer and guiding doctors on whom to offer PSA testing, researchers have found.
An analysis of 200,000 gene variants was carried out from more than 31,000 men with and without prostate cancer.
A risk score was developed based on 54 variants associated with an increased likelihood of prostate cancer, before being tested in a clinical trial of 6,400 men.
Results showed the score was a highly significant predictor of age at diagnosis of aggressive cancer, with men who scored in the top 2% having an almost three-fold greater relative risk of aggressive prostate cancer compared with those with average risk.
The researchers concluded: ‘This genetic risk model might play a role in guiding decisions about whether and when to screen for prostate cancer.’
A&E attendance ‘not driven by GP access’
Multimorbidity, not a lack of access to GP appointments, may be responsible for the year-on-year increases in A&E attendances, a study has found.
The study looked at records for just under 820,000 patients registered at GP practices in 2013 and found that a higher number of visits to the GP was a strong predictive factor for A&E attendance. Patients with one or more long-term conditions were also more likely to go to A&E, with patients who had four or more conditions showing a six-fold increase in attendance rates.
The researchers said in the paper: ‘Patients with more attendances at A&E also have higher GP consultation rates. This suggests that the year-on-year rise in A&E attendance is not primarily accounted for by poor access to primary care, but rather by increased patient complexity and longevity.’
They concluded: ‘These findings are an important contribution to the continuing debate on whether patient care will benefit from reducing A&E units and replacing them with community-based support.’
Volatile patients ‘key factor’ in GP burnout
Emotionally draining patient consultations are a key contributing factor to GP stress and burnout, a study has found.
The study was based on in-depth interviews with 47 GPs in England, including some who had experienced burnout or mental distress.
Doctors who got support from colleagues fared better, the research found, but some confided that it was distressing to deal with confrontational patients.
One respondent said that there had been no time for reflection at her practice following a colleague’s suicide after a bout of depression.
Internal practice conflict and bullying from colleagues were also cited as sources of stress.
The researchers said: ‘The sources of stress and distress cannot solely be attributed to increases in workload and occupational stress linked to the work role demands of being a GP.’
They said GPs should have ‘a safe space’ where they can deal with these causes of stress.
The research comes after the NHS England-funded GP mental health service was inundated with demand upon its launch one year ago.
Professor Clare Gerada, the medical director of the GP Health Service and who helped with recruitment to the study, said: ‘The cause of distress is fundamentally that we are unable to meet the demands.’
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens