The patient’s unmet needs (PUNs)
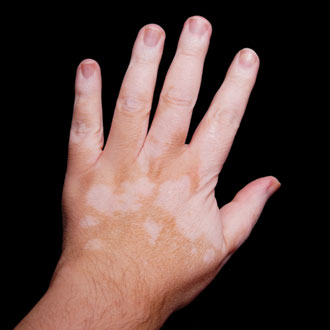
A 22-year-old man attends in a state of distress. ‘I need you to do something about this vitiligo,’ he says. ‘I’ve had it for two years now and I just keep getting fobbed off with creams.’ It transpires that, since he started a new job, he’s become increasingly self-conscious and depressed about his problem. ‘Is it definitely vitiligo anyway?’ he asks. ‘I’ve not seen a specialist. And I’ve read it can be linked to other diseases – but I’ve not had any blood tests to check them out.’
The doctor’s educational needs (DENs)
How can the GP make a definite diagnosis of vitiligo? With what other skin conditions could it be confused?
Vitiligo usually presents as a complete depigmentation of areas of the skin. The condition can affect white-skinned patients as well as those with darker skin types. In white-skinned patients, the condition may become apparent after a sunny holiday, whereas in darker skin types the contrast between affected and unaffected skin is often readily apparent. Children, in addition to adults, can also present with vitiligo.
Major clues to making the diagnosis are the degree of depigmentation and the distribution of the pale patches. In vitiligo, we expect the affected skin to be completely white, like a sheet of paper, with a smooth, normal surface. The classically affected areas are periorbital, perioral, digital tips and genital, although much larger areas can be affected. Occasionally, vitiligo can present in a localised area of skin – this is termed segmental vitiligo and is thought to be a form of mosaicism, which is localised variation in gene expression, perhaps caused by a post-zygotic mutation.
If the skin is paler, but not completely white, the presentation is less likely to be vitiligo, unless it’s a very early case, or a spontaneously repigmenting patch. More likely, the patient has another explanation for the hypopigmentation – commonly post-inflammatory after a process such as eczema. This is commonly a diagnostic issue with children who have developed pale patches during or after eczema. The rough surface of the skin, a history of itch and scale and the lack of complete depigmentation help differentiate the two.
Other than eczema, another common condition causing slightly scaly, hypopigmented patches, particularly on the chest and upper back, would be pityriasis versicolor. This can be diagnosed clinically by the very fine scale, which can also be sent for fungal testing after a gentle scraping.
A more serious condition, cutaneous T-cell lymphoma, can also present with pale, slightly scaly patches in children and adults. These have an atrophic quality, with the skin often having a crinkled, cigarette paper quality. In this condition, the patches of hypopigmentation are not distributed in the distribution of classical vitiligo, but are more randomly spread and tend to be 1-2cm in diameter.
In a patient with hypopigmentation that is not classical of vitiligo, and does not improve with emollients and mild topical steroids, a skin biopsy should be considered to look for evidence of lymphoma, although the patient may appear to be clinically well. Another consideration, particularly in endemic areas, would be leprosy.
How common are associated psychological problems like anxiety and depression?
Vitiligo can have a considerable impact on the psychological and social well being of patients, in all affected races. It is often assumed that white-skinned patients will be less concerned about depigmentation, but this is not the case.
The impact on the patient is a complex mixture of cultural and social pressures and their own sense of self-worth. In arranged marriage cultures, there can be difficulties with arranging a successful match and patients will often present to the GP when such an event is on the horizon. Studies demonstrate that the psychological impact can affect both the parents and the affected child, and vary from patients with vitiligo on exposed sites versus hidden sites.
Vitiligo patients are more likely to suffer from anxiety, depression, emotional stress and low self-esteem.
What other diseases is vitiligo associated with? Should the patient have blood tests for these – and if so, how often?
About 10-15% of vitiligo patients will develop autoimmune disease, compared with a population prevalence of about 1-2%. A wide range of autoimmune diseases have been linked, but in practical terms, thyroid disorders are the most common. Other notable associations are type 1 diabetes and the polyglandular syndromes. It is worth screening for thyroid disease and diabetes. Other autoimmune diseases can be investigated based on the clinical presentation.
What self-help measures can be advised – and what is the prognosis?
Patients are able to use cosmetic camouflage – it is worth recommending charities such as Changing Faces (see further reading) to support this as patients can receive helpful information on waterproof camouflage, sunscreens and a better match to their skin colour. Often, patients will think they have tried camouflage based on advice from a make-up counter, but a professional camouflage artist is far better placed to meet the needs of these patients and excellent results can be achieved.
As vitiligo can be induced by trauma, it is important to avoid injuries to the skin surface. It is advisable to maintain good skin condition with mild cleansers and regular moisturising to ensure the skin is resilient to trauma and inflammation.
What treatments are available and how effective are they? Which can the GP initiate and which require referral to a dermatologist?
Available treatments range from meeting the psychological needs of the patient through to camouflage, and careful attempts to match the skin colour.
Treatments to improve the skin colour match are usually dictated by the extent of the disease. Small patches can be treated with topical calcineurin inhibitors, which are unlicensed and can be prescribed by GPs who are confident in their diagnosis. They can also be treated by potent, very potent or super-potent topical steroids.
Often, facial and neck lesions will respond well to topical calcineurin inhibitors without significant adverse effect. However, these can be associated with herpes reactivation, particularly around the mouth or genitals.
A potent topical steroid may be the next step, but caution needs to be exercised around the eyes as they can increase ocular pressure, and around the mouth, again because of herpes reactivation, and also a rosacea-like condition known as periorificial (around either the eye or mouth) dermatitis.
More extensive disease can be treated with light therapy in a secondary care setting, to treat the whole body. This can be either UVB or PUVA treatment – both require many months, two or three times per week, so they suit only the patients who can commit to such a programme. Although physicians may see the results as a patchy improvement, patients are often very happy to see some return of pigment. We often find that this helps them move on with their lives.
A small number of patients will request depigmentation with monobenzyl ether of hydroquinone. This can affect liver function and requires specialist supervision. It is applied as a topical cream and gradually depigments the skin to an even white shade, over about two years, working from one body site to the next. Some patients may just treat the face and hands, while others will seek a whole body treatment.
Surgery is now becoming a more realistic option for patients. Those with stable vitiligo can have some kind of skin grafting – commonly, a punch graft or an epidermal blister graft, into a visible area around the eye or mouth. Each area will require multiple grafts to bring melanocytes into the local skin, which then migrate to fill out the patch.
One of the newest approaches is a keratinocyte/melanocyte harvest from a patch of skin, which is sprayed onto an abraded area of vitiligo. Followed by phototherapy, this has shown impressive results in trials with repigmentation and colour match. The fingertips, however, tend to remain refractory, perhaps because of repeated minor trauma.
Key points
• Vitiligo is characterised by complete depigmentation of a patch of skin.
• It is associated with thyroid disease and type 1 diabetes.
• There is a significant impact on psychosocial and sexual function and social stigma may be an issue.
• Camouflage is very helpful.
• Topical treatments are good for localised areas.
• Generalised skin involvement is best treated with phototherapy.
• Surgical/grafting technologies are reaching clinical practice for stable disease.
Dr Saqib J Bashir is a consultant dermatologist and dermatological surgeon at The London Clinic and King’s College Hospital, London.
Pulse Writing Competition 2024
Take our September 2024 survey to potentially win £200 worth of tokens