Advising patients who self-monitor their blood glucose

Clarity is required with regards to self-monitoring for patients with diabetes – in particular, which patients require it and which ones do not. The cost of test strips for the NHS in 2010 was around £150m, and appears to be on the rise.¹ Knowing which patients do not require self-monitoring and who can safely be managed with regular HbA1c testing alone could potentially make a significant saving. There is no doubt that patients treated with insulin must self-monitor, but there often tends to be confusion about self-monitoring in diabetes patients who are on oral or non-insulin medications.
The new NICE guidelines for the management of type 2 diabetes in adults states that blood glucose monitoring should not be routinely offered unless:
• The patient is on insulin.
• The patient has had hypoglycaemic episodes.
• The patient is on oral medication that can predispose to hypoglycaemia while operating machinery or driving.
• The patient is planning to become pregnant or is pregnant.
• Short-term self-monitoring may be considered if the patient is receiving treatment with oral or IV steroids, or to confirm possible hypoglycaemia.
1. Patients who are diet controlled do not need to self-monitor.
Diabetes patients who are diet controlled, and those on oral hypoglycaemic agents with a low risk of hypoglycaemia, for example, patients on metformin, glitazones, DPP-4 inhibitors, SGLT2 inhibitors or GLP-1 agonists, do not require self-monitoring.³,⁴,⁵ These patients can be managed with HbA1c testing on a three to six-monthly basis.
The DIGEM study (diabetes glycaemic education and monitoring) was a four-year randomised trial to see if self-monitoring alone, or in addition to self-care education, is more effective than usual care in improving glycaemic control, in 453 patients with type 2 diabetes not on insulin. After four years, there was no significant difference in HbA1c in all three groups. A cost analysis revealed that intensive self-monitoring in diabetes patients not on insulin doubles the net cost of the intervention, with no benefit in glycaemic control.
There have also been several RCTs that have shown that self-monitoring in type 2 diabetes patients who are diet controlled or on oral medication alone is not clinically effective.⁷
A Cochrane review found that the effect of self-monitoring of blood glucose on glycaemic control in type 2 diabetes patients who are not using insulin is not clinically significant after 12 months. Also, this study concluded that there was no evidence that self-monitoring of blood glucose affected patient satisfaction or general wellbeing.⁸
2. Self-monitoring may be required up to three times per week in type 2 diabetes.
For type 1 diabetes patients, the NICE guidelines advise:⁹
• Patients should self-monitor their blood glucose at least four times a day, before meals and before bed.
• Adults with type 1 diabetes can be supported to test up to 10 times a day if the HbA1c target remains high or if hypoglycaemic episodes increase – before driving, during sick days, pre-conceptually, or if pregnant or breastfeeding, or if the patient has a lack of hypoglycaemic awareness.
For type 2 diabetes patients, routine self-monitoring should be available in the following groups:
• Type 2 diabetes patients receiving sulfonylureas or glinide therapy should test to ensure they are not having hypoglycaemic episodes. Initially, testing may be required up to three times a week,¹⁰ but this could increase if there is intercurrent illness, exercise or change in lifestyle. Once the blood glucose is stable, HbA1c testing should be the mainstay of monitoring.
• Patients on basal insulin treatment, with or without oral hypoglycaemics, should have fasting blood glucose checked before breakfast while the basal dose is being adjusted, then once a day at other times to establish the variation of blood glucose throughout the day. The need for self-testing may increase if there are lifestyle changes or intercurrent illness.
• For those patients who are on multiple insulin injections, self-monitoring should be as per type 1 diabetes – at least four times a day, which may need to increase during times of illness or physical activity.
For pregnant women with diabetes:
• For diabetic women who wish to become pregnant, pre-conceptual advice is imperative. The risks of miscarriage, stillbirths and congenital malformations are reduced if pre-conceptual glucose control is optimised. The NICE guidelines recommend that women with diabetes who are planning a pregnancy should aim for an HbA1c of below 6.5%.¹¹ Women whose HbA1c level is above 10% should avoid becoming pregnant.
• These women should be offered a meter and blood glucose strips to monitor their glucose levels in order to maximise their control before becoming pregnant, even if their diabetes is diet controlled.¹¹
• Pregnant women with type 1 diabetes or type 2 diabetes treated by multiple daily insulin injections should test fasting, pre-meal, one hour after meals and bedtime blood glucose levels daily. Type 2 diabetes women who are pregnant, or those with gestational diabetes, should check fasting glucose levels and one hour after every meal. This is the case for patients who are both diet controlled or on oral hypoglycaemics, or on single daily doses of intermediate or long-acting insulin. During pregnancy, the fasting glucose levels should be kept below 5.3mmol/l (as long as hypoglycaemia is avoided), one hour after meals <7.8mmol/l and two hours post meals <6.4mmol.¹¹
3. Test blood sugars every two hours while driving.
The DVLA advises that in insulin-treated patients who drive cars or motorcycles, blood sugar should be tested no more than two hours before the start of the first journey and every two hours while driving. In insulin-treated patients who drive LGVs or passenger-carrying vehicles, twice-a-day glucose monitoring should be undertaken and at times before and during driving. A glucose meter should be carried with a memory function.
• In patients on oral hypoglycaemics, which may cause hypoglycaemia (such as sulfonylureas or glinides), self-monitoring may be required in those who drive cars or motorcycles. These patients must be under regular medical review.
• In type 2 diabetes patients on sulfonylureas or glinides who are drivers of LGVs or passenger-carrying vehicles, self-monitoring should be performed at least twice a day and at times relevant to driving.
You could reduce the cost of prescribing test strips by more than 30%.⁴
Significant savings can be made by practices by rationalising the choice of test strips and glucose meters prescribed. There are many glucose meters and test strips on the market, and it can be confusing for providers to get a grasp of all of these.
By prescribing strips and meters from a chosen formulary and by switching to more cost-effective brands (less than £10 for a box of 50 strips), a practice can make great savings. The cost of prescribing test strips could be reduced by 31% if there is a 100% switch to issuing more cost-effective strips.¹³
Placing test strips on the ‘acute medication’ list can be a useful compromise to stop self-monitoring.⁵ Patients will find it useful to know that there is clinical evidence to support HbA1c testing alone as an effective way of monitoring blood glucose in certain patient groups.
They should also be informed that there could be disadvantages to self-monitoring blood glucose, if this is not deemed necessary, and could cause unnecessary harm (see table).
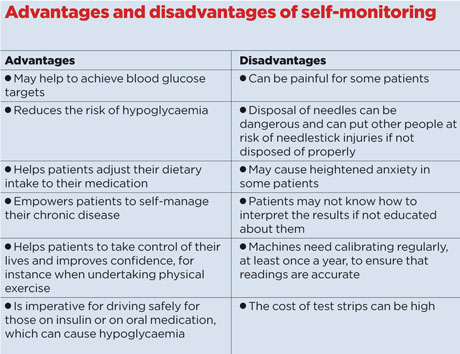
For patients who take oral medication or are diet controlled and who are keen to self-monitor, a compromise could be that prescriptions for test strips are placed on the ‘acute medication’ list and not on repeat medications.
This could prevent excessive testing in this group and an annual review of the need for self-monitoring could be performed in a structured way, to assess whether self-monitoring continues to be necessary.
Key points
• Intensive self-monitoring of diabetes patients not on insulin doubles the cost with no benefit in glycaemic control
• Patients who are diet controlled, or on oral agents with a low risk of hypoglycaemia do not require self-monitoring
• Instead, these patients can be managed with three to six-monthly HbA1c testing
• Self-testing is imperative for safe driving in those on insulin or oral medication that can cause hypoglycaemia
Dr Tina Farid is a GP with an interest in diabetes in north London
References
1 Diabetes Position Statement. Self-monitoring of adults with type 2 diabetes. London: Diabetes UK; 2013
2 NICE. NG28: Type 2 diabetes in adults: management. London: NICE; 2015
3 Fowler MJ. Diabetes treatment, part 2: oral agents for glycaemic management. Clinical Diabetes, 2007;25:131-134
4 Nauck MA. Update on developments with SGLT2 inhibitors in the management of type 2 diabetes. Drug Des Dev Ther, 2014;8:1335-80
5 Prasad-Reddy L, Isaacs D. A clinical review of GLP-1 receptor agonists: efficacy and safety in diabetes and beyond. Drugs Context, 2015;4:212283
6 Farmer A, Wade A, Goyder E et al. Impact of self-monitoring of blood glucose in the management of patients with non insulin treated diabetes. BMJ, 2007;335:132
7 NHS Diabetes Working Group. Self-monitoring of blood glucose in non-insulin treated type 2 diabetes. Aberdeen: NHS diabetes; 2011
8 Welschen LM, Bloemendal E, Nijpels G et al. Self-Monitoring of blood glucose in patients with type 2 diabetes mellitus who are not using insulin. Cochrane Database Syst Rev, 2012;2:CD005060
9 NICE. NG17: Type 1 diabetes in adults: diagnosis and management. London: NICE; 2015
10 Owens D, Barnett AH, Pickup J et al. Blood Glucose Monitoring in type 1 and type 2 diabetes: reaching a multidisclipinary consensus. Diabetes and Primary Care, 2004;6:8-16
11 NICE. NG3: Diabetes in pregnancy, management of diabetes and its complications from pre-conception to the post natal period. London: NICE; 2015
12 DVLA. At a glance guide to the current medical standards of fitness to drive. Swansea: DVLA; 2014
13 Ekuban B. Blood glucose test strips for patients with type 2 diabetes mellitus. Prescqipp, bulletin 46; 2013
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.



 Oviva’s fully remote Tier 3 Weight Management programme
Oviva’s fully remote Tier 3 Weight Management programme







