How to spot zebras – Kawasaki disease
What is it?
Kawasaki disease is an increasingly common, acute, systemic vasculitis of medium-sized muscular arteries that typically affects children – 85% are under five years, but it can affect any age. It affects boys more than girls and the major complications are coronary artery aneurysms (CAA), which are life-threatening and seen in over a quarter of those who are not treated early enough.
Consequently, there is a higher risk of myocardial infarction, aneurysm rupture, coronary artery thrombus formation and sudden cardiac death, even 20 years after the acute illness. Previously it was thought to be rare, but a recent British Paediatric Surveillance Unit study showed that 80% of 553 children over a two year period were brought to their GP with non-specific symptoms at an average of two days into the illness. This gives the GP an opportunity to review such children, perhaps more than once, and consider the diagnosis during this time so that at five days, treatment can be given. Since late treatment for this condition is associated with CAA formation, it is of vital importance that such children are recognised early and treated.
Prevalence
In developed countries, Kawasaki disease has overtaken rheumatic fever as the leading cause of acquired heart disease in children. The rate of Kawasaki disease has steadily increased, increasing four-fold in the UK over the last 10 years, and is now around eight in 100,000 by the age of five years.
This article therefore aims to highlight this risk to the GP, although not recognised as commonly as slapped cheek and scarlet fever. It can be more common than meningitis, which everyone is on the lookout for! It is most often seen in winter months between October and March and is also more likely in rural areas.
Presentation
The main problem with diagnosing Kawasaki disease is that there is no blood test or other test to make a definitive diagnosis. Instead, the diagnostic criteria of complete Kawasaki disease are the presence of a persistent fever lasting five days or more and at least two of the following five criteria. It is often called the ‘red disease’:
- Red eyes: bilateral, painless, non-exudative conjunctivitis.
- Red rash: polymorphous exanthema.
- Red lips/tongue: changes in lip or oral mucosa, commonly present as red, cracked lips, ‘strawberry tongue’ or generalised diffuse erythema of the oropharynx.
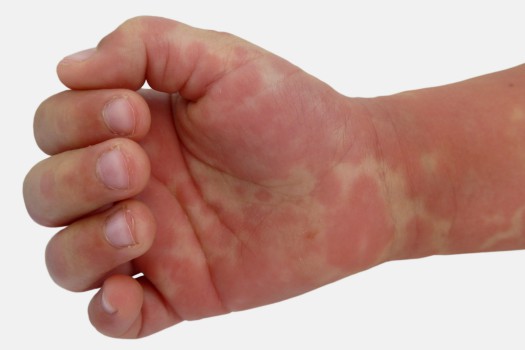
- Red fingers: changes of the extremities, particularly erythema and oedema of the palms and soles of the feet, this can progress later to desquamation of the skin.
- Cervical lymphadenopathy: classically larger than 1.5cm and commonly unilateral.
- Children are often very irritable and inconsolable.
Incomplete Kawasaki disease may be seen, with very few of the criteria in addition to fever. Detection of coronary artery dilatation or aneurysm on echocardiography requires only a fever and two of the criteria to make a diagnosis of atypical Kawasaki disease. In fact, it is one of the most important diagnoses to consider in an infant, with unexplained persistent fever, even if only two of the features are present and there is no other explanation. It is clear that the GP will see many children with some of the symptoms, but it is not common to have an unexplained fever for five days. A proper history from the parent is important since the signs and symptoms of this condition develop over a few days, usually without all the symptoms being present at the same time and tending to come and go.
Differential diagnosis
The differential includes childhood infections, such as streptococcal disease (scarlet fever), parvovirus (slapped cheek) and other viral infections. Alternatively, juvenile rheumatoid arthritis can initially present in a similar manner but tends to have arthritis as a major feature. The joints may be sore in Kawasaki disease but are not often acutely swollen and hot and tender. However, nothing else causes a persistent fever for five days without obvious cause. If antibiotics are given for a bacterial infection, it would be expected that the fever would resolve within 48 hours. The episode of Kawasaki disease is triggered often by another infection and diagnosis is made more difficult in that most normal children have streptococcus in the throat swab, and this can be coexistent with Kawasaki disease. Desquamation of the fingers occurs late in Kawasaki disease, after any damage has occurred to the coronary arteries, and should not be used to make the diagnosis.
Investigation
The most important aspect of Kawasaki disease is to include it in your differential diagnosis, especially in an infant who is a boy. Blood tests can be helpful in the emergency department, with a very high CRP, high white count, low albumin, low platelet count and anaemia being most prevalent in the worst cases. Sometimes liver function tests can be also abnormal. Throat swabs should not be taken, to avoid confusion.
Diagnosis
It is critically important to suggest the diagnosis of Kawasaki disease and to refer to the hospital in a child with persistent fever. Recent studies show that over 80% of such children are seen by the GP at two days into the illness and again a day later, such that if this is still present at five days, with no other obvious cause, there is timely opportunity to make the diagnosis. The most clinically significant complication is the vasculitis of coronary arteries, leading to CAA.
Early treatment with intravenous immunoglobulin at diagnosis, at five days of fever, leads to a regression of coronary artery aneurysms in most cases. In the UK, many cases are missed so that 28% of children have cardiac involvement. Some patients develop giant coronary artery aneurysms (often 1cm across or more), which carry the worst clinical prognosis. These often result in myocardial infarction, ischaemic heart disease and sudden cardiac death in patients, sometimes many years later and are a recognised cause of premature myocardial infarction in young adults. If there is CAA present, then children will be treated with low dose aspirin in the longer term, sometimes with the addition of clopidogrel or even warfarin in those where the aneurysm is giant.
There is now evidence that those children who had small or medium CAAs that shrank in size should be followed up in the longer term. They will be seen in the local Kawasaki clinic (or paediatric cardiology clinic) where they will undergo echocardiography, angiography, MRI scans and stress testing.
Kawasaki disease in adulthood
There has been no formal collection of data regarding the number of adult patients with a previous history of Kawasaki disease in the US or the UK. Estimates are that approximately 24,000 young adults (>18 years) in the US have had complications from Kawasaki disease, with 8,400 of these patients classified at an AHA risk level II or higher. Estimates for the UK have not yet been published but it appears that about 4% of young adults presenting with myocardial infarction have coronary angiograms indicative of previous Kawasaki disease. Although coronary artery aneurysms are the main complication, other cardiovascular abnormalities should also be investigated: myocarditis and valvulitis has also been observed in Kawasaki disease patients. Myocardial fibrosis and aortic and mitral regurgitation can follow and lead to death. Due to the growing rate of diagnosis, cardiologists will be dealing with adult patients who have long-term sequelae from this condition for many years to come.
Professor Robert Tulloh is a consultant paediatric cardiologist at the Bristol Royal Hospital for Children. Dr Louise Tulloh is a GP in Bristol.
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









