Genetics may play larger role than diet for developing gout, says study
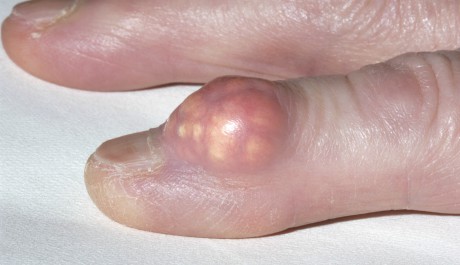
Genetics may play a larger role than diet in the development of gout, researchers have suggested.
Diet accounted for only a small proportion of variation in serum urate levels in a recent meta-analysis, challenging the widely held belief that gout is caused primarily by diet.
The study was carried out by researchers in New Zealand and looked at several different studies, including just under 17,000 men and women of European ancestry who didn’t have gout and weren’t taking urate-lowering drugs.
Patients enrolled in the studies completed dietary questionnaires, had their serum urate levels measured and had genetic profiles recorded.
The researchers looked at serum urate levels for the cohort and used statistics to determine how much of the variation in urate levels was due to either food or genetic variants.
They found that foods such as beer, lamb, potatoes, poultry and soft drinks were associated with increased serum urate, but that these foods accounted for less than 1% of variation in urate levels.
They also found that genetic factors that affect urate levels accounted for just under 25% of the variation.
They said in the paper: ‘Our data are important in showing the relative contributions of overall diet and inherited genetic factors to the population variance of serum urate levels.
‘Our results challenge widely held community perceptions that hyperuricaemia is primarily caused by diet, showing that genetic variants have a much greater contribution to hyperuricaemia in the general population than dietary exposure.’
Keele University researchers pointed out in a linked editorial that patients with gout faced stigma due to the societal perception that gout is caused by an unhealthy lifestyle and so were less likely to seek help and receive treatment.
They said: ‘The study… provides important evidence that much of patients’ predisposition to hyperuricaemia and gout is non-modifiable, countering these harmful but well-established views and practices and providing an opportunity to address these serious barriers to reducing the burden of this common and easily treatable condition.’
BMJ 2018; available online 10th October
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









