Patients hit by practice closures: the thousands who have had to find a new GP


GP leaders have been warning that many practices are on the brink of closure.But now Pulse can reveal that more than 160,000 patients across the UK were displaced as a result of their practice closing in just two years.
This is not only distressing for patients, but also piles the pressure on neighbouring practices, which are often forced to take on additional patients. And GP leaders say they expect the number of closures to climb further over the next year.
Pulse has been campaigning for additional support for struggling practices in its Stop Practice Closures campaign, and there are signs NHS managers are finally starting to listen. But this will come too late to help the thousands of patients whose practices have lost the fight to survive.
GPC chair Dr Chaand Nagpaul believes the figures obtained by Pulse are the ‘tip of a much bigger iceberg’.
He says: ‘There are many practices on the brink of collapse, while others may not be closing, but are significantly reducing the level of services they can offer. We have many practices running at half capacity and having to reduce the number of sessions.’
Dr Nagpaul adds: ‘There needs to be a national, proactive approach to support general practice to pre-empt and prevent this sort of issue occurring. Far too often it is a case of trying to make amends after the event.’
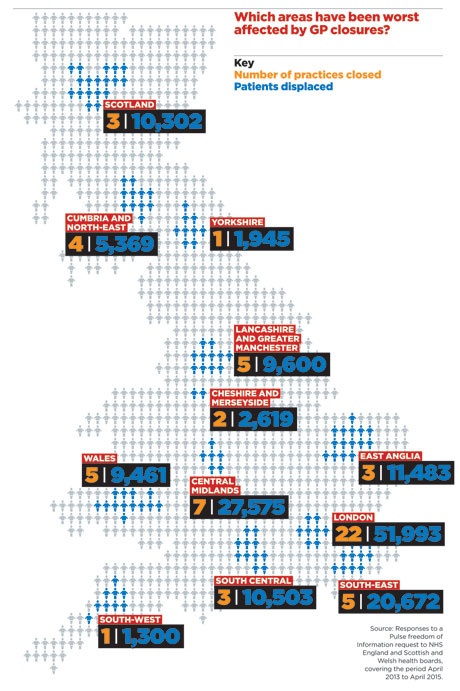
The closures are having a dramatic impact in some areas. In the Midlands, seven GP practices closed between April 2013 to April 2015, displacing 27,000 patients.
Birmingham LMC executive secretary Dr Robert Morley describes the situation as ‘absolutely dire and getting rapidly worse’.
He adds: ‘We have small partnerships that are becoming unviable because of issues of recruitment, retention, impossible workload, GP illness and singlehanders retiring, and practices are also being closed by the CQC, while commercial APMS contracts are being terminated.’
Since these closures were revealed, one of the largest practices so far affected shut its doors, citing chronic recruitment problems. The Hollywell Medical Group in Derbyshire, which had 27,000 patients, said it would be closing two branches, with the remaining three being taken over by the local foundation trust.
London has seen some 52,000 patients displaced after 22 closures – all but one of which involved GMS or PMS practices.
Dr Tony Grewal, medical secretary of Londonwide LMCs, says the closures put significant pressure onto neighbouring practices, which often have little choice but to take on the patients who have been left without a GP.
He says: ‘Most practices are working at full capacity [but] it is… policy for NHS England that smaller lists – usually less than 4,000 – will not be procured, but dispersed.
‘This means that surrounding practices may have to deal with several hundreds of new patients in a short space of time [and] it is recognised that the first year of registration with a new practice requires considerable extra work.’
Dr Grewal added that it was very hard for practices to close their list formally and that the GPC’s advice that practices could refuse new registrations while maintaining an open list ‘has not been completely accepted by NHS London’.
Emergency measures
Pulse recently revealed a 500% jump in the number of practices seeking advice from NHS managers about closure or merging. And some area teams are looking at emergency measures to support these practices, as called for in Pulse’s campaign.
The East of England NHS region is looking to pre-empt potential closures by creating an ‘index of vulnerability’ that proactively identifies struggling practices. But managers are still working on exactly what support can be offered to practices in difficulty.
Dr Guy Watkins, chief executive of Cambridgeshire LMC, says that the move is ‘clearly in our interests as GPs’.
He says: ‘Cambridgeshire LMC has been working with NHS England for some time to try to agree some support for practices to help review their options when practice stability is threatened, often for workload or financial reasons, before a crisis event, rather than afterwards.’
Last month, Pulse also revealed that the NHS England South region is preparing a scheme whereby neighbouring GP practices will be drafted in to provide emergency support to colleagues who are struggling to stay afloat.
In Wales, the Government has gone further, with the new GP contract making provison for a ‘sustainability programme’ to help out practices facing closure. The details are being hammered out, but the programme is likely to involve ‘assessment panels’ developing rescue plans.
The GPC insists that such programmes should be implemented on a nationwide basis – and for some areas the move cannot come too soon.
Only a few areas of the UK have avoided major closures, but local GP leaders are warning that it is only a matter of time before more practices succumb.
In the South-West of England, only one small practice has had to close, but Devon LMC medical secretary Dr Mark Sanford Wood says this won’t be the case for long.
He says: ‘We have worked hard in the South-West to rescue practices in difficulty, so the headline rate of failure is not a reflection of those that would have collapsed were it not for those efforts.
‘That said, we do understand that we have been relatively spared so far. The omens for the next 12 months are not good, though.’










