Revealed: ‘Shocking’ 25% of evening and weekend GP appointments empty

This month, the flagship Government policy of routine weekend and evening GP appointments is to be rolled out across England.
The Conservative Party pledged that every patient would be able to book a routine appointment any day or evening by October 2018.
The Government and NHS England have continued to pump money into this scheme, with specific pledges being made in the GP Forward View, and CCGs given earmarked funding.
In all, the NHS has committed more than £200m of new investment for the next year, on top of £144m in 2017/18. More than £500m is due to be invested per year by 2020/21.
Yet it has had little support from the profession. From the start, GP leaders have said the money would be better spent on routine care, that the policy would further stretch an already pressured workforce and that patients would be unlikely to use extended hours slots in high numbers.
And now a Pulse investigation can reveal that these warnings have been borne out.
A freedom of information request, answered by around 80 CCGs that have already rolled out the scheme, shows that 25% of evening and weekend appointments are left unfilled. From April 2017 to September 2018, this amounted to half a million empty slots across the 80 CCGs.
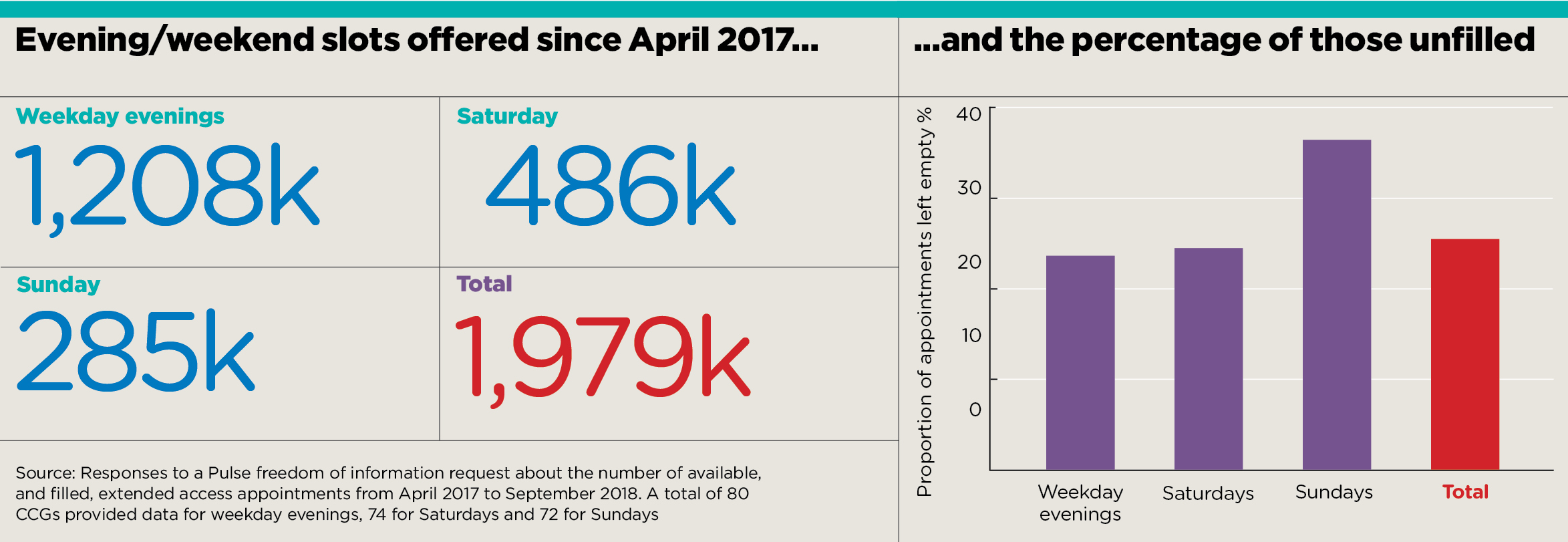
table and graph analysis
On Sundays – the least popular day with patients, according to the data – as few as 3% of appointments were being used in one CCG. Overall, 37% of Sunday appointments go unfilled. Yet local commissioners continue to increase the number of available slots.
This comes as the average wait for an in-hours appointment remains at two weeks, and one in six practices has had to stop booking routine appointments.
‘Ridiculous’ blanket approach to seven-day GP service
GP leaders branded the findings ‘shocking’, saying the ‘ridiculous’ blanket approach to extending access does not offer value for money while reiterating that funding should be used to provide services during routine hours, when most patients want to attend.
BMA GP Committee chair Dr Richard Vautrey says: ‘Because it has become a political must-do, everybody is jumping. We understand there is huge pressure from the centre on CCGs to demonstrate they are providing a full seven-day service.
‘Sensible CCGs that want to use their resources in a better way are under pressure to maintain a service that really isn’t good value for money.
‘That is ridiculous so I think we really do need to see much more common sense and pragmatic flexibility… if we had the luxury of resource and workforce then we could look at extending the service but until then we’ve got to focus on what is most important,’ he adds.
In addition, the goal of reducing patient demand on other services has not been achieved, says Dr Vautrey.
‘The time that people are waiting for an appointment during the daytime is getting worse and neither are we seeing any real impact on A&E waiting times, which was one of the justifications for extended access – that it was somehow going to reduce pressure on A&E.
‘All that has happened is it has widened access, rather than managing demand.’
NHS England maintains patients want access to a GP outside routine hours, suggesting they will choose a service based on speed of access.
In response to Pulse’s data, an NHS England spokesperson says: ‘Even though six out of 10 CCGs didn’t respond to this small survey, the more representative results of the annual GP survey and the patient response to new digital-first GP providers is clear: patients want quicker access to a trusted GP both during the working week and outside traditional surgery hours, and are increasingly prepared to vote with their feet to get it.’
Warning signs of unfilled appointments during pilot
Yet the 20 regions that piloted the scheme in 2014/15 offered a clear pointer as to levels of take-up. In those pilots, a quarter of all extended hours appointments were not filled as well.
However, NHS England policymakers dismissed concerns, claiming there had been a 15% reduction in minor A&E attendances. So they and the Government proceeded with the policy to enable any patient to access appointments until 8pm on weekdays, and to ensure Saturday and Sunday appointments were available across England by 1 October 2018.
CCGs are going ahead with rollout, although some say they have identified the least popular times and reviewed their service and at least 10 have reduced appointments.
Yet around six in 10 have increased the number of appointments on Saturday and Sunday over the course of the past year. Similarly, almost three-quarters of 58 CCGs that provided comparable data currently have, or plan to introduce in the next six months, more appointments on weekday evenings than they had around a year ago.
But a number of regions are unable to fill the majority of their appointment slots – particularly at the weekend.
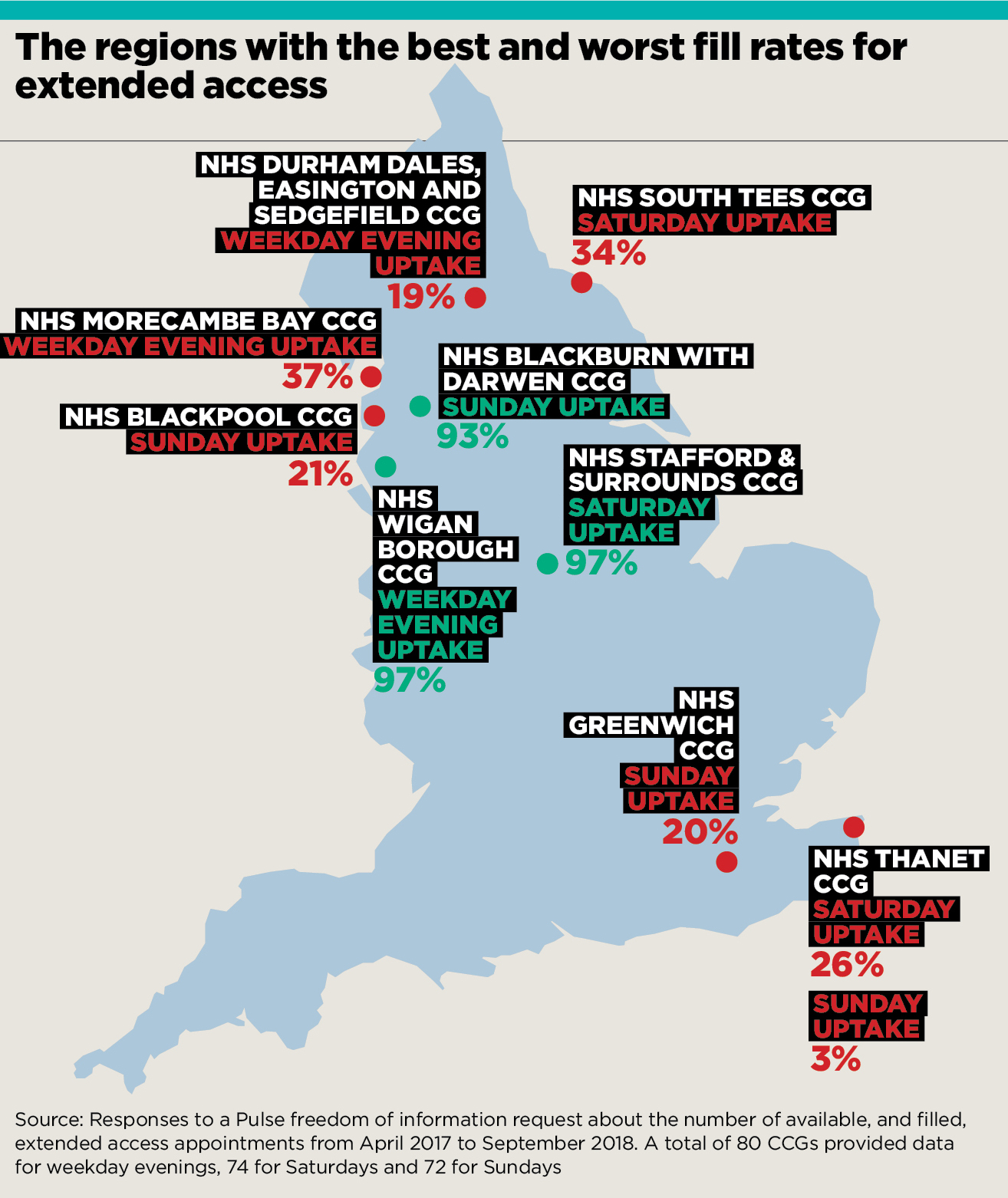
region map analysis
Pulse’s analysis of FOI responses from CCGs operating the scheme shows take-up remains lowest on Sundays, when 37% of appointments go unfilled, followed by Saturdays at 24%. On weekday evenings, 23% of slots go unused.
Waste of GP time when core services are struggling
NHS Thanet CCG, in Kent, has seen patients book just 3% of available appointments on Sundays and 26% on Saturdays since April 2018. Nevertheless, Thanet has opted to increase the number of appointments for the rest of this year.
Kent LMC vice-chair Dr Gaurav Gupta, who has worked some Saturday shifts in nearby Faversham, says this is explained by ‘political reasons, rather than what patients need’.
He adds: ‘I think patients would benefit more if these resources were spent to provide continuity of care in the week rather than on Sunday appointments patients don’t really want for routine care.
‘Also there’s the big issue of workforce… we are all struggling to provide core services anyway, so it doesn’t make sense to ask us to do more hours that aren’t used.’
A CCG spokesperson says the region has so far only been piloting the service and that appointment usage is expected to increase following a publicity campaign.
They add: ‘We are working with our team to ensure there is a publicity campaign across East Kent prior to the national 1 October go-live date. Our expectation is that uptake will improve once awareness increases and will build with time.
‘For Thanet, this represents about 200 additional GMS appointments per week. We have no reason to believe we’ll have an issue filling the available slots.’
Several other CCGs were only able to fill around a fifth of Sunday slots. This included NHS Blackpool CCG, with a 21% fill rate since September 2017. Local GP Dr Marie Williams says: ‘People didn’t seem to want Sunday access in this area.
‘Patients like to be seen at their own practice by someone they know and at a location nearby. Extended access schemes using existing practices just mean GPs are spread thinner during the working day, causing problems elsewhere.
‘Just adding appointments for primary care into a system doesn’t necessarily relieve the pressure on general practice, if it isn’t what your population wants or if they default to see their own GP for follow-up or referral onwards.’
CCGs blame lack of publicity for empty appointments
But Dr Amanda Doyle, chief clinical officer at NHS Blackpool CCG and former co-chair of NHS Clinical Commissioners, tells Pulse the service has generally been well received.
She says: ‘We have reviewed the service with patients in Blackpool and found Sundays are the least preferred time for people wanting appointments, although many have told us that they would use an appointment at any time if it meant a shorter wait to see a healthcare professional – which it does.
‘There are many reasons for low uptake, including lack of public awareness, reluctance to see a different doctor, appointment locations and difficulty for practices in booking these appointments. We continue to promote awareness of the service so patients understand what is available to them and its benefits.’
Nearby NHS Morecambe Bay CCG saw one of the lowest uptakes of appointments on weekday evenings, with 37% filled between October 2017 and June 2018 – but officials claim their popularity has increased over summer.
But RCGP chair Professor Helen Stokes-Lampard says it is ‘shocking’ that so many appointments are going unused.
‘GPs want to give patients access to services they need but this will differ depending on local demographics. At a time when general practice is struggling for resources and patients are waiting longer for routine appointments, to find out so many evening and weekend appointments have been unfilled due to lack of demand is shocking.’
Cost of unused appointments at least £15m
Pulse estimates at least £15m has been wasted on the total of 501,396 unused extended hours slots across the 80 CCGs that responded to the FOI. This is based on NHS England’s evaluation of the scheme’s pilot, in which the cost of each appointment was around £30-50.
In addition, last year some CCGs were told by NHS England to market seven-day access to patients if take-up is faltering.
Pulse can reveal 77 CCGs collectively spent £207,872 on marketing the scheme in 2017/18, according to data supplied under a separate FOI request. These campaigns to boost awareness of extended hours appointments appear to have produced mixed results.
The approach worked for NHS Bromley CCG, which spent £48,000 on a campaign and has managed to fill 96% of slots on weekday evenings and Saturdays and 79% on Sunday in 2017/18.
Yet there has been less success in NHS Southwark CCG, which spent £20,000 on a campaign to raise awareness in 2017 but only filled 50% of Sunday appointments between April 2017 and May 2018. However, weekday evenings and Saturdays did see higher take-up, at 82% and 73% respectively.
Southwark does not envisage further marketing, but it also does not plan to change its number of appointments, saying feedback has been ‘positive’.
GPC chair Dr Vautrey argues money should not be spent on marketing extended hours appointments.
‘Nobody is marketing their daytime GP services yet there is still a huge demand for them. We need to be investing the limited resources we have in the most effective way, and that is in core hours.’

page 15 infographic marketing spend
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens











