‘Daily aspirin can ward off cancer’ and ‘miracle pill cuts cancer deaths’ were the headlines dominating the national newspapers last month after UK researchers proclaimed people in late-middle age should consider taking adaily dose of the pill to prevent stomach and bowel cancer.
And the impact of the media reports was instant. Patients scrambled to self-prescribe as pharmacies reported big spikes in sales of the drug.
One pharmacy chain saw sales treble within a week.
But despite the hype, not everyone is persuaded by the evidence.
The research team insist they’re ‘convinced’ the overall mortality benefit-to-harm ratio is large enough to warrant a broad recommendation straight away. But after examining the data, other experts warn the actual benefits are so small that 200 patients would need to take the tablets for 20 years for even one of them to benefit.
The GPC argues that GPs don’t need to take a proactive role in recommending aspirin, with the RCGP saying doing so would only increase the profession’s already onerous workload.
But with the researchers and Cancer Research UK recommending patients see their GP rather than self-prescribe, it seems that GPs need to be prepared for a flurry of patients seeking their advice.
Out of favour
The humble aspirin has long been touted for its life-saving properties, largely because its antithrombotic effects significantly reduce the risk of recurrent vascular events in people who have had heart attacks or strokes.
But its use in the primary prevention of cardiovascular disease has gradually fallen out of favour, with mounting evidence showing its benefits in reducing the risk of heart disease are offset by increased risks of serious bleeding events, including haemorrhagic stroke.1
Even in patients with diabetes – for whom NICE guidance still recommends aspirin – studies are questioning its use.
However, evidence has steadily been accumulating since 2009 that aspirin may have more potent effects in reducing the risk of cancer – in particular cancers affecting the gastrointestinal tract.
Most recently, a large meta-analysis concluded aspirin significantly reduces the risk of cancer death if taken for at least five years.3
Now a team of researchers say these anti-cancer benefits mean that overall the benefits of taking a low dose of aspirin every day far outweigh any harms.4 Lead researcher Professor Jack Cuzick, professor of epidemiology and head of the Centre for Cancer Prevention at Queen Mary University of London, argues more research is needed to determine the optimal dose and duration, but tells Pulse: ‘We’re convinced the overall risk-to-benefit ratio is sufficiently positive that we don’t need to wait for [further] research, but can start with what we know now; that is, low-dose aspirin for people aged 50-65 who don’t have the standard risk factors for bleeding.’
Crucially, the experts’ pronouncement is not based on new trial evidence or a formal systematic review and meta-analysis. The researchers have simply re-appraised available evidence from published systematic reviews of randomised controlled trials and epidemiological studies – although they say they have carried out a more comprehensive analysis of the net benefits against harms than has ever previously been attempted.
‘GPs are the ones who can really help to identify people who are at increased risk of bleeding – people with hypertension, on warfarin, and those kinds of things.’
Professor Cuzick
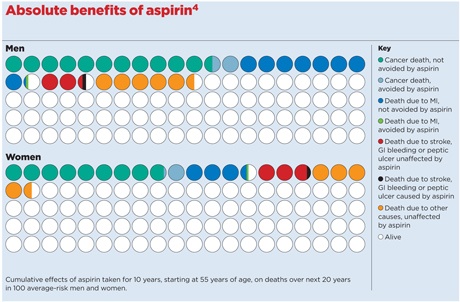
From these data, they conclude a daily aspirin (between 75mg to 100mg) taken for at least five years and up to 10 years will reduce the risk of dying from colorectal cancer over 20 years by 40%, and from stomach or oesophageal cancer by 35-50%. On the other hand, it will increase the risk of a fatal stroke by 21% and the chance of developing, or dying from, a serious gastrointestinal bleed or peptic ulcer by 60%.
Despite these downsides, they calculate that, for people aged 50-65 years, the mortality benefits of routine aspirin treatment outweigh the harms by eight to one, although from the age of 70 the risk of bleeding increases considerably.
But Professor Tom Marshall, professor of primary care and public health at the University of Birmingham, points out the calculations show a high number of people would need to be treated for one person to benefit.
Professor Marshall says: ‘Even if we believe the claims… the benefits are very small, perhaps 200 patients taking tablets for 20 years for even one to benefit.’
In addition, Cancer Research UK – listed as one of the sponsors of the review – is quick to distance itself from the researchers’ unequivocal conclusions, arguing that ‘some important questions’ need to be answered over dosage, who may suffer side-effects and for how long people should take aspirin.
‘Given the continued uncertainty over who should take aspirin, Cancer Research UK is funding a number of trials and research projects to make the picture clearer,’ says Dr Julie Sharp, the charity’s head of health information.
What should GPs do?
The researchers and Cancer Research UK are united in urging patients to avoid self-prescribing and visit their GP for advice instead.
However, GP leaders are warning that offering such advice will be easier said than done, particularly in the absence of new guidance or a change in policy that GPs can rely on.
The Department of Health says it is in the process of developing guidance, in collaboration with Cancer Research UK, and that the current study forms part of that programme of work. But it says there is no new advice for GPs yet.
‘It is for doctors to make prescribing decisions based on the needs of their patients,’ a DH spokesperson says.
Professor Cuzick argues that GPs have a ‘major role’ to play in implementing his recommendations.
Numbers needed to treat with aspirin4
33-127 to prevent one major cancer or CVD event
46-213 to prevent one CVD or cancer death
He says: ‘GPs are the ones who can really help to identify people who are at increased risk of bleeding – people with hypertension, on warfarin, and those kinds of things. That kind of trade-off has to be made every day by a GP. This is a good bet in that the benefits outweigh the risks by eight to one in terms of mortality – but some people are going to be harmed, we know that. GPs need to be clear that there are side-effects.’
But the RCGP points out asking GPs to give out advice on aspirin does not take into account the reality of practices’ daily priorities. ‘It is difficult to see how we will be able to find enough time to do this when the profession is already struggling to cope with the soaring numbers of patients who are presenting with multiple and increasingly complex needs,’ the college says.
Estimated impact on mortality if total UK population aged 50-64 years took aspirin for 10 years.
The GPC offers a more robust line, saying the experts’ review does not shift the balance in favour of recommending aspirin and there is no need for GPs to take a proactive role.
Dr Andrew Green, chair of the GPC clinical and prescribing subcommittee says: ‘I would be encouraging people to have a chat with their pharmacist about it rather than their GP. We don’t have enough evidence to recommend it for everybody. If a patient wants to disregard that they should still get some advice – but the pharmacist can advise them if there is anything in their medical history or their current prescriptions that means they shouldn’t take aspirin.’
Professor Willie Hamilton, GP and professor of primary care diagnostics at the University of Exeter, agrees the latest review provides little additional information and is not enough to support a population-wide approach.
‘There’s not much difference between the findings – just the interpretation is more positive,’ he says. ‘What these studies don’t take into account is the practicalities. We’ve seen the fuss over NICE’s statin guidance, and although the apparent battle lines in that argument were around quantifying the number of patients who experience side-effects, another part of the reluctance by the GP community was the fact of changing a person into a patient. I know taking 75mg of aspirin should be as easy as brushing my teeth every night – but it’s not’.
But it seems that patients are taking it into their own hands, with pharmacies reporting hikes in aspirin sales following the study’s publication. Superdrug told Pulse it had seen a 229% increase in the amount of low-dose aspirin sold nationally the week after the study was published. Despite GP reservations, aspirin is making a comeback.
References
1. Seshasai SR et al. Effect of aspirin on vascular and nonvascular outcomes. Meta-analysis of randomised controlled trials. Arch Intern Med 2012;172:209–216
2. Ekström N et al. Aspirin treatment and risk of first incident cardiovascular diseases in patients with type 2 diabetes: an observational study from the Swedish National Diabetes Register. BMJ Open 2013; 3: e002688
3. Rothwell PM et al. Short-term effects of daily aspirin on cancer incidence, mortality and non-vascular death: analysis of the time course of risks and benefits in 51 randomised controlled trials. Lancet 2012;379:1602-1612
4. Cuzick J et al. Estimates of benefits and harms of prophylactic use of aspirin in the general population. Ann Oncol 2014; available online 6 August
5. NHS Choices 2014. Daily aspirin ‘reduces cancer risk’, study finds.
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.