How GPs are defying the push to widen statin use


As the debate over the merits of statins for primary prevention rumbles on, it seems GPs are digging their heels in and resisting the drive to put millions more patients on the drugs.
A Pulse analysis of NHS prescribing data reveals that overall GP prescribing of statins in England has changed little since the introduction of NICE guidelines that could effectively double the number who take the drugs for primary prevention of cardiovascular disease.
These data even suggest the rise in overall statin use seen over recent years is levelling off, with only a 2% increase in statin use this year, compared with 3% the previous year. The number of statins prescribed per 1,000 patients on GP lists has risen by a barely perceptible 0.9%.
GP experts from both sides of the debate say this reflects doubts over the new recommendations and also that many GPs are simply ‘too busy to worry about it’.
And it comes as NICE is very much on the back foot over its recommendations on lipid modification, after GP leaders recently fought off plans that would have seen GPs incentivised through the QOF to prescribe more statins.
But GP proponents of statins say they are disappointed more is not being done to promote uptake, particularly in younger people with cardiovascular risk factors, which they claim is an essential part of the Government’s drive on prevention.
Overburdened
Introduced in July 2014, NICE’s updated guidelines on lipid modification advocated halving the risk level at which outwardly healthy people should be considered for statin therapy – from a 10-year predicted risk of 20% to 10%.
At the time, NICE estimated this would make around five million more people eligible to start taking a statin – with the potential to ‘save 8,000 lives over three years’ and prevent ‘up to 28,000 heart attacks and 16,000 strokes each year’.
However, the move was roundly condemned by GP leaders, with both the GPC and RCGP questioning the evidence behind it and warning it would not only risk overmedicalising vast swathes of the population, but also swamp already overburdened practices with extra appointments, diverting precious time away from patients in more immediate need.
A survey by Pulse last October revealed that two-thirds of GPs were completely disregarding the guidelines and refusing to offer statins to newly eligible patients at the 10% risk level.
Now, data from the Health and Social Care Information Centre – aggregated by the market research division of Cogora, the publisher of Pulse – show the number of statin prescription items written in general practice in England – and dispensed to patients – in the first half of 2015 was only 2% higher than in the same period of 2014, before NICE pushed through the new guidance. This compares with increases of 4% and 3% over the two preceding years. When population growth is factored in, the number of prescriptions for statins has barely risen, with 569 per 1,000 patients in 2015 taking statins compared with 564 in 2014.
Dr Martin Duerden, prescribing adviser to the RCGP and a member of the NICE panel that drew up the 2014 guidelines, says the figures show GPs are too busy to implement them.
He says: ‘The relative lack of overall growth is related to getting to grips with the new guidance and also a fair amount of resistance to changing practice in this way. Workload also has a lot to do with it, as many GPs are already running to stand still and don’t see this as a priority.’
Dr Duerden adds another reason for the slow uptake may be patient choice: ‘Lower-risk people might be keener to explore lifestyle change rather than embark on a lifetime of pills. Negative media coverage of statins doesn’t help.’
Simvastatin switch

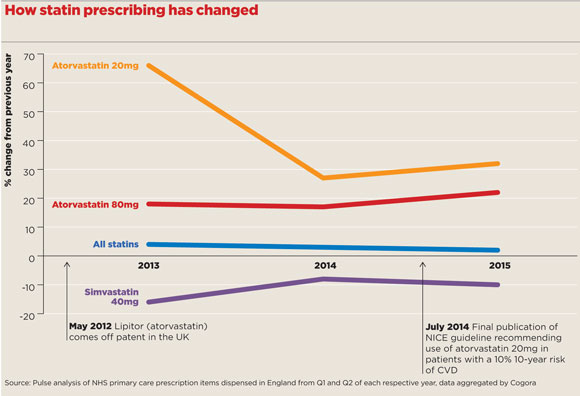
For atorvastatin 20mg – specifically recommended for primary prevention – there has been a rise of 32% in prescribing this year above 2014 figures, compared with a 27% increase in prescriptions between 2013 and 2014. However, much of this can be explained by a 10% reduction in simvastatin 40mg prescriptions, which remains by far the most widely issued statin, with more than 30% of all prescriptions.
There was a massive 66% rise in atorvastatin prescribing in 2012, which coincided with its coming off patent, as GPs in many areas began systematically switching patients from simvastatin under local cost-saving schemes designed to take advantage of atorvastatin’s plummeting price. This was reinforced when evidence emerged of an interaction between simvastatin and the calcium channel blocker amlodipine.
Meanwhile, prescriptions of atorvastatin 80mg have grown by 22% in the past year – more than in previous years when they grew by 17%-18% – but also in line with a switch from simvastatin as first choice for secondary prevention.
Dr John Ashcroft, a GPSI in cardiology in Derbyshire who supports lowering the risk threshold, says these data show ‘the biggest change is the increase in atorvastatin 20mg with commensurate reduction of simvastatin… presumably in part the result of NICE guidance’.
However, he adds: ‘Overall there has been a small growth in the prescribing of statins, but it looks less than in earlier years and less than one would have hoped.’
NICE chiefs have maintained they never intended that millions more people be put on statins, but wanted to offer the option for those who had already considered lifestyle options to reduce risk.
But the institute came under fire after it moved to pressurise GPs into adopting the 10% threshold through the QOF, recommending an indicator rewarding practices by their rate of statin prescribing in anyone newly diagnosed with hypertension or diabetes who has a 10% or higher 10-year cardiovascular risk.
Public Health England announced last year that it wanted the NHS Health Checks programme – the five-yearly ‘health MOT’ offered to everyone aged 40 to 74 – to adopt the 10% risk threshold. However, evidence indicates that, with the exception of some areas that have put in extra resources, the health checks scheme as a whole is still struggling with poor uptake as well as treatment and follow-up of patients identified as at risk.
Lack of progress
A NICE spokesperson tells Pulse that the evidence supports its approach: ‘The independent committee of experts found that if a well patient and their doctor measure the risk and decide statins are the right choice, the weight of evidence clearly shows no credible argument against their safety and clinical effectiveness in people with a 10% risk over 10 years.’
However, some GP experts in cardiovascular disease have expressed concern at the lack of progress in preventing CVD since the NICE guideline.
Dr Matthew Fay, a GPSI in cardiology in Shipley, West Yorkshire, says these data are ‘very depressing’ and reflect ‘a failure of our clinical leaders to engage the media and hence the population in a reasoned debate’.
He adds: ‘The prevention agenda has to be one of the most important facets of the strategy for the future. This failure to implement the NICE guideline has to be laid at [GP leaders’] door, I fear, allowing the few naysayers to be seen as the opinion of the profession.’
But Dr Kathryn Griffith, a GPSI in cardiology in York and a leading member of CVGP, the ‘society for professionals with an interest in cardiovascular disease in general practice’, believes there has been more statin prescribing ‘in areas where the [NHS] health checks are going well’, but that for ‘the average GP, the enthusiasts will be prescribing and the others will be too busy to worry about it’.
Dr Martin Brunet, GP trainer in Guildford, Surrey, and a leading member of the RCGP’s overdiagnosis and overtreatment group, says ‘neither the public nor GPs are convinced of the value in using the 10% on an individual level’.
He explains: ‘It might make sense on a macro public health level, but the argument is very different for someone who has a 10% risk just by virtue of age.’
And so far, despite the best efforts of NICE, it looks like the ‘naysayers’ are winning the argument.
Statins ‘postpone death by three or four days’
Treatment with statins only improves people’s overall survival very slightly, postponing death by around three or four days, a new analysis of trial evidence has found.
The authors of the analysis said GPs should not push the use of statins in people worried about their side-effects or in those with limited life expectancy.
The Danish researchers looked at 11 randomised controlled trials of statins that reported all-cause survival curves, with follow-up lasting between two and six years.
They found statins postponed death by a median of 3.2 days in the six studies where they were being tested for primary prevention, and a median of 4.1 days in five studies of their use for secondary prevention.
The researchers wrote: ‘Statin treatment results in a surprisingly small average gain in overall survival within the trials’ running time.’
They said that as a result, when treating people with statin intolerance or in whom treatment is associated with unpleasant side-effects, GPs ‘should not be too insistent on the patient continuing them’.
Meanwhile, ‘for patients whose life expectancy is short, the benefit of statin therapy in terms of survival gain may be quite limited’, they wrote.
The team added that explaining how long statin treatment is likely to delay death, rather than using terms like ‘numbers needed to treat’, may help people to weigh up the benefits and risks of treatment more easily.
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.











