CQC admits errors and (almost) pulls its risk ratings
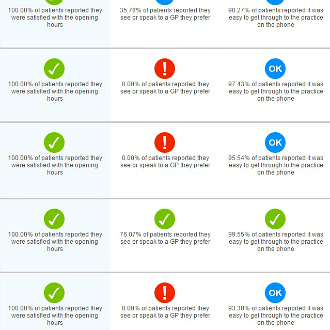

GP practices will no longer be given risk ratings by the CQC, after the regulator promised to end publication of its ‘intelligent monitoring’ bandings, which had caused huge distress for hundreds of practices.
A mere four months after the bandings were introduced, the regulator has bowed to overwhelming pressure from the profession and said it will only give an overall rating to GP practices after an inspection.
And it went even further, by apologising to practices, admitting its language about the ‘risk’ posed by the practices given the worst ratings ‘wasn’t right’.
However, some are still using the ratings. A website run by the Department of Health to allow patients to compare GP practices was continuing to publish the ratings four weeks after the CQC’s apology. And for some GPs the U-turn is a pyrrhic victory.
The damage was done late last year when their practices were splashed across the front of local newspapers, denounced as a risk to patient safety.
In an email to GPs, sent on 26 March, the CQC said it had ‘listened to the concerns of the GP profession’ and, as a result, would no longer give practices a banding between one and six to signify their potential level of risk.
It will also change the language it uses so as not to ‘imply a risk to patient safety’, although it will continue to publish its so-called intelligent monitoring reports without ratings.
The regulator said it would work with the GPC and the RCGP to develop a ‘better way of reviewing practice data’, and it is also in the process of reassessing the indicators it uses to prioritise practices for inspection.
The controversy started in November last year, when, almost out of the blue, the CQC published the intelligent monitoring data on its website, giving practices a banding of one (potentially risky) to six (no risk) based on QOF scores and patient survey data. Practices given ratings of one or two found themselves featured in local media, while national media ran headlines declaring ‘one practice in six’ was a risk to patient safety.
Growing pressure
The GPC said there had been minimal consultation with the profession and, almost immediately, errors in the data were found by Pulse, the BMA, the RCGP and individual practices themselves. The message to the CQC from all parties was clear: the bandings should be withdrawn.
Department of Health’s My NHS website
The regulator refused to go this far at first. It admitted there were errors, but stuck to the line that the bandings were not meant to rate practices, and were simply supposed to indicate which practices should be prioritised for inspection.
But the pressure grew, with the GPC and RCGP continuing public attacks on the process. Following this lobbying from the profession, the CQC has now apologised in full for publishing the data and agreed to stop banding practices based on intelligent monitoring.
The CQC’s email to practices stated: ‘What we published wasn’t right regarding the use of language around risk, and on the analysis of variation between practices. We apologise.’
But as usual, it was not quite so simple. My NHS – the Trip Adviser-style website run by the DH – was still publishing the ratings several weeks later.
Dr Robert Morley, chair of the GPC’s contracts and regulations subcommittee, called on the DH to remove the information immediately.
He said: ‘It is outrageous that the discredited and discontinued banding ratings are still being publicised on a DH website.’
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens











