The true cost of a CQC inspection


GP practices look set to pick up the tab for the radical expansion of the CQC’s inspection regime.
Under chief inspector Professor Steve Field, the CQC intends to inspect every GP practice in England by April 2016.
Pulse has learned this is costing £13.3m a year, and the intention is for practices to foot the entire bill.
The Treasury is insisting that all central funding for regulation is phased out under a timescale to be negotiated by the regulator and the Government. This means the average GP practice faces the prospect of paying hundreds of pounds more per year for the honour of being inspected.
The regulator has already increased fees way above inflation since the new inspection regime was introduced, with a 12% hike in 2013, 2.5% in 2014 and a further 9% this year.
Currently, GP practices with a single site pay between £616 and £948 per year, while fees for those with multiple locations range from £1,341 to £16,759. But these fees could more than double over the next few years.
And these figures do not include the sizeable costs borne by practices preparing to be inspected, with one GP estimating preparation for the CQC’s arrival cost his practice nearly half a million pounds.
A Pulse survey reveals that almost half of GPs said their practice spent more than 20 staff hours preparing for an inspection, with many spending hundreds of hours, and had to cancel an average of 15 appointments on the day of the inspection.
All this comes at a time when GPs are increasingly questioning the need for the CQC in primary care.
The GPC and the RCGP have publicly called for the CQC’s activities to be scaled back and the LMCs Conference went even further, voting to press for the abolition of the regulator, a call subsequently backed by the wider BMA Annual Representatives Meeting last month.
The RCGP passed an emergency council motion calling for an immediate suspension of inspections to allow practices to deal with their current huge workloads. This provoked an angry response from Professor Field – a former RCGP chair – who said he was ‘extremely disappointed’ with the college.
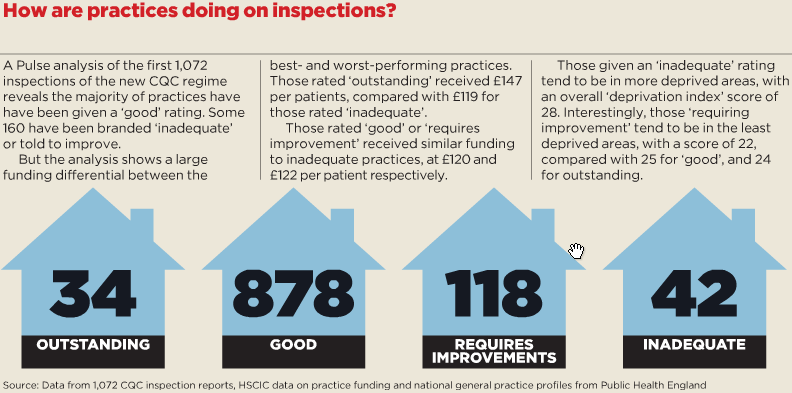
Despite this wrangling, a Pulse analysis shows GP practices are performing remarkably well under the inspection regime. Only 3.9% (42) have been branded ‘inadequate’, against 11% of acute trusts, and most are rated as ‘good’.
Nevertheless, the amount of funding received per patient and levels of deprivation seem to be linked with a practice’s CQC rating, particularly at the top and bottom ends of the scale, leaving some practices feeling they are doomed before inspection.
Regardless of GPs’ concerns over its regime, the CQC is publishing its consultation on the new fees structures this month – and it is unlikely to make happy reading for practices.
The true cost of a CQC inspection
Totalcost of GP inspection regime in 2014/15
£13.3m
Contribution from GP fees to CQC in 2013/14
£6m
GP practice fees (single location) in 2015/16
£616-£948
GP practice fees (multi-location) in 2015/16
£1,3410-£16,759
How long did you practice spend preparing for the inspection?
0-12 staff hours 11%
12-15 staff hours 5%
15-20 staff hours 36%
More than 20 48%
How many appointments did your practice have to cut on the day of the inspection?
No appointments 28%
0-10 appointments 14%
11-20 appointments 23%
21-30 appointments 19%
31-40 appointments 10%
41-50 appointments 4%
More than 50 appointments 2%
The survey launched on 9 June 2015, collating responses using the Survey Monkey tool. The survey was advertised to Pulse readers via our website and email newsletter, with a prize draw for a Samsung HD TV as an incentive to complete the survey. Some 206 GPs answered these questions.
Untenable costs
A Department of Health spokesperson tells Pulse the CQC will continue to receive Government funding for work such as annual reports and accounts, thematic reviews and costs for enforcement actions. However, the spokesperson says the regulator ‘is moving to full cost recovery for registration and inspection functions’.
How quickly the CQC ramps up its fees will be down to the regulator itself, and the CQC admits that they are likely to increase incrementally.
When Pulse put it to the CQC that fees paid by GPs could double, a spokesperson responded: ‘It would be reasonable to assume that fees for all providers are likely to increase over time to meet our obligations for cost recovery.
‘We will be setting out the indicative levels for all providers later this year as part of a full consultation.’
Dr Robert Morley, executive secretary of Birmingham LMC, says he expects fees ‘at least’ to double in coming years.
He says: ‘Fees account for about 50% of the cost of inspecting primary care services as it is. The big question is whether the scope of inspections will increase as well. There may be additional costs – the CQC can keep increasing fees, there’s no one to regulate the regulator.’
Dr Morley also points out that fees are not the only issue: ‘We are talking about significant amounts of money and time spent on a process that has not been proven. For smaller practices, the process is proving virtually untenable and we need this to be acted upon.’
One practice, the Over Wyre Medical Centre in Lancashire, estimated that preparing for inspection, including staff costs, cost £430,000. The practice was only able to shoulder these costs thanks to the goodwill of staff, who worked weekends without overtime and carried out mandatory training in their own time.
Pointless courses
A GP in Essex told Pulse that his practice had paid upwards of £8,000 in fees and preparation to get ready for a recent inspection, while a GP from Woking says his practice spent close to £10,000 to change floors and carpets across three different sites to prepare for inspection.
Dr Chantal Simon, a GP in Oxford, says: ‘Preparation runs into thousands of pounds in practice manager and administrative staff time, not to mention the hours of GP time doing pointless courses to tick boxes – and that is even before we have been inspected.’
Some practices have even gone as far as to take on permanent employees specifically to maintain CQC-related data.
This has a direct effect on patients too – more than 65% of the GPs Pulse surveyed said their practice had been forced to cut more than 10 appointments on the day of their inspection.
The CQC argues inspections should not be a burden to a ‘well-managed practice’ but with costs to practices set to increase further, concerns about the value of the CQC are likely to get louder over the coming months.
CQC fees analysis – July
Additional reporting by Allie Anderson and Sally Nash.













