The online providers disrupting the market

In 2016, the Dr Jefferies and Partners practice in west London was an unremarkable practice. It had a patient list size of around 16,000, nine GPs and a CQC rating of ‘good’.
It has now become the symbol of a fundamental shift in general practice. Its patient list exceeds 44,000, it has forced its CCG to borrow money from neighbours just to afford its global sum and NHS England has proposed changes to the GMS contract in response to its business model.
The reason for this sea-change? The practice hosts the new GP at Hand online service in partnership with private provider Babylon. It offers patients across London the chance to ‘see an NHS GP for free 24/7’ and a video consultation usually within two hours. It also promises in-person appointments ‘the same or next day’ from Monday to Saturday. It is using rules that allow practices to register patients from outside their area, with no obligation to provide home visits.
And patients have been flocking to it. For many – including, importantly, the new health secretary – it seems like a great use of innovation, and the direction general practice should be moving in.
The emergence of Babylon is part of a wider trend. There are now 37 private providers registered with the CQC to provide online consultations in England. In Wales, regulators have received five enquiries in the past year from online GP providers wanting to register, and Scotland is currently registering its first online primary care providers.
Some of these are now looking to access the NHS funding on offer by partnering with NHS practices to give younger, fitter patients services they can’t get from their bricks-and-mortar practices.
Others are using apps to make private consultations more convenient for patients and attracting NHS GPs to work for them. They are using major advertising campaigns and comparing themselves with consumer brands. It seems genuine market competition could now exist in general practice.
But, for many, this is a worrying development. Although some patients might enjoy the benefits of a speedy service, GP leaders say this is a threat to traditional practices and has the potential to harm vulnerable patients.
Two-tier general practice
East London GP and deputy chair of Doctors in Unite Dr Jackie Applebee has been leading the protests against GP at Hand. She says the trend towards online services has serious ramifications for general practice. ‘There will be an increase in patients moving around… there is cherry-picking of younger, fitter patients – on whom we rely. Some practices could go under, because they are losing these patients.
‘This could mean two-tier general practice. General practice for the internet-savvy – and general practice for those who are less able to use the apps, or who are sicker and need a different level of care.’
As RCGP chair Professor Helen Stokes-Lampard put it, GP at Hand is ‘disruptive innovation at its most disruptive’.
Most of these online providers started by offering their apps at a cost to patients, either charging a fee for video consultations or providing convenient appointments booked through an app, with patients retaining their registration with their usual practice.
But over the past year, many have been targeting partnerships with NHS practices. Push Doctor – a private service that currently offers video consultations with GPs ‘in minutes’ for £20 each – is in talks with Birmingham-based superpractice Modality about offering its service to patients for free in order to attract NHS patients.
Online triage and consultation tool eConsult is being rolled out across numerous practices after it was trialled in the capital. The Hurley Group, which developed the tool, has said its own NHS superpractice in London plans to see patients face to face only when necessary in the future.
And Now Healthcare Group is offering its app-based video consultation technology to practices for free, in a bid to reach more patients to whom it can advertise its repeat prescription delivery service.
Meanwhile, Babylon is looking to expand. Medical director Dr Mobasher Butt tells Pulse ‘tens of practices’ are interested in partnering to offer GP at Hand. Importantly, it seems this model of general practice has the backing of NHS England, which has set out requirements to ensure safety.
But suspicions have been raised about whether GP at Hand has had behind-the-scenes support, after NHS England chair Professor Sir Malcolm Grant said the service was an experiment ‘we have been conducting in London’. NHS England has denied this, saying it has only been involved in commissioning and assessing the service.
Support for technology from new health secretary
In any case, GP at Hand has another influential cheerleader. New health secretary Matt Hancock – previously the digital, culture, media and sport secretary – is signed up and has reportedly claimed it to be ‘brilliant’.
Such developments are concerning, says Dr David Mummery, joint-chair of Hammersmith and Fulham LMC, where Dr Jefferies and Partners is based.
He says: ‘There wasn’t much of a warning. GP at Hand was a bit of a bolt from the blue.
‘It was full-on and quite aggressive advertising. Posters when you got off the tube at West Brompton, things on the underground. It was clever marketing.
‘It created a lot of anxiety for GPs as to whether all their healthy patients would be attracted to GP at Hand.’
The Drum, a website for the advertising and marketing industries, said Babylon’s media agency PHD Media looked at which of the capital’s boroughs outside west London would be best to target 20- to 39-year-olds – it chose Hackney and Southwark.
Crucially, GP at Hand advises certain patients to ‘discuss’ whether it may be ‘appropriate’ to register with ‘a practice closer to home’. These include pregnant women and patients with learning difficulties, drug dependency, complex mental health conditions, frailty or dementia. It says this advice followed discussions with NHS England.
Practices in London are already feeling the effects of this disruption. One said it was losing an average of 10 patients a week to GP at Hand and that the practice’s growth had slowed considerably in the past year (see further below).
Just as importantly, the flock of patients registering with the service is playing havoc with CCG funding (see graphic directlybelow).
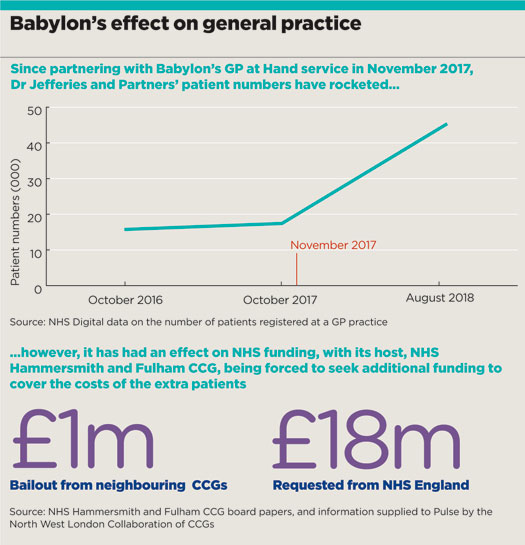
babylon effect on general practice
Increasing numbers of staff working for private providers
On top of this, the online providers are luring GPs to work for them at a time when most practices are struggling to recruit. NHS practices are finding it hard to compete with private providers that offer incentives, flexible working and even the option to work from home.
Babylon says it has more than 200 GPs on its books. Push Doctor launched in 2015 with 7,000 GPs providing private consultations, Doctaly works with 70 NHS GPs and nine private GPs – up from 40 GPs at the end of 2017 – across 49 practices in eight areas of England and two in Scotland. Now Healthcare Group’s Now GP app has ‘access to hundreds of NHS GPs’ across the UK for its paid consultations.
Dr Applebee underlines that this activity is far from helpful in a recruitment crisis: ‘There’s no two ways about it – if GPs are not working in traditional general practice and are working for an online provider, that is creaming off staff.’
Babylon is bullish about its offering, saying competition already exists and there is nothing to stop other practices offering online services.
Dr Butt says: ‘It’s an even playing field. Any practice is able to think of innovative ways to provide care and there’s nothing about the launch of GP at Hand that precludes anyone else from forming similar innovative solutions.’
But BMA Council deputy chair Dr David Wrigley disagrees: ‘Most practices struggle to offer basic GMS care at the moment due to gross underfunding and lack of staff, so it is unfair that companies who seek funding from city financiers set up services to compete with surgeries. That’s not a level playing field.’
Babylon hasn’t had it all its own way though. NHS Birmingham and Solihull CCG has objected to it expanding to the second city, while the changes proposed to the GP contract by NHS England to distribute funding more fairly between ‘digital first’ practices and the rest could see a slight reduction in funding for Dr Jefferies and the like.
However, in England, regardless of any stumbling blocks facing online providers at the moment, the long-term direction of travel is clearly towards ‘digital-first’ practices, where patients access their GP online before face to face.
As NHS England itself says in its consultation document on the contract reforms: ‘We know that by the end of the next decade digital technology is likely to have transformed general practice.’
For Hammersmith and Fulham GP Dr Mummery, ‘it’s pretty likely’ others will follow the GP at Hand model: ‘Most people think this horse has bolted. It’s a game changer.’
‘We’re losing young, healthy patients’

dr gary marlowe
Dr Gary Marlowe
The De Beauvoir Surgery in east London was previously seeing 1,500 patients join its list each year – but in the past 12 months just 200 have registered, according to its principle GP Dr Gary Marlowe.
He said the practice list mainly comprises younger patients, who attract less funding. But the healthier ones are signing up with GP at Hand.
Dr Marlowe said: ‘We are already quite affected financially because the majority of our patients are between the ages of 20 and 40. They are often in highly stressed jobs in the City and can take up a huge amount of time and appointments for mental health issues and work-related stress.
‘But because of their age and their conditions, they don’t carry a QOF code, which means our prevalence for heart failure, COPD and so on is really low, which affects our income.
‘The patients we are losing are our really young, healthy patients who maybe contact us once a year… that allow us to see the other patients who are coming in to consult once a week.’









