Medical arithmetic: losing cuticles, puffy eyelids, blistered lips
What do these presentations add up to? By Dr Keith Hopcroft
CASE EASY
The patient
This 43-year-old man works as a dishwasher in a restaurant.
He says
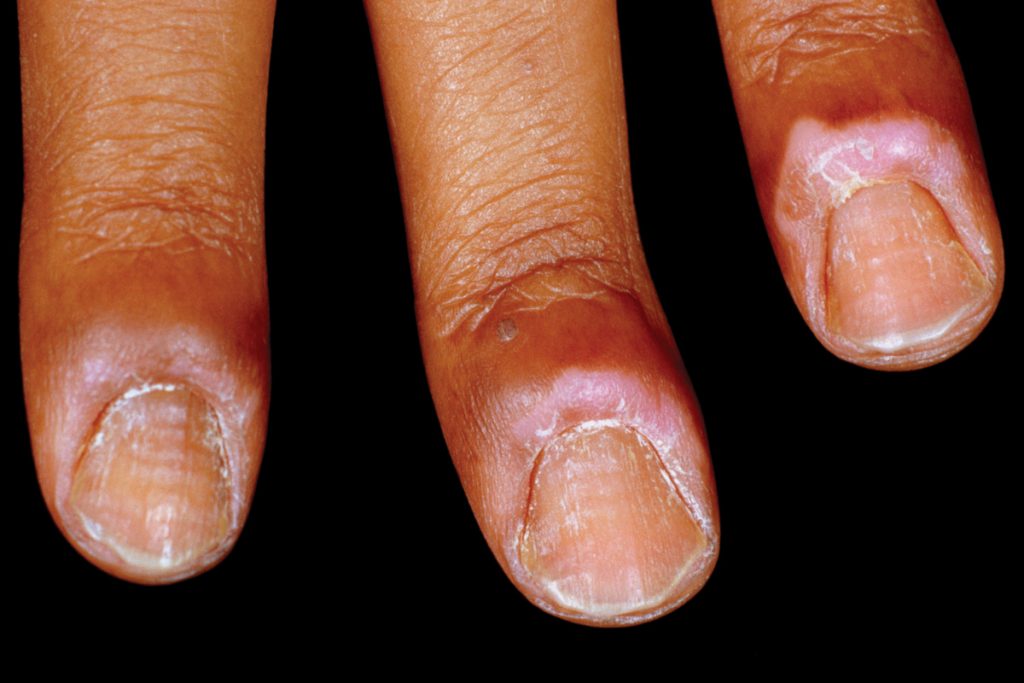
‘My nails are weird. It looks like I’m losing the cuticles. I thought it would go away but it’s persisted for months now, and all the fingers are affected. At work, they won’t let me back in the kitchen until it’s sorted out.’
+
=
See end of article for answer
CASE MODERATE
The patient
This 68-year-old woman has no significant past medical history, and is on no medication.
She says
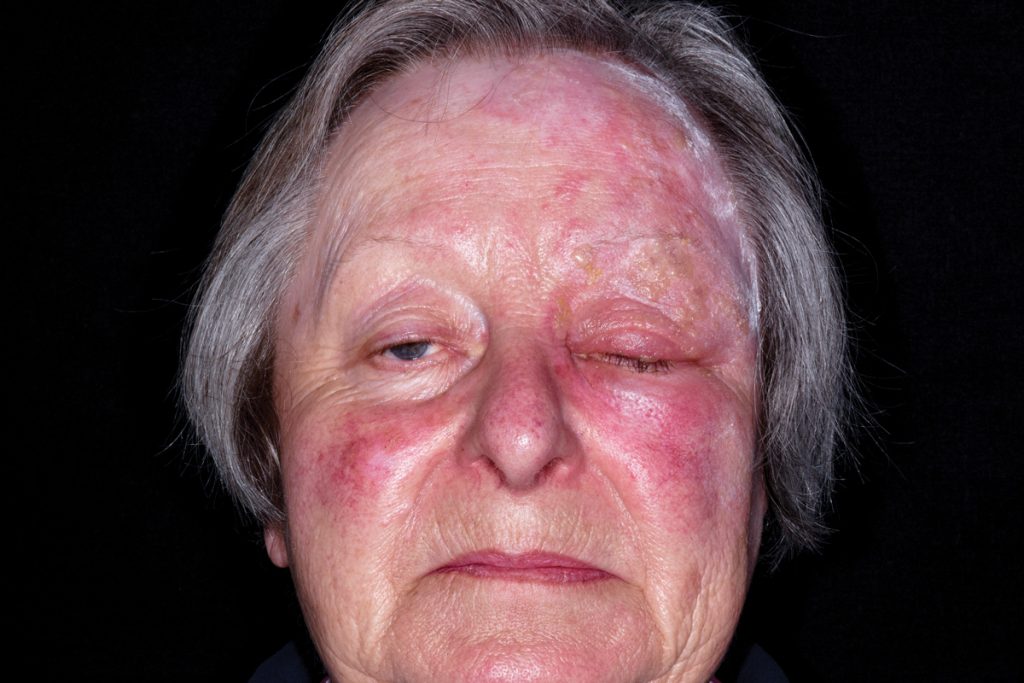
‘I’ve felt tingling and some numbness on the left side of my face for a few days. Now it’s gone red and lumps are appearing, which are getting worse. My eyelid’s gone puffy and I feel a bit like I might have flu.’
+
=
See end of article for answer
CASE HARD
The patient
This 19 year old girl was brought in by her mother.
Mum says
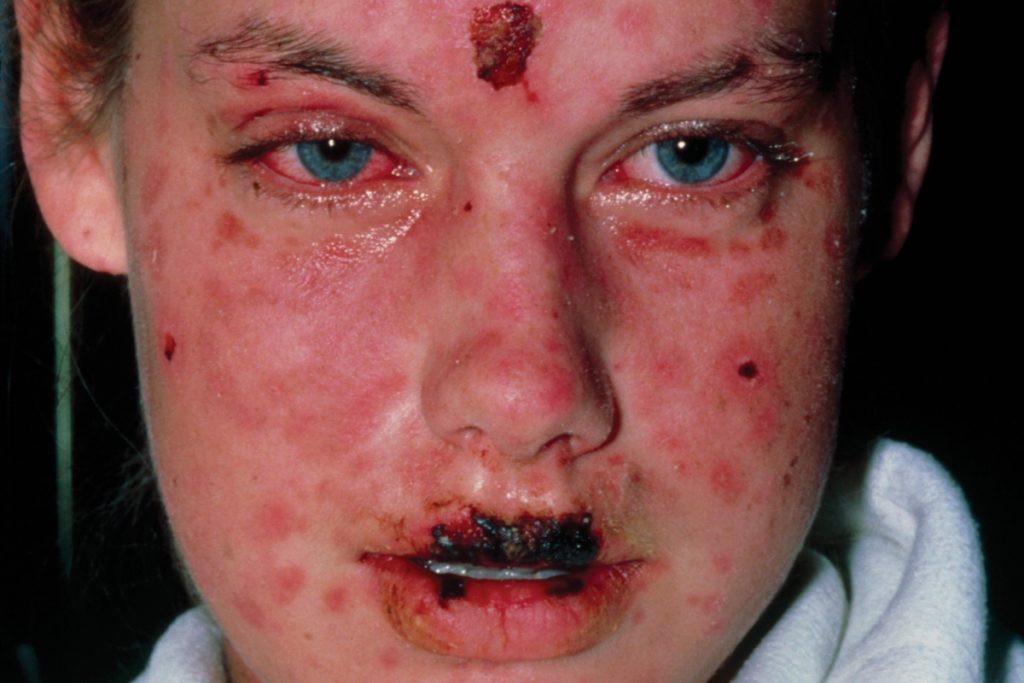
‘I’m so worried about my daughter. She’s coming to the end of a course of amoxicillin for a chest infection but she seems to be having a terrible reaction. She got a rash on her body yesterday and now it’s spread to her face. Her lips are all blistered, her eyes are red and she feels terrible.”
+
=
See end of article for answer
Dr Keith Hopcroft is Pulse’s medical adviser and a GP in Basildon, Essex
Answers
EASY Chronic paronychia: Loss of the cuticle and inflammation of the nail fold. The cause is multifactorial – typically involving immersion in water – and may be complicated by candidal infection. Treatment involves avoiding water and using emollients and topical antifungals.
MODERATE Shingles: The clues are the unilaterality of sensory symptoms followed by the rash. This could be mistaken for cellulitis (particularly with the systemic upset) but look closely and you can see blisters. The treatment involves oral acyclovir, analgesia and liaison with ophthalmology about ocular involvement.
HARD Stevens-Johnson syndrome: A rare mucocutaneous reaction to medication or infection. Patients can be severely ill, and a case of this sort would require hospitalisation for fluids, supportive care and possible steroids.
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.
Related Articles
READERS' COMMENTS [2]
Please note, only GPs are permitted to add comments to articles










Thanks for these.
For ophthalmic shingles, 3 safety net questions the ophthalmology team will ask:
1. Rash down to tip of nose (nasociliary nerve), 2 blurred vision. 3 photophobia.
Any of these indicates likely zoster iritis, and
needs review in eye casualty (usually steroid eye drops).
thank you , good review