How not to miss – myeloma
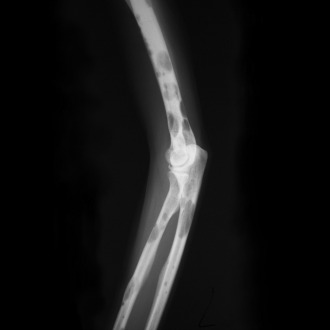
Worst outcomes if missed
• Death – delays in diagnosis predispose myeloma patients to early mortality. Analysis of data from around 3,000 patients in several UK MRC trials found that 10% of the patients died within 60 days of diagnosis. Only 51% of myeloma patients survive more than a year if diagnosed via A&E, compared to 81% diagnosed via GP referral.1
• Renal disease – may progress from reversible to irreversible if not dealt with promptly.
Five key questions
- Has the patient had repeat visits with constant tiredness/fatigue with possible anaemia?
- Has the patient previously presented with back, neck and rib pain or other bone pain that is not resolving?
- Does the patient repeatedly get infections?
- Has the patient lost a significant amount of height or weight recently?
- Has the patient presented with combinations of the above?
Epidemiology
Although myeloma is a ‘less common’ cancer, with a GP usually seeing only one or two cases in their career, it represents around 15% of haematological malignancies. The National Cancer Patient Experience Survey in England notes that over half of patients require at least three consultations with their GP before receiving a diagnosis, which is the highest of all cancers.2
Until recently, the prognosis for those diagnosed with myeloma was poor, but since the advent of new treatments the survival rate has improved faster than any other cancer, increasing six-fold since the 1970s.
The majority of cases are seen in those over 60 years, but around 10-15% of cases develop in those aged 45 and under. It is slightly more common in men than in women, with a higher incidence in people of Afro-Caribbean ethnicity.
Symptoms and complications
Myeloma is a malignancy of the plasma cells. This gives rise to diffuse bone marrow infiltration causing bone destruction, bone marrow failure and
the overproduction of a monoclonal antibody (paraprotein), which can be detected in serum and urine.
Myeloma UK, with the help of GPs and haematology consultants, has developed a Myeloma Diagnosis Pathway to aid GPs in recognising the signs of myeloma. See related files, on the right hand side, to download a copy of this.
Common symptoms and complications to look out for include:
• Myeloma bone disease – can result in acute or chronic pain, pathological fractures, spinal complications (with or without neurological complications) and even spinal cord compression. Be vigilant and aware of patients who present with sudden or persistent bone pain, particularly non-improving back, neck or rib pain. This is an often overlooked symptom, but when coupled with other potential markers should be investigated promptly to rule out myeloma.
• Anaemia – although fatigue and anaemia are common, anaemia is a key marker of myeloma when coupled with other symptoms. Normocytic normochromic anaemia should always be taken seriously and investigated, particularly if FBC shows unresolving haemoglobin levels of 20g/l below the lower limit of normal, or under 100g/l.
• Renal impairment – renal impairment is a common and potentially serious complication of myeloma, occurring at presentation in 20-25% of patients and in up to 50% of patients at some point during their disease. Symptoms include vomiting and diarrhoea, nausea, weight loss, more or less frequent urination, and difficulty urinating. Patients presenting with renal failure have a higher morbidity rate.
• Raised calcium – hypercalcaemia is present in around 30% of patients, usually when their disease is active. It is caused by increased breakdown of bone, which deposits itself in the blood, causing mild to more serious symptoms such as vomiting, nausea, constipation, confusion, bone pain, muscle weakness and polyuria.
In addition to the four common complications outlined above, GPs should also look out for the following:
• Prolonged or frequent infections.
• Hyperviscosity.
• Peripheral neuropathy.
• Weight loss or loss of appetite.
• Night sweats.
• Asthenia.
Spinal cord compression, severe hypercalcaemia and acute renal failure are all medical emergencies requiring immediate investigation and treatment. Do not delay if you suspect a patient may be presenting with one of these problems. As many as 31% of patients report being asymptomatic at the time of diagnosis, so it is imperative to follow up on abnormal laboratory results encountered in screening or testing for other potential diagnoses.3
Differential diagnoses
Differential diagnosis of myeloma includes other conditions that may cause similar symptom profiles, and other causes of abnormal laboratory results consistent with myeloma.
Connective tissue disorders, chronic infections and skeletal metastasis may have the same clinical presentation as multiple myeloma. Non-specific back pain is common in general practice – the following are red flags for myeloma:4
• Age over 50 years.
• Pain that is worse in supine position.
• Pain that is worse at night or awakens patient from sleep.
• Pain with a band-like distribution around the body.
• Pain that is not relieved with conventional methods (rest, NSAIDs, paracetamol).
• Associated constitutional symptoms (fever, weight loss, dehydration).
• Progressive neurologic deficit in lower extremities.
Differential diagnosis of abnormal laboratory findings will normally be guided by the pathologist. It is vital that the GP and the patient be aware of the importance of following up such results.
Other causes of paraproteinaemia include:
• Lymphoma.
• Monoclonal Gammopathy of Undetermined Significance (MGUS).
• Smouldering myeloma.
• Plasma cell leukaemia.
• Solitary plasmacytoma.
• Waldenstrom macroglobulinaemia.
Five red herrings
- Menopausal women who commonly experience aches and pains, night sweats and fatigue
- Paraproteinaemia due to other types of haematological dyscrasia such as lymphoma
- Patients with bone pain presumed to be related to existing osteoporosis, ageing or existing bone or joint disease or injury, which may mean pain is not investigated further
- Negative serum electrophoresis, as Bence Jones and non-secretory myeloma can only be revealed by checking for Bence Jones proteinuria
- Amyloid light-chain amyloidosis, a rare condition, which may show the laboratory features of myeloma
Investigations
The following tests should be performed in suspected myeloma:5
• FBC to check for anaemia, immunosuppression and thrombocytopaenia.
• ESR or plasma viscosity that may show raised levels.
• Calcium levels that may show raised levels.
• U&E and creatinine levels that may show impaired renal function.
• Serum protein electrophoresis, which will show raised serum globulin and
a presence of paraprotein.
• Urine protein electrophoresis and serum free light chain (SFLC) assay, if available, which may show light chains in the urine or an abnormal SFLC ratio.
It is important to note that the use of one of these tests is essential for detecting Bence Jones (light chain) and non-secretory myeloma.
Patients with suspected myeloma require urgent haematology referral.
Dr Anant Sachdev is a GPSI in palliative medicine in Bracknell, Berkshire. He is also cancer lead for Berkshire East and the Cancer Network, leading on the National Awareness and Early Diagnosis Initiative, working with Macmillan, Cancer Research UK and NHS England, and is involved clinically and strategically with CCGs and NHS England
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









