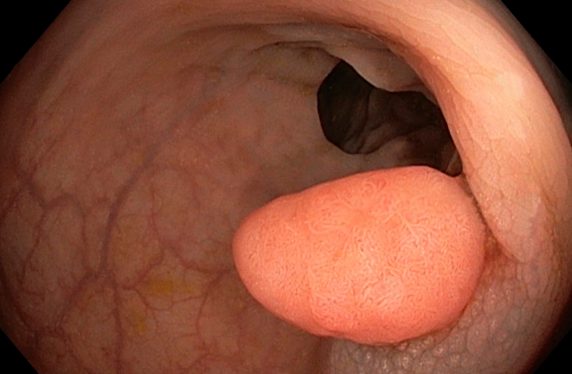
Case
A 32 year-old gentleman presents to his GP with a history of painless, bright red rectal bleeding. He is anxious as his mother and her brother died of bowel cancer, and his maternal grandmother died of uterine cancer, all in their forties. Physical examination, including rectal examination, is normal but because of the strong family history, the GP feels he warrants a two week wait referral. The subsequent colonoscopy confirms twelve adenomas, including a 3cm growth in the sigmoid colon. The patient returns to see his GP to discuss a genetics referral.
The problem
Colorectal cancer is the fourth commonest cancer in the UK and the second biggest cause of cancer death. The majority of colorectal cancer cases are sporadic, but less than 5% or so1 will have a strong genetic component. Lynch syndrome, or hereditary non-polyposis colorectal cancer (HNPCC), has an estimated population prevalence of one in 4402 and is characterised by an increased risk of colorectal cancer and other cancers such as uterine and ovarian, renal or bladder cancer, or other gut-related cancers such as stomach, pancreas or small bowel. People with Lynch syndrome have a high (50-80%) risk of colorectal cancer in their lifetime and women have a 30-60% risk of uterine cancer and a 10% risk of ovarian cancer.3
Features
There is a ‘3-2-1’ diagnostic rule for Lynch syndrome4:
- Three people, one of whom is aged under 50 with colorectal cancer (or other ‘Lynch cancers’)
- Across two generations
- One of whom is a first degree relative of the other
These diagnostic criteria are extended if the results of genetic testing are available. Lynch syndrome is caused by mutations in DNA mismatch repair genes MLH1, MSH2, MSH6 and PMS2. These are inherited on an autosomal dominant basis, meaning that a child of an affected parent has a 50% chance of receiving the gene and suffering from the condition. Although not all cancer families will have established gene defects, the large majority (80%) will, and this allows genetic screening of individual members of families to either provide reassurance they are unaffected or establish a surveillance program that will minimise their lifetime risk of cancer.
Diagnosis
Although the diagnosis of suspected Lynch syndrome can be made clinically on the basis of family history, the only way of confirming the diagnosis is through colonoscopy and genetic testing. Colonoscopy not only allows optical diagnosis (finding and classification of polyps) but also by removing the polyps reduces the risk of colorectal cancer. Genetic testing is preceded by extensive counselling by a trained health professional, as diagnoses such as Lynch syndrome can have far-reaching consequences for the individual. Recently, NICE5 has requested that all colorectal cancers removed at surgery are tested for the presence of mismatch repair proteins indicative of Lynch syndrome. In this way, more Lynch families will be diagnosed and surveyed before they develop cancer.
Other polyposis syndromes do exist, such as familial adenomatous polyposis or Peutz-Jeghers syndrome. These are both much rarer than Lynch syndrome and are distinguished usually by clinical features as well as different genetic expression.
Management
Families identified as having Lynch syndrome should have a colonoscopy every 18 months until the age of 75 starting, at age 25.1 If colorectal cancer develops, the risk of developing a metachronous cancer (in other words, a colorectal cancer occurring at a later date) is higher and some patients will require an extensive resection removing the majority of their colon. A proportion of patients may request a subtotal colectomy to minimise their risk. Screening will also be required for other associated cancers such as uterine and ovarian, and again some patients will elect to undergo prophylactic surgery. Aspirin can be used to reduce the risk of cancer developing in someone with Lynch syndrome6, but the benefit needs to be balanced against the risk of bleeding or haemorrhagic stroke.
In general practice, the most important requirement is to be aware of the heightened risk associated with Lynch syndrome over a variety of cancers. Colorectal cancer can occur at a younger age in this group, and therefore the diagnosis needs to be considered in patients with a high-risk family history.
Dr Ed Seward is a consultant gastroenterologist at the University College London Hospital
References
- Cairns SR, Scholefield JH, Steele RJ et al. Guidelines for colorectal cancer screening and surveillance in moderate and high risk groups (update from 2002) Gut 2010;59:666-690
- Rubenstein JH, Enns R, Heidelbaugh J et al. American Gastroenterological Association Institute Guideline on the Diagnosis and Management of Lynch Syndrome. Gastroenterology 2015;149:777-782
- Sehgal R, Sheahan K, O’Connell PR, et al. Lynch syndrome: an updated review. Genes (Basel). 2014;5(3):497-507
- Vasen HF, Mecklin JP, Khan PM, et al. The International Collaborative Group on Hereditary Non-Polyposis Colorectal Cancer (ICG-HNPCC). Dis Colon Rectum 1991;34:424-5
- Molecular testing strategies for Lynch syndrome in people with colorectal cancer Diagnostics guidance [DG27] Published date: February 2017
- Burn J, Gerdes AM, Macrae F, et al. Long-term effect of aspirin on cancer risk in carriers of hereditary colorectal cancer: an analysis from the CAPP2 randomised controlled trial. Lancet. 2011;378(9809):2081-7