CPD: Key questions on peripheral arterial disease
Key points
- PAD has a five-year mortality of 25%, which is very high – by comparison six-year CAD mortality is half that, at 13%
- PAD is a marker for future CV events and risk factor modification is crucial, though often neglected and suboptimal
- Risk factor targets for modification are the same as those for CAD
- Although some patients present with classical symptoms, two-thirds do not, so a high level of suspicion should be held for all inexplicable cases of leg, buttock or foot discomfort
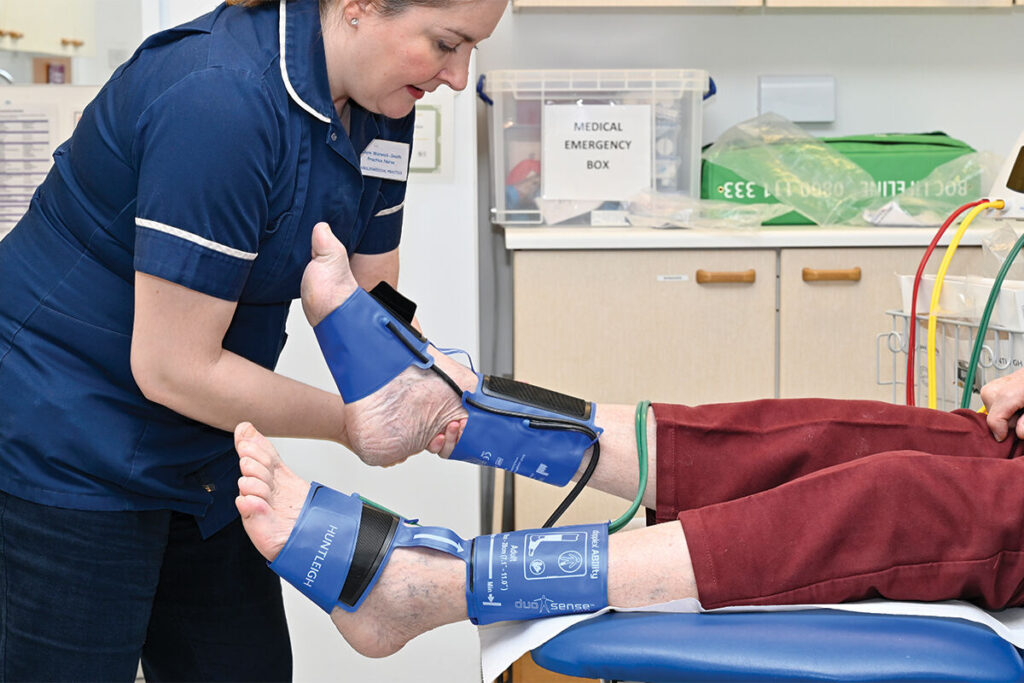
- ABPI is easy to do and is the gold standard test for primary care diagnosis of PAD
- Statin treatment adherence is poor in PAD patients but can be improved by explaining it helps claudication symptoms and reduces the likelihood of amputation
- Both acute and worsening CLI are clinical emergencies requiring immediate referral to secondary care
Professor Jill Belch is professor of vascular medicine at the University of Dundee and President of the European Society of Vascular Medicine
Q: What are the key symptoms? How can they be distinguished from other causes of leg pain on exertion?
A: Atherosclerotic peripheral arterial disease (PAD) may present as intermittent claudication (IC) or as critical limb ischaemia (CLI). The latter can be acute (due to plaque rupture and emboli) or chronic. IC presents as ‘angina’ of the legs – pain on walking, relieved by rest. The commonest site of pain is the calf, but most patients with PAD are asymptomatic. They may have angina, dyspnoea, arthritis or other walking-limiting disease that means they do not reach claudication distance.
Under a third of patients with PAD report the typical symptoms of IC, which mainly relate to leg muscle discomfort on exertion that is relieved with rest.1 Many patients present with atypical symptoms, including leg fatigue, difficulty walking and leg pain, that are not typical of claudication.2 This makes diagnosis difficult as many other conditions, such as musculoskeletal disorders, present in this way.
Classical IC presents as pain in the muscles of the leg on walking, the site depending on which vessel is affected. It may present in the soles of the feet with occlusions in the lower leg, or the gluteal region with occlusions in pelvic arteries. More usually, however, patients experience pain in the calf from iliac, femoral or popliteal occlusions, especially going up hills or stairs, where the vessels are too narrow to get sufficient blood to the exercising muscle. Stopping for a period resolves the pain. Although described as ‘angina of the legs’ it is actually linked to a higher risk of CV events than angina, or even myocardial infarction (MI).3,4
It is important, in atypical leg pain, where other causes have been excluded, to consider ankle-brachial pressure index (ABPI) measurement to test for PAD. Even asymptomatic or atypical PAD confers a huge risk of cardiovascular (CV) events, although no cost-benefit analysis of screening for PAD in those at risk has been done. Those at greatest risk of PAD are people aged 50 years and older with two or more CV risk factors such as diabetes, dyslipidaemia, obesity, elevated inflammatory markers and smoking history.5
Click here to read the full article and download your certificate logging 2 CPD hours towards revalidation
Not a Pulse Learning member? Click here to join and gain access to over 400 CPD modules
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.













