The information – venous insufficiency
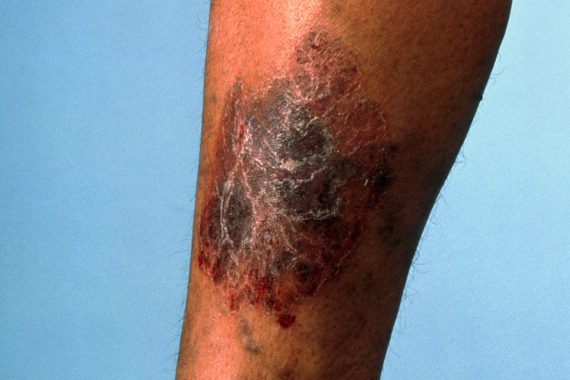
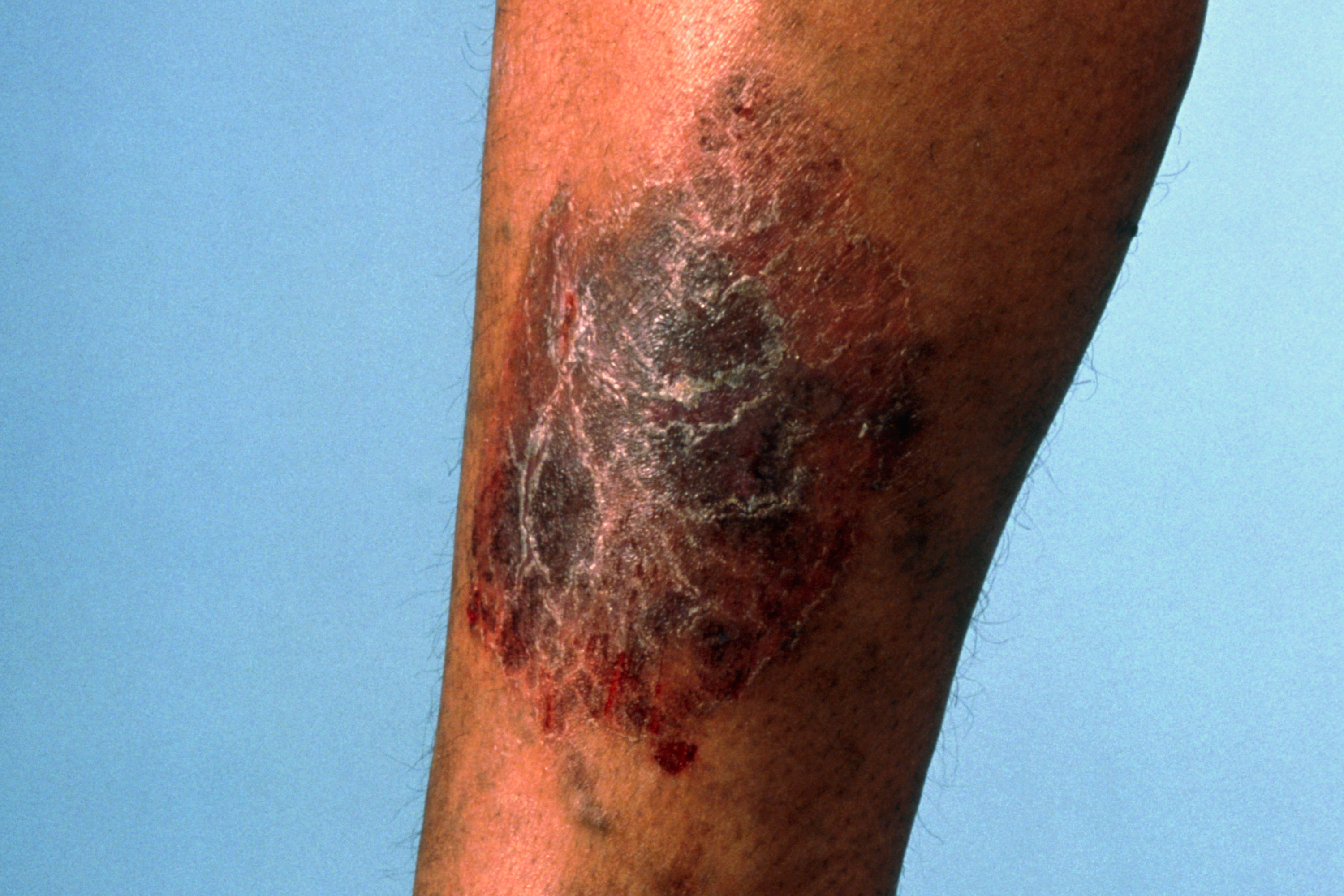
The patient’s unmet needs (PUNs)
A 75-year-old lady attends with the opening gambit, ‘You’ve got to do something about my legs’. For many years she has suffered what sounds like mild gravitational oedema, but in the last year or so she has attended increasingly frequently because her lower legs have felt itchy and uncomfortable. A variety of topical treatments have proved ineffective, and she is not able to tolerate support stockings. Examination reveals skin changes consistent with chronic venous insufficiency, although there are no obvious varicose veins. She volunteers that she is terrified of developing ulcers, which her mother suffered. ‘If it’s all down to my veins, couldn’t I have an operation on them?’ she asks.
The doctor’s educational needs (DENs)
What are the key features of venous insufficiency?
Venous insufficiency in its broadest sense is the failure of the mechanisms that allow for adequate drainage of blood from the legs, leading to persistent elevated pressure in the venous system.
The key features are skin changes (pigmentation, eczema and ulceration) and symptoms (pain, tightness, aching, itching).
The classification of patients with venous insufficiency is based on the CEAP classification system. C stands for clinical and is the part used most frequently. E is etiological, A is anatomical and P is pathophysiological.
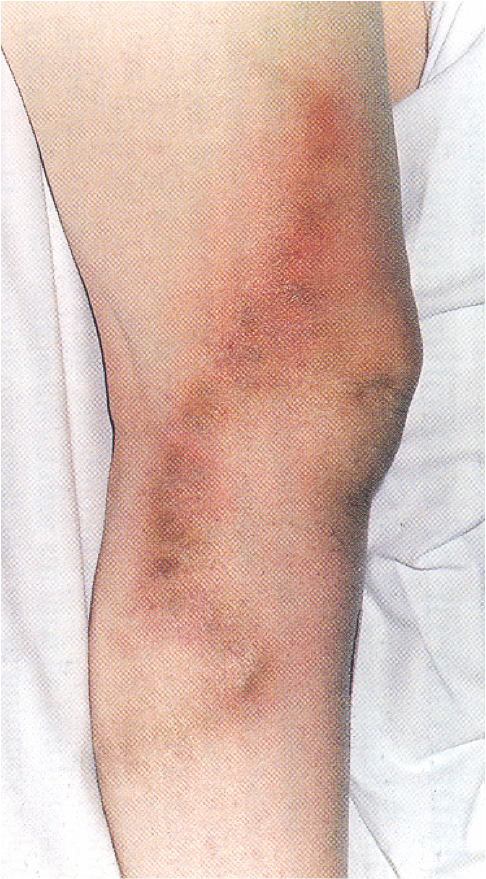
Clinical classification
C0 – no visible or palpable signs of venous disease
C1 – telangiectasies or reticular veins
C2 – varicose veins
C3 – oedema
C4a – pigmentation or eczema
C4b – lipodermatosclerosis or athrophîe blanche
C5 – healed venous ulcer
C6 – active venous ulcer
S – symptomatic, including ache, pain, tightness, skin irritation, heaviness, and muscle cramps, and other complaints attributable to venous dysfunction
A – asymptomatic
Etiology classification
Ec – congenital
Ep – primary
Es – secondary
En – no venous cause identified
Anatomic classification
As – superficial veins
Ap – perforating veins
Ad – deep veins
An – no venous location identified
Pathophysiologic
Pr – reflux
Po – obstruction
Pr,o – reflux and obstruction
Pn – no venous pathophysiology identifiable
The C component of the classification is commonly used without the other components. As a patient with venous insufficiency moves from C0 through to C5/6, they develop progressive signs of chronic venous insufficiency. Anyone at a level of C4 or above is considered to have chronic venous insufficiency.
In practice, if a patient presents with pigment change in the gaiter region and symptoms, with visible veins (secondary) and a scan which confirms only superficial venous reflux, they would be classified C4aS, Es, As, Pr
Does the absence of obvious varicosities shed doubt on the diagnosis or alter the management?
No. As can be seen with the classification above, varicose veins are not the sole component. In many cases, the patients may have developed venous insufficiency secondary to deep venous disease or previous DVT. In the latter group, this will come under the heading of post-thrombotic syndrome – venous insufficiency secondary to previous thrombosis – so it is important to consider all the possible causes.
In patients with only telangiectasia and no visible veins, there is an 80% chance that there will be an underlying problem of venous reflux in the superficial system, despite the absence of varicose veins.
In particular, it is useful to consider the diagnosis of venous claudication in patients who describe a bursting sensation in their lower calf on exercise.
Venous claudication is pain induced by exercise secondary to obstruction in the venous outflow of the leg. Like arterial claudication, it settles with rest but typically takes longer. The patients are often younger, without arterial risk factors, and may have had a previous DVT. The pain, unlike arterial claudication, is a bursting sensation rather than a cramp.
What are the most effective topical treatments?
Topical treatments are rarely effective alone, and if symptoms and signs of chronic venous insufficiency are present, then the patient requires treatment of the underlying venous disorder.
Topical treatments are aimed at treating the skin effects of stasis dermatitis, which may manifest as varicose eczema. Mid-potency topical corticosteroids may be effective in reducing inflammation and itching during acute flare ups, but care must be taken to avoid prolonged use.
Long-term topical management is through the use of bland emollients to maximise epidermal moisture.
When using support stockings, what grade and length should be used?
There is no evidence to support the use of stockings to manage varicose vein-related venous insufficiency, unless the patient is unsuitable or unable to have appropriate intervention.
In patients with post-thrombotic syndrome, they may play an important role in managing swelling and oedema. However, if there is an obstruction to venous outflow from the leg, for example, occluded iliac veins, stockings may make the pain worse.
If stockings are used, it is ideal to aim for thigh length class 2 compression stockings, but these are very difficult to get on, particularly for elderly patients, and are poorly tolerated. This is why knee length class 2 compression is often more effective.
If the patient has active ulceration, they should be placed in compression bandaging by an appropriately trained nurse specialist.
Is it always necessary to undertake Doppler assessment of the arterial circulation first?
No, but it is always necessary to do an assessment of the pulses. If pulses are easily palpable, then a Doppler assessment is not necessary. If the patient has oedema and the pulses are not easily palpable, then a Doppler assessment is useful. If there is any doubt about the patients arterial circulation, particularly in the presence of risk factors for arterial disease, then refer for a vascular opinion before using stockings or compression bandaging.
Is there any way of predicting who is most likely to go on to suffer ulceration?
Approximately 3% to 6% of people with varicose veins will go on to develop venous ulcers, but there is no way of predicting who falls into this group.
Which patients should be referred with a view to surgery?
Refer patients who have bleeding related to varicose veins immediately.
Refer if they have any of the following:
- Symptomatic primary or symptomatic recurrent varicose veins.
- Lower limb skin changes (for example, pigmentation or eczema).
- Superficial vein thrombosis.
- A venous leg ulcer.
- A healed venous leg ulcer (not previously seen or treated by a vascular surgeon).
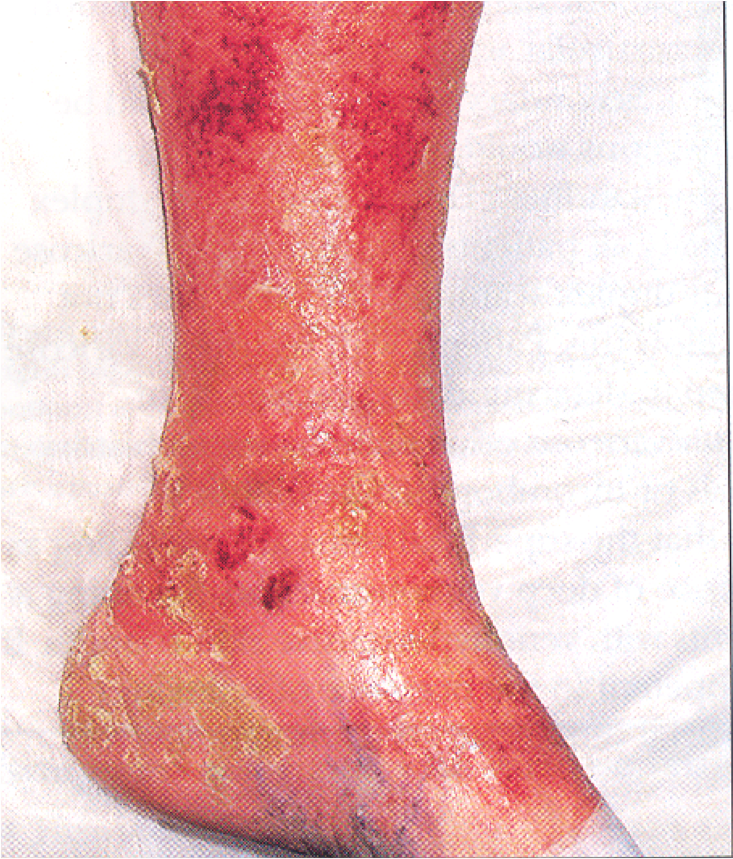
Key points
Cause
The basic cause is persistent long standing failure of adequate venous drainage from the leg
Epidemiology
Prevalence rises with age and may be as high as 40% of the population. Risk factors for developing veins are largely congenital but may develop during pregnancy and increase with obesity.
Clinical features
History or clinical presence of venous disease associated with skin changes predominantly pigment deposition, eczema and ulceration.
Management
Skin changes of stasis dermatitis and eczema can be controlled with topical ointments and symptoms may be controlled with compression stockings, but ultimately treatment relies on dealing with the underlying cause, be that superficial venous reflux, deep venous reflux or obstruction.
Mr Stephen Black is a consultant vascular surgeon and clinical at Guy’s and St Thomas’ NHS Foundation Trust
Further reading
NICE. CG168: Varicose veins in the legs. London: NICE; 2013
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.













