Continuing our series on clinical scenarios that can be mishandled in primary care, Dr Peter Bagshaw advises against routine swabbing of venous ulcers
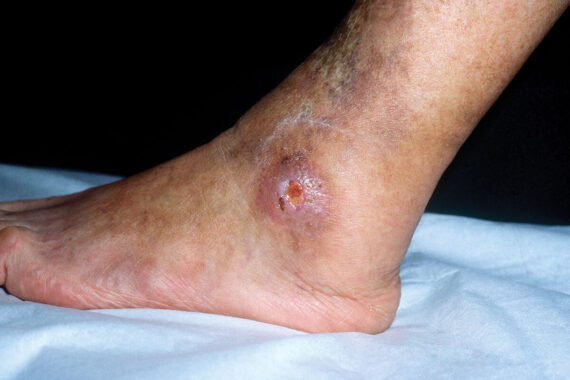
Mrs R is a 92-year-old patient in a care home with chronic venous ulcers above both ankles. Following Doppler testing the community nurse has been applying compression bandaging, but after two months there is little progress. The nurse has taken a swab which shows Staphylococcus aureus and mixed anaerobes. She requests an antibiotic prescription in order to aid healing. There is no increase in pain, surrounding erythema or fever, but the bandaging is soaking through quickly and the nurse, who is very experienced, is worried the patient has an infection.
The reality
Although traditional teaching and intuition is that the presence of bacteria delays healing, there is no evidence for this. Swabs may indicate colonisation of the ulcer by bacteria, but this is not the same as infection. Infections need treatment but are diagnosed clinically, so swabbing wastes time and resources, and risks overtreatment.
The issue
Routine swabbing is of no benefit. Overtreatment with antibiotics is clinically unnecessary, and also carries the risk of increasing drug-resistant bacteria, which will be more difficult to treat if the patient does develop a significant infection. Current guidelines recommend that antibacterial preparations should be used only in cases of clinical infection, not for bacterial colonisation.
The evidence
All the papers on this stress the crucial difference between bacterial colonisation and infection. As Moore states, ‘bacteria can be cultured from all venous leg ulcers regardless of healing status’.1 In a study of weekly sampling of 178 ulcers, they found Staphylococcus aureus in 64.3% of assessments, Corynebacterium striatum in 60.6%, Pseudomonas aeruginosa in 32.6%, and Proteus mirabilis in 16.1%.1 The authors concluded that ‘no single species or the presence of anaerobes and increasing diversity of bacterial species, previously thought to be predictive of impaired healing, was shown to be associated with healing outcome’.
A Cochrane review found the same thing.2 NICE is even clearer: ‘most leg ulcers are not clinically infected but are likely to be colonised with bacteria. Antibiotics do not help to promote healing when a leg ulcer is not clinically infected. Offer an antibiotic for adults with a leg ulcer only when there are symptoms or signs of infection’.3
So if antibiotics are only indicated for infection, might swabs be useful in helping us know if a significant infection is present? Apparently not: Finlayson found ‘no studies reporting a significant relationship between clinical signs and symptoms of infection and microbiological results, including the qualitative and quantitative results.’4 He went on to stress that infection is a clinical diagnosis, and found the most useful criteria to be increasing or altered pain in the ulcer area, malodour, increase in ulcer area, wound breakdown, delayed or non-healing, erythema and increase in local temperature. Pain is the most reliable symptom. Blokhuis-Arkes et al came to the same conclusion.5
Avoiding a clanger
If this is an issue in your practice, consider a consensus approach among the GPs. Agree not to respond to lab results with automatic antibiotic prescriptions. You might arrange an educational session or produce guidelines for community nurses, based on NICE best practice.
Caveats
Swabbing is appropriate if there is no response to empirical antibiotics and we need to identify a pathogen in active infection. NICE recommends sending a sample (from deep within the leg ulcer after cleaning) for microbiological testing if signs of the infection are worsening or have not improved following a completed course of antibiotics.3
Remember that infection not only delays ulcer healing, but can lead to cellulitis and sepsis. Clinical infection is important and needs treatment, but it is a clinical diagnosis, regardless of swab results.
Key points
- Antibiotics should only be used for infection, not colonisation
- Routine swabbing of chronic venous ulcers is of no benefit as they reflect colonisation rather than infection
- Diagnosing infection is a clinical process, not a bacteriological one
- Increasing pain is the most reliable pointer to infection, as are malodour, increase in ulcer area, wound breakdown, non-healing erythema and increase in local temperature
Dr Peter Bagshaw is a GP in Somerset
References
- Moore K et al. Surface bacteriology of venous leg ulcers and healing outcome. J Clin Pathol 2010;63:830-4. Link
- O’Meara S et al. Antibiotics and antiseptics for venous leg ulcers. Cochrane Database of Syst Rev 2014 Jan 10;(1):CD003557. Link
- NICE. Leg ulcer infection: antimicrobial prescribing. 2020. Link
- Finlayson K, Edwards H. The diagnosis of infection in chronic leg ulcers: A narrative review on clinical practice. Int Wound J 2019;16:601-20. Link
- Blokhuis-Arkes M et al. Rapid enzyme analysis as a diagnostic tool for wound infection: Comparison between clinical judgment, microbiological analysis, and enzyme analysis. Wound Repair Regen 2015;23: 345-52. Link
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens












Headline looked odd and grated until the end of the article- “Can you prescribe antibiotics please” would have been clearer way to explain scenario – is it really a clinical clanger? More a dilemma ?
Noctors will be fuming when you refuse.
GPs already know this, but here is a classic case of the difference between the Ideal and Real World.
– Ideal World- nurse reports ulcer (plus/minus photo), GP advises swab not needed, nurse then insists on home visit, GP squeezes in visit, repeats advice, nurse revisits, disagrees, and requests repeat visit if swab not deemed necessary, and so the vicious circle keeps going round, with all parties unhappy……..patient thinks nothing being done, nurse angry with GP, and GP fuming in traffic, day ruined, doing pointless meaningless home visits and considering early retirement
– Real World- nurse swabs wound, GP issues flucloxacillin, everyone happy (except the idealists).
Triple the number of GPs and put some of them purely on home visit duty then you can have your Ideal World.
But in 2023 when the last few remaining GPs are being pulled in all directions all day long, please accept we will continue to take the path of least resistance, even if it doesn’t meet “best practice” standards.