Sponsored CPD: Eczema and psoriasis – the mental health link

GP Dr Nisa Aslam explores the impact of eczema and psoriasis on mental health and the importance of timely and appropriate treatment in management of these skin conditions
Eczema (also known as dermatitis) and psoriasis are inflammatory dry skin conditions, which can affect people from infancy to old age. Although both conditions can occur at any age eczema often starts in childhood whereas psoriasis usually manifests in early adulthood or later. The National Eczema Society estimates that the most common form of eczema, atopic eczema, affects one in 5 children and one in 10 adults in the UK whilst psoriasis affects about 2% of the population.
These skin conditions are debilitating for both physical and mental health.
This CPD module will update your knowledge on the similarities and differences in presentation between eczema and psoriasis before focusing on the lesser understood mental health impacts of these conditions.
Learning objectives:
- Summarise key differences and similarities in presentation and symptoms between psoriasis and eczema
- Understand and acknowledge the mental health impacts of these skin conditions
- Identify therapies for mental impacts of eczema and psoriasis and know how to refer patients
- Explain the principles of stepped care in eczema and psoriasis
- Understand the need for immediate treatment of flares in both conditions
This module is sponsored by Typharm Ltd.
Eczema and psoriasis: presentation and symptoms
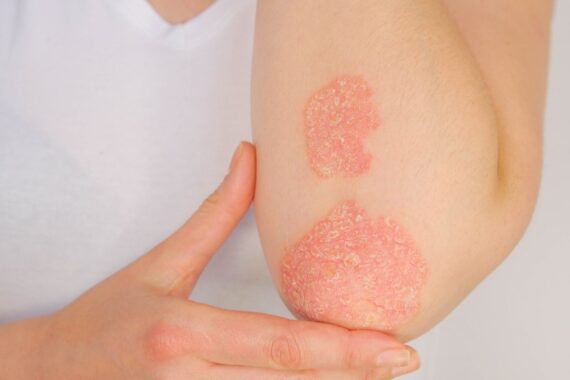
Both eczema and psoriasis cause a rash, with patches of raised, red, itchy skin. They can appear in similar places on the body like the hands and scalp and can become secondarily infected. It is vital for the GP to see the patient in the first instance to ensure the diagnosis is correct. For people without medical training these conditions can be difficult to tell apart.
A key difference between psoriasis and eczema is the underlying cause. Psoriasis is an autoimmune condition in which the epidermal cells grow too rapidly forming a white scale on the surface of the skin. The causes of eczema are more complicated, with both genetic and environmental factors (eg, allergens, pollutants) playing a role. In patients with eczema there is generally a family history and if both parents have eczema there is a 50% chance that the offspring will develop it.1
Both psoriasis and eczema cause itchiness. In eczema the skin is unbearably itchy – the urge to scratch can be irresistible and during a flare-up it can also be red, cracked and raw and the skin may bleed. Psoriasis tends to cause milder itching and in some less common types of psoriasis a painful burning sensation. Psoriasis commonly occurs on the scalp, elbows, knees, buttocks and face. Eczema can occur at these sites but most commonly occurs behind the knees or inside the elbows. Symptoms of psoriasis are often improved by ultraviolet (UV)B light from the sun as UVB light can slow down the growth of skin cells. Eczema by comparison may not respond well to the heat of summer as perspiration can cause flare-ups.
What is common to both skin conditions is their impact on mental health. Together with the painful and itchy physical symptoms, many children and adults experience related sleeplessness, anxiety, depression and other mental health problems. Stress and anxiety can in turn trigger flare-ups.
Impact of eczema and psoriasis on mental health
Substantial evidence demonstrates an association between eczema or psoriasis and several mental health issues including depression, anxiety and feeling suicidal.2,3 Data from the UK Clinical Practice Register Datalink (CPRD) also showed that both eczema and psoriasis are linked with anxiety and depression. Poor sleep quality was a risk factor particularly in eczema.4 An analysis of 230,047 patients in the UK Biobank study with linked primary care data found that having eczema or psoriasis was associated with higher odds of having anxiety or depression.5 Limited evidence from cross-sectional and case studies suggests an association between psoriasis and eczema and severe mental illnesses including bipolar and schizophrenia.6
It is important to acknowledge and address the psychological impact of skin conditions. Poor mental health is unhelpful for overall wellbeing. Patients who are anxious and depressed may not stick to their treatment.
Click here to read the free full article and download your certificate logging 1.5 CPD hours towards revalidation
Not a Pulse Learning member? Click here to join and gain access to over 400 CPD modules
Dr Nisa Aslam is an NHS GP in Hertfordshire and Chief Medical Officer for a health data company. Dr Aslam has a special interest in dermatology across the areas of psoriasis, eczema and dermatitis.
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.















