The information – hidradenitis suppurativa
The patient’s unmet needs (PUNs)
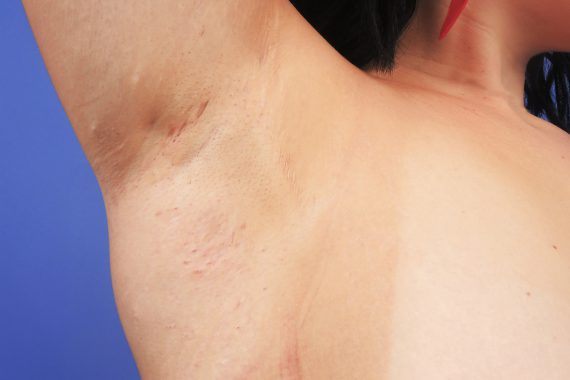
‘I can’t believe I’ve got these boils again,’ says your next patient, a 30 year old lady. You see from her records that she has attended on numerous occasions over the last year or two for ‘boils’ or ‘abscesses’ in her groin and, occasionally, her axillae. On one occasion, these needed incision and drainage, but the other episodes have been treated with short courses of antibiotics. Examination reveals tender, red, lumpy areas in her groin, with evidence of scarring and sinuses. She has no significant medical history but she is a heavy smoker. You explain that you think she has hidradenitis suppurativa. ‘Why have I got this?’ she asks. ‘Is there anything I can do? Or do I need to see a specialist?’
The doctor’s educational needs (DENs)
What causes hidradenitis suppurativa? What are the key features that should suggest the diagnosis?
Hidradenitis suppurativa (HS) is a chronic inflammatory skin disease that presents with painful, inflamed nodules of the skin. These recur and persist at specific sites, often discharging pus and progressing to sinus formation and scarring. The body sites affected are those where the apocrine glands predominate, typically the axillae, groin and breasts. HS is a disease of the hair follicle, with histology frequently showing inflammation and follicular occlusion and apocrine glands involved only as a secondary process.
The cause of HS is still debated but appears to be multifactorial. There is a familial tendency in some patients and specific genetic mutations have been identified in some families. A strong association with smoking and obesity, confirmed by several studies, suggest environmental factors play an important part in initiating the disease. Despite the painful and inflamed appearance of nodules during an acute flare, these are not true boils and aspiration for culture shows they are sterile in most cases. Anaerobic bacteria are present in the chronic sinuses of HS, and it is thought that altered immune response to commensal bacteria may be the mechanism for continued inflammation.
HS is not a rare disease, with an incidence of around 1% in Western populations. The diagnosis is suggested by the triad of:
- Typical lesions – painful nodules, discharging lesions and sinuses
- Typical sites – commonly groin, axillae and breasts but buttocks, perineum, lower abdomen and neck are also characteristic
- Typical course – recurring or non-healing at the same sites over months and years, despite short courses of antibiotics
In many patients this is a disease of flares, with variable levels of pain and itch from scarring and persisting lesions between exacerbations. It is approximately three times more common in women than men, although some slim men can have a severe variant of the disease.
What is the differential diagnosis? Is it associated with any underlying illness such as diabetes?
The presentation is characteristic in most patients though frequently they have had the condition for months or years before diagnosis, either through delay in presenting to a doctor or having each episode treated as an individual ‘boil’. Boils recurring in sites not typical of HS should prompt investigation for underlying causes such as diabetes and immunodeficiency. Recurring boils in healthy young people on atypical sites can rarely be due to PVL-positive Staphylococcus aureus, which is diagnosed by sending in a bacteriological swab from a lesion and specifically requesting testing for this organism.1
HS is associated with increased risk of metabolic syndrome, but diabetes does not cause HS. Other aspects of metabolic syndrome, such as elevated serum lipids and hypertension, are also commoner in HS and should be screened for. Patients with HS have significantly increased cardiovascular risk, possibly due to the effects of chronic inflammation, compounded by the prevalence of smoking and obesity.2
What self-help and lifestyle measures should be recommended?
HS has a strong association with a BMI >30 (in 80% of patients). Obesity is thought to worsen HS through hormonal factors, particularly increased androgens in women, and by friction of skin folds. Clinical experience suggests HS tends to improve in moderately obese patients who manage to reduce their weight. In patients with very high BMIs, there is some evidence that dramatic weight loss causing pendulous skin folds actually worsens HS unless these skin folds are removed and subsequent improvement can occur, so counselling patients about this is important3 .Weight reduction also helps reduce the risk of developing metabolic syndrome.
Smoking is also strongly associated with HS, with 80% of patients being current or former smokers. There is mixed evidence regarding whether stopping smoking improves established HS, but it appears smoking is one of the triggers for the onset of the condition in susceptible patients. In view of the raised cardiovascular risk in HS patients, stopping smoking is important despite uncertainty about benefits on disease severity.2
HS can be a debilitating disease that lasts for decades, so depression is common and should be screened for. Patients may benefit from guided self-help for low mood and contact with patient organisations such as the Hidradenitis Suppurativa Trust.4,5
How effective are long-term antibiotics in this condition? Which ones should be used and for how long? What other medical treatments are helpful?
Standard courses of penicillin-type antibiotics are not helpful in HS. Long courses of tetracycline-type antibiotics and erythromycin can be effective in controlling mild to moderate HS. Often these need to be given for at least four to six months. Mild HS may respond to lymecycline 408mg daily, but my clinical experience is that doxycycline 100-200mg daily is required in more severe disease or those with a higher BMI. Once HS is controlled, treatment can be stepped down to daily maintenance use of topical clindamycin gel, which is also useful for mild HS where patients can’t tolerate oral antibiotics. Erythromycin 500mg twice daily is a useful alternative if tetracyclines are contra-indicated.
Metformin (500mg-1500mg daily, off-licence) can be helpful in some women with HS, either alone or as well as antibiotics, due to its anti-androgen effects. Choice of contraception is important in women, with less androgenic methods such as the combined oral contraceptive pill (COC) being less likely to worsen HS. Many women will have risk factors that make the COC unsuitable, and for these the levonorgestrel IUS would be a good choice.1
Many people with HS struggle with discharging lesions in skin creases. The surrounding skin often gets macerated, and pain and odour can be hard to manage. Standard dry dressings often cause skin trauma, so ‘gentle border’ dressings, with an absorbent foam layer may be required. Odour, often due to anaerobic bacteria, can be improved with specialised dressings containing charcoal. Pain and itch, which can be debilitating even between flares, should be treated appropriately. Antidepressants should be considered in patients whose mood has not improved with other measures.
Secondary care treatments for HS include unlicensed use of actitretin and dapsone and courses of combined rifampicin and clindamycin. Adalimimab has recently been licensed for HS in patients unresponsive to standard treatments.
Which patients require referral? Should they be sent to a dermatologist or a surgeon?
It’s helpful to grade HS severity according to how much scarring has taken place. The Hurley system grades HS with no scarring as stage 1, HS with scarring in one or more body sites as stage 2 and if there are widespread interconnecting sinuses and active lesions throughout an area, it is stage 3.5 Hurley stage 1 HS can usually be managed in primary care with oral antibiotics and lifestyle interventions. Patients who have failed to improve on two different antibiotics for a minimum of three months each should be referred to dermatology. Where patients have Hurley stage 2 HS that is fairly mild, then treatment is the same as stage 1. However, if a number of sites are affected, or there are frequent flares despite treatment, then dermatology referral is appropriate. Patients who have Hurley stage 3 HS at presentations require specialist input and should be referred immediately.
Generally, dermatology referral is more appropriate than surgical referral for HS patients. Localised excisions of isolated lesions have a high risk of recurrence of the lesions and are only useful as part of a plan to control the underlying disease. More extensive surgery involving excision of large areas of skin, with grafting or flap formation, can be transformative for patients but needs to be carefully planned with dermatology input for ongoing management.
References
- Collier F, Smith RC, Morton CA. Diagnosis and management of hidradenitis suppurativa, BMJ 2013; Apr 23:346
- Dufour DN, Emtestam L, Jemec GB. Hidradenitis suppurativa: a common and burdensome, yet under-recognised, inflammatory skin disease. Postgraduate Medical Journal 2014; 90:216-221.
- Javorsky E et al. Hidradenitis suppurativa : Patient experiences with bariatric surgery, JAAD April 2013 ; Vol 68: Issue 4 Supplement 1 http://dx.doi.org/10.1016/j.jaad.2012.12.370
- www.hstrust.org -site for patients
- www.hidradenitissuppurativa.co.uk incorporates two sites- one for health professionals and one for the public.
Dr Fiona Collier is a GP in Clackmannanshire, a GPSI in dermatology at NHS Forth Valley and a member of the Medical Advisory Board of the HS Trust.
Competing interests: Dr Collier has participated in an observational demographic study of HS sponsored by AbbVie, with no personal financial interest.
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.













