Head and neck clinic – neck lumps
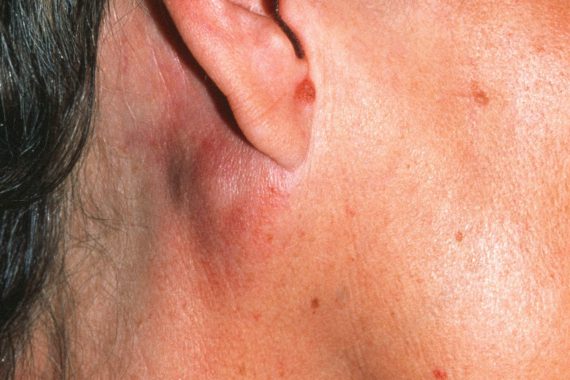
Case
A previously healthy 40-year-old man presents to the GP with a three week history of an enlarging mobile, firm, painless lump in the left upper lateral neck. There is no systemic upset (specifically no B symptoms – night sweats, fever, loss of weight), and no other head and neck symptoms such as sore throat or salivary gland obstruction. He smokes 20 cigarettes a day and has a moderate alcohol intake.
Examination reveals a firm 2cm mass deep to the skin and sternomastoid muscle in the left upper neck with no other findings on neck palpation. Examination of the oral cavity and throat is also unremarkable. Routine blood tests including FBC, ESR, EBV and U&Es are all normal. After urgent referral a diagnosis of tongue base squamous cell carcinoma with metastasis to the upper neck nodes was made.
Features
When considering any neck lump, it is important to have a clinical impression at an early stage as to whether the lump might be malignant. The short history, absence of other head and neck symptoms (including upper respiratory tract infection, swelling relating to eating, absence of dental or skin infection) and that he is a smoker should raise suspicion and prompt early referral to the local neck lump clinic, preferably using the two week wait pathway.
In contrast, many neck lumps that are clearly non-malignant are still being referred urgently, including lipomas and sebaceous cysts that in some cases have been present for years. In one example a calcified TB neck node which had been unchanged for 75 years was referred on the two week pathway.
Taking a simple history should give you some idea of how long the lump has been present and whether or not it is enlarging. General enquiry about systemic upset, other lumps (including axillary, inguinal lymphadenopathy) will also help to determine whether the lump is most likely related to head and neck pathology or is manifestation of a systemic disease such as a lymphoma. Given that 300 of the 800 total body lymph nodes are found in the head and neck, many systemic diseases can present with neck lymphadenopathy. Most solitary lumps in the upper lateral neck are unlikely to be metastatic from a primary below the clavicle (such as lung or breast), which is not the case with a low neck lump presentation (remember the classic supraclavicular Virchow node from a GI primary?).
A solitary upper neck lump is often indicative of pathology in the upper aero-digestive tract and these lumps can be malignant in any age. The important differential diagnosis to exclude is metastatic squamous cell carcinoma. Several features should raise your suspicion. Malignant nodes enlarge progressively and are usually painless and not associated with other symptoms (many primary head and neck cancers are painless in the early stages). The nodes feel firm on palpation while lymphoma nodes often feel rubbery and tend to be multiple from an early stage. Lymphoma can present at any age but typically in young adults (classic Hodgkin’s disease) and the elderly (non-Hodgkin’s lymphoma).
In contrast, reactive (benign) nodes occur far more commonly and often present following a sore throat (tonsillitis), another infection, such as EBV, acne or dental abscesses. They are sometimes painful. A soft lump presenting for the first time anterior to the sternomastoid muscle in a younger patient (20-30 years) may be a branchial cyst, but as a small percentage of these can harbour malignancy in their wall, urgent referral should be made. It is very unusual for longstanding lumps (histories of years not weeks) such as lipomas and skin pathology to be malignant, so these should be referred routinely.
Investigation
Many GPs will do initial blood tests including FBC, ESR, U&Es and EBV. These are likely to be normal, especially if there is no other relevant history to suggest infection. Both lymphoma and metastatic squamous cell carcinoma cannot be diagnosed on a blood test.
The most useful investigation following referral is head and neck ultrasound with fine needle aspiration cytology (FNAC) for nodes that look worrying. The nodal size is not a determinant in itself for malignancy but instead the morphology and ratio of the short to long axis guides the radiologist when deciding if FNAC is needed. For example, some reactive (benign) nodes following repeated tonsillitis can measure over 2cm in length but have a short axis of 7-8mm.
Diagnosis
If malignancy is confirmed on FNAC, appropriate further investigations including staging CT, examination and biopsy of the oropharynx under general anaesthetic and PET-CT may be required. Sometimes ultrasound-guided core biopsy or node excision is needed to confirm a diagnosis, particularly for lymphoma.
Management
- Neck lumps are common presentations in general practice and the majority are not malignant.
- A good history is important for helping to guide management – a lump present for many years is almost certainly not going to be malignant, while a painless enlarging lump with no other symptoms should be taken very seriously indeed.
- Blood tests are only useful in primary care when infection is thought to be the cause.
- Urgent referral to a neck lump clinic should be made for lumps persisting more than three weeks to exclude a malignant process. These clinics are usually run jointly with oral/maxillofacial surgery and ENT and have a radiologist and pathologist present to be able to provide a diagnosis in most cases on the day of the visit.
Professor Peter Brennan is a consultant maxillofacial/head and neck surgeon at the Portsmouth Hospitals NHS Trust
Mr Alex Goodson, Mr Karl Payne and Mr Arpan Tahim are specialty registrars in oral and maxillofacial surgery.
The authors have recently published a book entitled ’Important Oral and Maxillofacial Presentations for the Primary Care Practitioner’. It has been sent to every GP practice in the UK, free of charge, and contains algorithms providing guidance for the management of many head and neck conditions, including neck lumps and malignant disease. The book has been written in collaboration with the RCGP. Further copies are available at cost price (£12.50) from Amazon.
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.













