Ten top tips – shingles
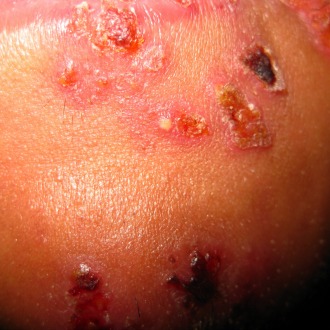
1. There should be risk assessment of household and other close contacts who are pregnant, less than one month old or severely immunosuppressed
Shingles (herpes zoster) represents local reactivation of varicella zoster virus (VZV), giving a unilateral vesicular dermatomal rash. Contact, by direct or droplet spread of vesicle fluid, may result in primary VZV infection (chicken pox) in those who have never before been infected with VZV and who are unvaccinated against VZV. Cases are considered infective until the rash has completely crusted over, so a risk assessment of household and other close contacts who are pregnant, less than one month old or severely immunosuppressed is imperative, as primary VZV infection could have severe consequences. Note, if the body site affected is covered by clothing, risk of transmission is low, but patients with shingles should still avoid contact with the immunosuppressed and pregnant until the rash has completed crusted over.
The incubation period for primary VZV disease is between one and three weeks in the immunocompetent, and between one and four weeks in the immunocompromised if they have received prophylactic zoster immunoglobulin.
2. Check the maternal VZV IgG level prior to giving human varicella zoster immunoglobulin (VZIG)
A pregnant woman exposed to shingles that has never previously been infected with VZV (i.e. gives no history of chicken pox) has a risk of acquiring chicken pox, which carries a risk to the unborn child and the health of the mother. There is a 10-day window post-exposure in which VZIG can be given to mitigate the risk and severity of VZV disease.1 Prior to this being given, the maternal VZV IgG level should be checked (serum serology). A positive VZV IG indicates immunity to VZV – there would be no risk of VZV disease, and VZIG would be unnecessary. Serology for VZV is only for the purpose of assessing immunity, not diagnosis of infection. VZIG has no benefit once VZV infection has occurred.
3. Shingles in a pregnant woman carries no risk to the unborn baby
The mother will already have protective IgG from past primary VZV infection, and so there is no risk to her baby. If shingles is confirmed, the woman should avoid contact with other pregnant women and neonates until the rash has completely crusted over, i.e. after about five to seven days. Where lesions are completely covered by clothes, the risk of transmission is low, though by convention she should still avoid these vulnerable groups until crusting has occurred.
4. Pain associated with shingles is neuropathic
As a result, it may respond to over-the-counter NSAIDs and paracetamol, but the mainstay of treatment is with neurotropics such as pregabalin and gabapentin.
5. Shingles that takes more than two weeks to heal should warrant investigation
Shingles which is recurrent, disseminated, covering several dermatomes or slow to heal (i.e. more than two weeks) should warrant investigation for immunodeficiency, including HIV infection.
6. Beware special or complicated cases
Ophthalmic involvement may cause permanent impairment of sight and therefore these patients should be referred. Systemic aciclovir should be given at the earliest opportunity – aciclovir eye drops should also be given, but are insufficient alone.
Facial shingles may rarely cause Bell’s palsy. Any neurological signs should warrant hospital admission for assessment and parenteral aciclovir. In the immunocompromised, shingles may rapidly lead to disseminated VZV disease, which carries high mortality and has possible complications of pneumonia, encephalitis, hepatitis and disseminated intravascular coagulopathy.2 Cases of shingles in the profoundly immunocompromised warrant immediate parenteral aciclovir and hospital admission. Valaciclovir may be given if immunosuppression is mild.
7. Shingles should be treated with oral valacicolovir, famiciclovir or aciclovir
Ideally, the regimen should be started within three days of the rash developing, in order to reduce symptom duration and reduce the risk of post-herpetic neuralgia. Famciclovir and valaciclovir are preferable because they achieve better blood levels than oral aciclovir and can be taken less frequently. Treatment is always indicated in the following groups:
- Those aged over 50 years old
- The immunocompromised
- Severe pain at presentation
- Lesions on the tip of the nose or eye i.e. Hutchinson’s sign, which indicates involvement of the nasocilliary branch of the ophthalmic division of the trigeminal nerve.
Standard antiviral treatment duration is five days for healthy individuals and seven to 10 days for immunocompromised individuals.
8. Bacterial super-infection of shingles may occur and is most commonly caused by Staphylococcus aureus
Oral flucloxacillin is a reasonable empirical therapy. Secondary spreading cellulitis as a result of super-infection should raise the possibility of Group A streptococcal infection. For cellulitis not warranting admission, co-amoxiclav, clindamycin or a combination of flucloxacillin and amoxicillin would cover both possibilities.
9. Live VZV vaccine is effective in preventing shingles3
The zoster vaccine is licensed in the UK and recommended for patients aged between 70-80 years old. Mild side effects, including fever and local erythema, are common, but severe side effects are rare. Should a shingles rash develop on a patient who recently received the vaccine, viral swab of the lesion should be sent to determine whether the disease is due to wild-type VZV or the vaccine strain itself.
This does not alter case management, but is requested by VZV reference services to monitor vaccine failure and adverse outcomes. New evidence shows that shingles is more common in those with rheumatoid arthritis, chronic obstructive pulmonary disease, inflammatory bowel disease, asthma, chronic kidney disease, type 1 diabetes and depression.4 Consideration should be given to vaccinating patients with these conditions to prevent shingles, provided there is no immunosuppressive state which would contradict it.
10. Shingles in patients under 40 years should warrant a review of vascular risk factors
There is growing evidence that shingles is associated with an increased risk of stroke, TIA and MI, particularly in patients less than 40 years old. Shingles in this population should warrant review of vascular risk factors.5
Professor Judith Breuer is a consultant virologist at Great Ormond Street Hospital
Dr Andrew Flatt is a specialist registrar in virology at Great Ormond Street Hospital
Competing interests: Dr Flatt has received sponsorship from GlaxoSmithKline for a poster presentation on a separate topic
References
- Department of Health. Immunisation against infectious diseases (The Green Book) – Varicella: Chapter 34. London; DOH: 2012
- Department of Health. Immunisation against infectious diseases (The Green Book) – Shingles: Chapter 28a. London; DOH: 2013
- Gagliardi AM, Gomes Silva BN, Torloni MR, Soares BG. Vaccines for preventing herpes zoster in older adults. Cochrane Database Syst Rev, 2012;(10):CD008858
4 Forbes HJ, Bhaskaran K, Thomas SL, Smeeth L, Clayton T, Langan SM. Qunatification of risk factors for herpes zoster: popukation based case-control study. BMJ, 2014;348:G2911.
5 Breuer J, Pacou M, Gauthier A, Brown MM. Herpes zoster as a risk factor for stroke and TIA Neurology, 2014;82(3):206–12
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









