Learning Objectives
To update you on
- Managing rheumatoid arthritis in practice
- Which blood tests to perfor
- What kind of monitoring might need to be done for patients on DMARDs
- Complications
- The role of steroids
Dr Louise Warburton is a GPSI in rheumatology, associate medical director of Shropshire Community NHS Trust and clinical lead for Telford MSK service
GPs see many patients with joint aches and pains. What are the key features to consider a diagnosis of rheumatoid arthritis (RA)?
This is the million-dollar question. The length of the history is important. If the patient has new symptoms of pain or joint swelling, that is significant. If they have been experiencing the same symptoms for years, it is unlikely to be new-onset inflammatory arthritis.
Which of the following are typically features of RA?
- Stiffness lasting for around 10 minutes
- Asymmetrical inflammation
- Early morning stiffness
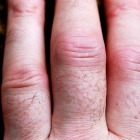
- Inflammation that starts in the small joints of the hands and feet?
This module reviews the symptoms and signs.
The NICE guideline for RA advises not to wait for the results of blood tests and X-ray before referring for a specialist opinion if the symptoms and signs are present.
What is the value of blood tests in these patients in primary care? How reliable is rheumatoid factor, and when should anti-CCP be considered?
GPs understand that patients with inflammatory arthritis require prompt referral but won’t want to swamp rheumatology departments unnecessarily. How can they recognise when to refer?
Then what treatments can be offered to relieve pain, but not obscure physical signs in patients awaiting their first appointment?
Which disease-modifying antirheumatic drug (DMARD) might be offered in secondary care – and when should steroids be used in RA?
This module also reviews the complications of RA that might be encountered in primary care.
Click here to read the full article and download your certificate logging 1.5 CPD hours towards revalidation
Not a Pulse Learning member? Click here to join and gain access to over 400 CPD modules
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens