GP beware – musculoskeletal
Case 1
An 83-year-old man presented with pain around the right groin over the previous four months. He was extremely fit, a keen tennis player but could no longer play due to the discomfort. He had had a right total hip replacement six years previously and had returned to all activities. The GP examined him and excluded a hernia and any other intra-abdominal pathology. Suspecting the hip, they organised an X-ray of the pelvis. The report suggested no abnormality. The diagnosis of a groin strain was made. Analgesia was prescribed and physiotherapy was started.
After six months, there was no improvement in the symptoms and tennis was still impossible. A referral to an orthopaedic surgeon was made. At that point, he walked with an antalgic gait. The hip had a good range of movement but rotation and ‘telescoping’ the affected leg reproduced the pain. The original X-rays were reviewed and showed subtle changes within the pelvis suggestive of osteolysis – bone destruction due to wear of the polyethylene hip socket. A CT was organised and this scan confirmed fairly extensive bone loss within the pelvis around the hip socket.
He underwent revision surgery, where the acetabular component was found to be loose, and polyethylene debris having caused extensive bone loss in the pelvis. This was reconstructed with a revision acetabular prosthesis and ceramic joint surfaces. He made a good post-operative recovery and has been able to return to tennis.
GP’s diagnosis
Groin strain
Actual diagnosis
Osteolysis
Clues
A patient presenting with new symptoms after an otherwise successful joint replacement.
Take home message
The important message here is that a patient who presents with new, worsening symptoms, related to a replaced joint, should be referred to a joint replacement specialist, even in the event of apparently normal radiological investigations.
Accelerated wear of modern implants in such a short timescale is unusual but can occur. The management, based on the information available to the GP, was entirely reasonable. However, radiographic appearances may be subtle and are not always picked up by the duty radiologist who, in fairness, may not appreciate the significance of the changes. Previous images may not be available (as in this case), which also makes it harder to interpret any radiographic changes.
In fact, many radiology departments will now include a statement at the end of their report suggesting an orthopaedic opinion, even if the imaging of a joint replacement appears normal.
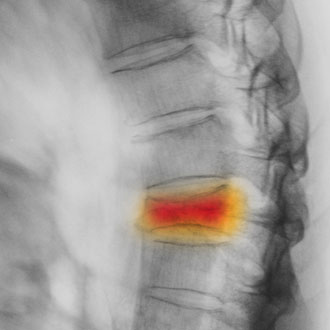
Case 2
Mr A is a 65-year-old gentleman who presents to his GP with lower thoracic back pain over the last five to six weeks. He has just returned from a long vacation in his caravan. He recalls a fall five weeks ago when he stumbled out of his caravan and landed on the step. It was quite an innocuous fall, as there are only two steps coming out of his caravan and he only fell gently on his back. He had some pain initially but this was not severe. However, the pain has not subsided.
Of note, he is known to have ankylosing spondylitis, but this has never caused him problems in the past. On examination, there was some tenderness over the thoracolumbar junction but there were no neurological deficits. His GP was not too worried, but given the history of a fall sent him for an X-ray of his thoracolumbar spine. This was reported as showing no visible fracture, and Mr A was reassured of this and sent for physiotherapy.
However, his pain continued and over the next two to three months the pain actually worsened, such that he was becoming steadily less mobile and became housebound. Mr A was referred to his local hospital and was assessed by the orthopaedic team. A CT scan of the thoracolumbar spine was ordered, which showed a T11 fracture across all three columns. This fracture was not visible on X-ray. Mr A was transferred to a specialist spinal hospital where he underwent percutaneous posterior pedicle stabilisation of the fracture. He made a full recovery.
GP’s diagnosis
Musculoskeletal back pain.
Actual diagnosis
Thoracic fracture.
Clues
Patient has ankylosing spondylitis with ongoing pain after fall.
Take home message
Any patient with ankylosing spondylitis, with an innocuous fall and ongoing pain, must have a CT scan to rule out a fracture as the fracture is not always visible on plain X-ray.
Case 3
Mrs P has had pain in her second toe for six months. This came on gradually and is made worse on activity and relieved by rest. She feels pain under the plantar aspect of her second metatarsophalangeal joint and into the toe. Her GP notices her second toe is elevated slightly off the ground when standing, and has deviated toward the great toe.
The GP diagnoses a Morton’s neuroma and performs a steroid injection in the first-second web space. The pain eases, but the deformity worsens, with persistent elevation and deviation of the second toe now causing rubbing on shoes and pain on the top of the toe.
GP’s diagnosis
Morton’s neuroma
Actual diagnosis
Second metatarsophalangeal joint (MTPJ) synovitis with torn plantar plate following steroid injection.
Clues
Morton’s neuroma is rare in the first-second interspace (most common is three-four, then two-three interspaces). Morton’s neuroma does not cause a toe deformity, whereas second MTPJ synovitis can as it progresses – classically elevation and medial deviation. This produces the ‘peace sign’, where a V-shaped gap between the second and third toes develops from medial deviation of the second toe, like two fingers making the peace sign.
Tenderness on the top of the joint differentiates synovitis from Morton’s neuroma, where tenderness occurs on the plantar aspect of the foot, in between the MTPJs. Steroid injections around the joint with an already weakened plantar plate (due to synovitis), may cause a plantar plate rupture and make the deformity worse. Therefore, judicious use of steroids is advised and used for a confirmed diagnosis.
Take home message
Think of second metatarsophalangeal joint synovitis in the differential with Morton’s neuroma. Obtain an ultrasound if unsure – in synovitis, this may show increased vascularity around the synovium (joint lining), tears in the plantar plate (later stages of the problem) or a Morton’s neuroma. Avoid ‘blind’ steroid injections unless you are sure of both the diagnosis and the anatomy.
Mr Tim Waters is a consultant orthopaedic surgeon at Spire Bushey Hospital and West Herts Hospitals NHS Trust.
Mr Robert Lee is a consultant spinal surgeon at Spire Bushey Hospital and Royal National Orthopaedic Hospital, Stanmore.
Mr David Gordon is a consultant foot & ankle surgeon at Spire Bushey Hospital and Luton and Dunstable University Hospital
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.











