Orthopaedic clinic – osteomyelitis
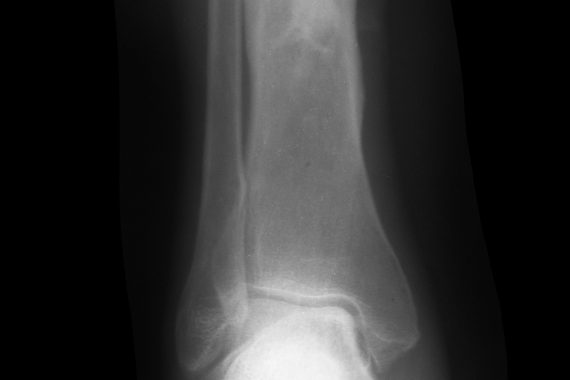
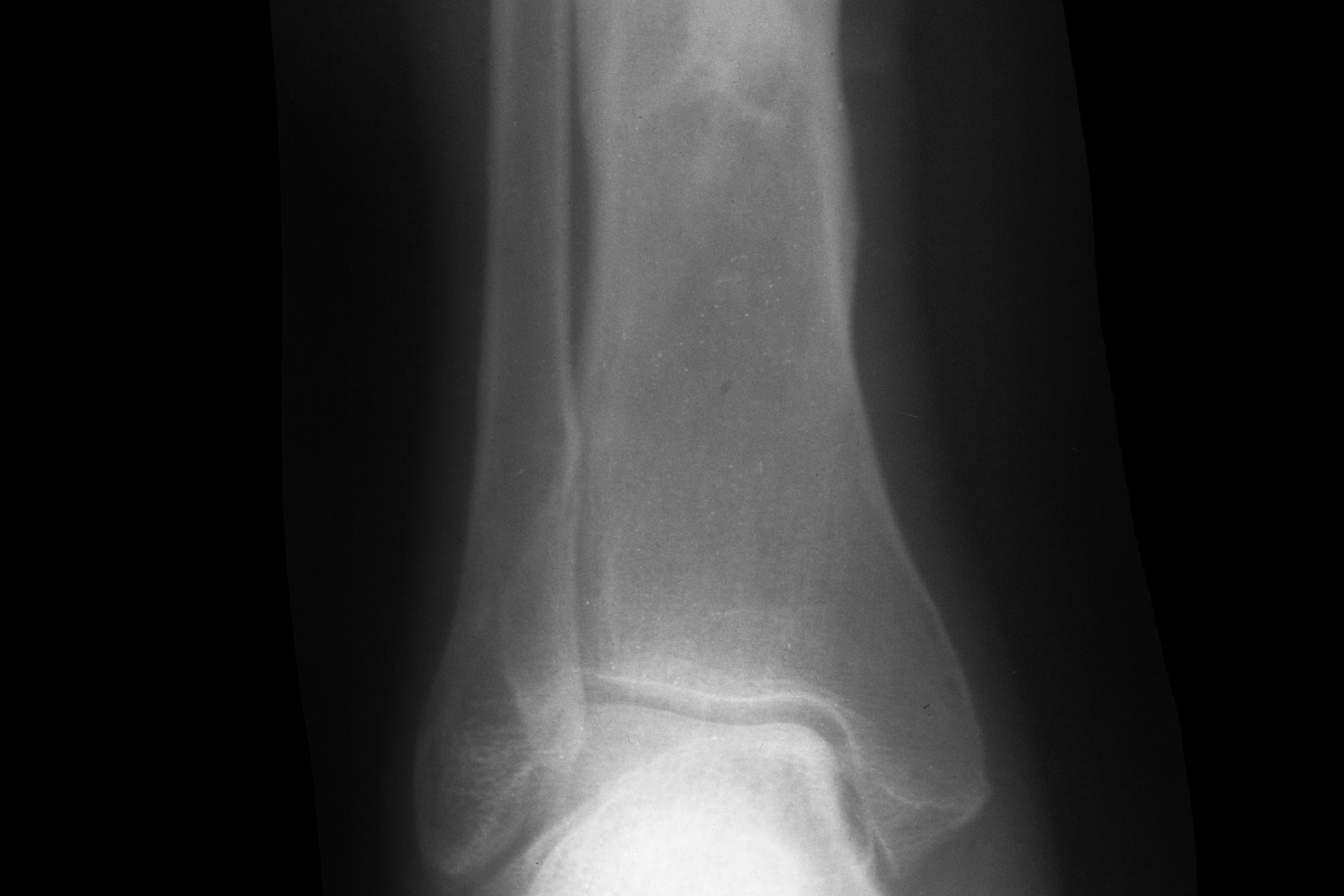
A 65-year-old lady presents to her GP with intermittent pain and discharge from a sinus on the proximal anterior border of her shin. A detailed history reveals that she has had problems on and off since the age of six, when she had treatment in Kenya (where she was temporarily domiciled) for an infection in the bone. She had had a total of 14 operations on the leg in total and many courses of antibiotics, and had been told there was nothing that could be done short of an amputation to stop the infection coming back.
On examination, she is afebrile and has a 10x10mm sinus on the anterior border of the shin in the proximal third. There is extensive scarring tethering the skin to the bone but no significant inflammation or induration of the soft tissues. There is no pain on weight-bearing but there is tenderness on percussion of the tibia (as you would percuss the chest). Foot pulses and sensation are normal. Blood tests reveal minimally-raised white cell count, ESR and CRP. A plain X-ray of the tibia reveals chronic remodelling deformity with evidence of a cavity in the bone.
The problem
Osteomyelitis can generally be regarded as acute or chronic, depending on the absence or presence of dead bone. If left untreated, acute haematogenous osteomyelitis will progress to chronic osteomyelitis by a well-recognised mechanism. Organisms can also enter the bone via penetrating injuries, open fractures, contigious spread from adjacent soft tissue ulcers, or iatrogenically during any orthopaedic procedure. When organisms multiply in the bone they incite an inflammatory response that would normally cause swelling, but inside the closed cavity of the bone this causes an increase in pressure. Once this pressure rises above capillary perfusion pressure, blood ceases to flow and bone death ensues. It also means antibiotics will not be delivered to the area, even if given intravenously. The local inflammatory response causes lysis of the surrounding living bone and frequently the dead bit of bone separates to form a sequestrum lying in a fluid-filled cavity. As time goes by the surrounding bone becomes sclerotic, walling off the cavity and, in doing so, making it practically impenetrable by the body’s defences. From time to time, however, the organisms continue to multiply and force their way out, creating a channel, known as a cloaca, to the outside world. As they do so, the periosteum is often lifted by the pressure, leading to a florid calcified periosteal reaction or involucrum, and eventually making it to the skin surface through a sinus. Once the pus under pressure has discharged, the pain, swelling and systemic symptoms often resolve, but if the sequestrum is not removed the stage is set for the whole cycle to begin again.
Features
There is often history of cycles of pain, particularly at night, as well as swelling and redness with fevers and rigors until the pus comes to a head and discharges, leading to a resolution of symptoms only to recur every few weeks or months. But presentation can be much more subtle, with infection sometimes lying dormant in a cavity for many, many years.
Diagnosis
History and examination usually give the diagnosis away. Be sure to ask about previous travel history, antibiotics, allergies and surgical interventions. Keep a special lookout for new soft tissue growths around chronic sinuses, as sarcomatous change (known as Marjolin’s ulcer) can occur, necessitating urgent referral. Blood tests such as FBC, ESR and CRP can be useful but may be normal during a quiet phase. Plain X-rays should be ordered first and MRI scans are the most useful for surgical planning. Nuclear bone scans are generally unhelpful and reserved for the localisation of active areas in complex cases.
Management
Management is generally surgical. Antibiotics may help the soft tissues to settle quicker during a flare, but unless the source is dealt with then they will not affect a cure. Once referred to her local specialist bone infection unit, she will be seen by a multidisciplinary team including orthopaedic, plastic surgery and infectious disease specialists. The principles of surgery include:
- Laying open or debridement
- Sending multiple deep samples for microbiology and histology
- Complete removal of all dead or non-viable bone (sometimes requiring segmental excision and external fixation)
- Filling any dead spaces with a dissolving antibiotic carrier
- Primary closure with the use of local or free flap transfer as required
- Prolonged intravenous (up to six weeks) or oral antibiotics according to cultures and sensitivities.
With the above measures, 95% of patients will remain symptom-free for five years or more, and most will never require further surgery. Amputation rate is as little as 1%. Clinicians should no longer be continuing the misguided impression that amputation is the only option for long-term disease control.
Mr David Stubbs is a consultant orthopaedic and limb reconstruction surgeon at Oxford University Hospitals NHS Foundation Trust.
References
1 McNally M, Nagarajah K. (iv) Osteomyelitis. Mini Symposium: Pathology. Orthopaedics and Trauma, 2010;24:6:416-429
2 Ferguson JY, Dudareva M, Riley ND, et al. The use of a biodegradable antibiotic-loaded calcium sulphate carrier containing tobramycin for the treatment of chronic osteomyelitis: a series of 195 cases. Bone Joint J, 2014;96-B:829-36
3 Sheehy SH, Atkins BA, Bejon P, et al. The microbiology of chronic osteomyelitis: prevalence of resistance to common empirical anti-microbial regimens. J Infect, 2010;60:338-43
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









