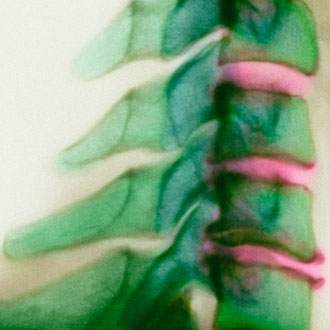
1. Radiographic cervical spondylosis is common but does not correlate with neck pain
There is a very poor relationship between the severity of cervical spondylosis and symptoms, and only a small percentage of patients with radiographic evidence of cervical spondylosis are symptomatic.
MRI is the investigation of choice for nerve root entrapment or spinal cord injury. Where neck pain is the primary complaint and cervical spondylosis the suspected diagnosis, imaging is seldom helpful. In one study of asymptomatic individuals over 70 years of age, 95% of men and 70% of women had radiographic evidence of cervical spondylosis.1
Plain radiographs of the neck may be useful in excluding boney lesions such as malignancy or Pagets, where systemic symptoms are present.
An MRI scan is the investigation of choice where signs of radiculopathy are present, such as myotomal weakness, persistent dermatomal sensory loss, or where cord compression is suspected.
2. Symptomatic cervical spondylosis can cause neck, shoulder, intrascapular and chest pain
The most common symptoms of cervical spondylosis are neck pain and stiffness with no neurological involvement. Pain from the lower cervical structures may radiate to the shoulders, intrascapular region or rarely the chest wall.
The pain associated with mechanical musculoskeletal derangement is typically dull, deep, and aching.
Cervical spondylosis may also present with headaches, as referred pain from the upper cervical structures may be perceived in the distribution of the of the trigeminal nerve and C1-3 dermatomes.
Clinical findings are limited to restricted movements and tenderness of the cervical spine.
3. Nerve root entrapment in cervical spondylosis can present with shoulder/arm pain, paraesthesia or weakness.
In cervical spondylosis radiculopathy usually occurs due to a combination of boney impingement due to osteophytes at the uncovertebral joints and degenerative disc bulge.
The most commonly involved nerve roots are the sixth and seventh nerve roots, which are caused by C5-C6 or C6-C7 spondylosis. Patients usually present with neck or arm pain, paraesthesia or weakness in the upper limb or a combination of these symptoms.
4. Cervical spondylosis is a recognised – but rare – cause of dysphagia and airway dysfunction.
Cervical spondylosis is a rare cause of dysphagia or airway dysfunction. Primary oesophageal pathology should be ruled out before attributing dysphagia to spondylosis. Dysphagia occurs when large anterior osteophytes cause mechanical compression of the oesophagus.
A plain radiograph demonstrating large anterior osteophytosis would support the diagnosis.
Conservative therapy with anti-inflammatory medications and PPIs may help in mild-to-moderate cases of dysphagia. Surgery is reserved for more severe cases.
6. Postural, sleep and simple range of movement exercises are reasonable first-line treatment options
First-line treatment for patients with cervical spondylosis with no neurological involvement is usually given as advice on posture, sleep position and range of movement exercises for the neck.2
The Arthritis Research UK information sheet can be downloaded to provide a simple guide to neck exercises and posture.
I would recommend, where possible, sleeping on the side or back with a pillow which allows the neck to be in a neutral position (no flexion or rotation). The use of a cervical soft collar for sleep may promote a neutral neck position but is often poorly tolerated by patients. Neck collars should not be used long term without specialist advice.
7. Physiotherapy can offer a wide range of options for patients with cervical spondylosis
Physiotherapy incorporates a number of different modalities including manual therapy, neck strengthening exercises, laser therapy, acupuncture, interferential, traction, hot/cold therapies and massage.
Although patients report symptomatic relief during massage, a systematic review of massage for neck pain showed little data to support its use as an individual treatment.
A recent Cochrane review suggested a modest short-term benefit with manipulation.
In patients with neuropathic pain, physiotherapy is a good first-line referral combined with neuropathic medication. A good physio will know when to be active or passive so as not to exacerbate nerve compression.
8. Medical management should start with paracetamol. Neuropathic pain may respond to low dose amitriptyline.
Medical management for cervical spondylosis presenting with no radicular signs should start with paracetamol initially on a prn basis titrated to a regular 1g tds to qds depending on bodyweight and comorbidities.
Compound analgesic agents including low dose codeine may be considered but the risk of dependence and side effects needs to be balanced against analgesic benefit.
NSAIDs offer reasonable analgesia and have been recently approved by NICE for use in other forms of osteoarthritis, but side effects limit their long-term use.
Where radicular pain is present – dysaesthesia with evidence of dermatomal or myotomal involvement – low dose tricyclic agents such as amitriptyline or nortriptyline can be useful.
Tramadol, gabapentin and pregabalin are also useful in the management of neuropathic pain but their use may be limited by their side effect profile.
9. Identifying the source of pain is key to choosing the right treatment
Acute episodes of pain often improve without intervention, but if it doesn’t settle after the conservative approaches already mentioned, then intervention may be required.
Interventional treatment for cervical spondylosis is dependent on the source of pain. Clinical examination offers little to pinpoint the specific location or source of pain in spondylosis.
Possible sources of pain include the zygapophyseal joints, the disc and nerve root entrapment.
Most radiculopathy pain responds to conservative treatment – decompression surgery is indicated for refractory pain and persistent or progressive neurological deficits.
10. Cervical spondylotic myelopathy accounts for the most common cause of atraumatic spinal cord injury in elderly patients.
Cervical spondylosis in the majority of patients is a relatively benign condition but is the most common cause of non-traumatic spinal cord injury in the elderly.
Cervical spondylotic myelopathy occurs as narrowing of the spinal canal. Progression of myelopathy may be slow or may occur in a stepwise fashion.
Early signs of spondylotic myelopathy include gait disturbance (spastic gait) and numbness and clumsiness of the upper limb.
Autonomic symptoms generally occur late and include increased urinary urgency, frequency and incontinence.
The clinical findings in spondylopathic myelopathy include mixed upper and lower motor neurone findings in the upper limb depending on the level of injury, with:
- a positive Hoffmans’ reflex – a hyper reflexive response suggestive of an upper motor neurone lesion elicited by flicking the terminal phalanx of the middle or ring finger. A positive response is seen with flexion of the terminal phalanx of the thumb
- a positive Babinski test and
- an ataxic gait in the lower limb.
Acute myelopathy may also occur where individuals with pre-existing cervical spondylosis and a narrow canal sustain an acute cervical hyperextension (commonly a blow on the forehead).
An MRI scan is the investigation of choice, usually followed by surgical decompression.
Dr Richard Smith is a consultant rheumatologist at Salisbury District Hospital
Professor Les Barnsley is an associate professor of rheumatology at Concord Hospital, New South Wales, Australia
Simple Tasks is a national awareness campaign to help people understand the negative impact of diagnosing and treating rheumatic conditions, outside what is recognised as the ‘window of opportunity’ – the first 12 weeks after onset of symptoms.
References
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens