Obscure diagnosis – postural tachycardia syndrome
Recognising disorders of the autonomic nervous system is a challenge for GPs. Symptoms can be subtle, non-specific and mimic other conditions (1). Yet dysautonomia can be a source of considerable disability and poor quality of life for patients. The postural tachycardia syndrome is no exception (2).
Definition
Postural tachycardia syndrome (PoTS) is an abnormal response by the autonomic nervous system to upright posture. The normal vasoconstrictive response to standing that ensures venous return from limbs and splanchnic blood vessels to the heart is inadequate in PoTS, resulting in venous pooling, compensatory tachycardia and noradrenaline release, and altered cerebral circulation. Patients develop symptoms of orthostatic intolerance – symptoms that develop in an upright position and are relieved by lying down.
PoTS is a heterogeneous group of disorders sharing similar characteristics, but probably has a variety of causes. To be diagnosed with PoTS, patients must experience a persistent increase in heart rate that starts within 10 minutes of standing or head up tilt table test. This increase should be 30bpm or more (40bpm in teenagers), or to over 120bpm and must be associated with symptoms of PoTS (3). Although by definition, blood pressure does not drop in PoTS, some patients subsequently develop a vasovagal response with drop in blood pressure or heart rate (4).
Prevalence/epidemiology
The prevalence is unknown, but has been estimated at approximately one in 600 of the general population. Recognition seems to be increasing and tertiary referral centres with an interest in this condition are now flooded with referrals and have waiting times of over a year for the first appointment, and a further year for tests. A rough poll at two recent Pulse Live conferences revealed that approximately one in 10 GPs had heard of PoTS, so recognition and referrals have the potential to increase further.
PoTS is four times more common in women and often affects those between the ages of 15 and 50 (5).
Other names
PoTS was named and defined in 1993, but experts consider it to be the same phenomenon as Da Costa Syndrome, which affected soldiers during the American Civil War, and The Soldier’s Heart as described in the BMJ by Sir James Mackenzie during the First World War. Both physicians noted its existence in their civilian patients and further studies suggested it was actually more common in women and ran in families.
Clinical features
GPs should consider PoTS in patients who present with a multitude of apparently inexplicable symptoms. The most common ones reported are light-headedness, palpitations and fatigue (6).
Symptoms can include (7):
- Light-headedness.
- Syncope.
- Fast palpitations.
- Chest discomfort.
- Breathlessness.
- Mental clouding.
- Headache.
- Fatigue.
- Nausea.
- Gastrointestinal upset (often diagnosed as irritable bowel syndrome).
- Tremulousness.
- Blurred vision.
- Poor sleep.
- Exercise intolerance.
Many symptoms improve rapidly with decumbency, but fatigue, gastrointestinal upset and ‘brain fog’ can persist for some hours after episodes, and these more chronic symptoms can make the postural trigger more difficult to identify.
Routine tasks such as bathing and dressing can exacerbate symptoms and disability has been shown to be equivalent to congestive heart failure.5 While some patients experience only a few symptoms, others experience most of them every time they attempt to stand, resulting in wheelchair dependency or confinement to bed.
On examination, patients may exhibit no abnormality when sitting or lying flat.
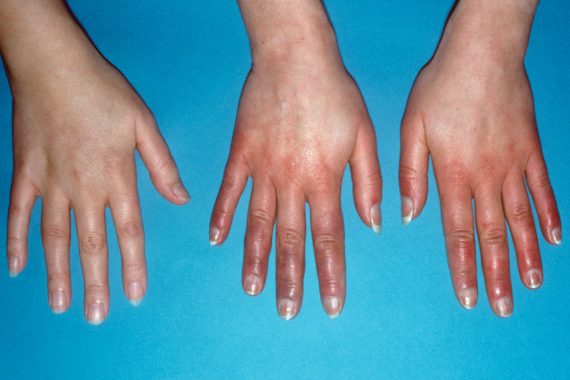
On standing, in addition to a tachycardia, 50% of PoTS patients develop dependent acrocyanosis, a dark blue-red discolouration of lower legs, feet and hands (5).
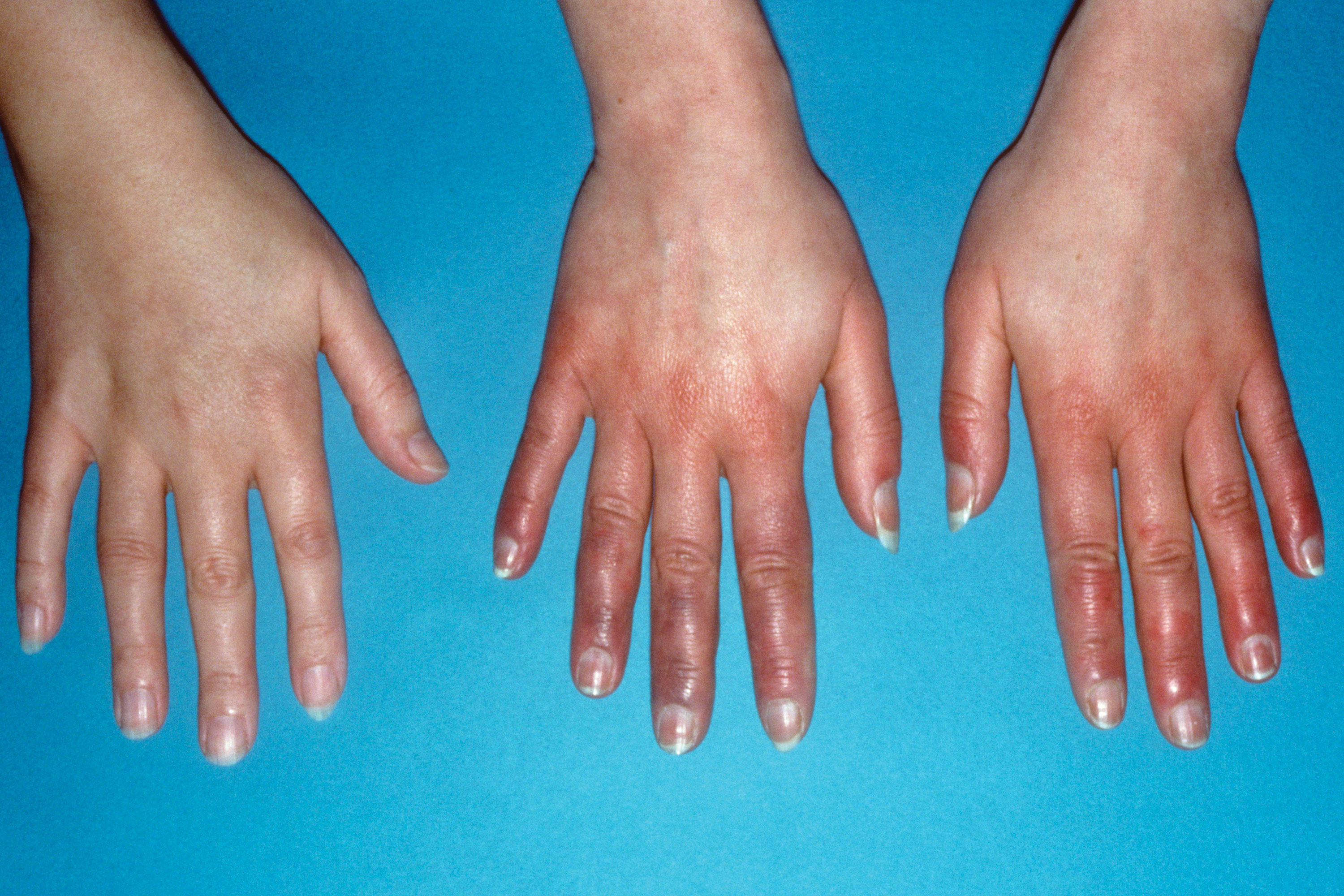
Acrocyanosis of the hands
Differential diagnosis
Conditions with similar symptoms should be excluded. These include anaemia, thyrotoxicosis, Addison’s disease, orthostatic hypotension and phaeochromocytoma.
Misdiagnosis of PoTS is common and the mean time to correct diagnosis in the UK is seven years (6). This may be due in part to the large number of non-specific symptoms and few clinical signs. In fact, the most common medically unexplained symptoms as described by the Royal College of Psychiatrists are remarkably similar to symptoms of PoTS.
Patients often receive incorrect psychiatric diagnoses from both primary and secondary care physicians, including anxiety, panic disorder and depression. As noradrenaline levels are often elevated in the upright position in PoTS, it is unsurprising that anxiety assessment tools reliant upon measuring physical symptoms of anxiety would reveal high scores in PoTS, but when a psychologically based tool is used (the Anxiety Sensitivity Index), in PoTS there is a tendency toward less anxiety than in the general population (5).
In patients who present with anxiety and symptoms suggestive of a hyperadrenergic state, it can be helpful to ask if they occur only after rising from bed or are exacerbated by standing in queues to help clarify a postural link.
Up to one-third of patients with chronic fatigue syndrome have been found to have PoTS, although the association is not clear (8). Current NICE CFS/ME guidelines do not include an active stand test as part of the assessment process, but there are those who would recommend this as part of the investigations.
How can GPs diagnose PoTS?
If GPs suspect PoTS, they can perform an active stand test. This involves resting the patient flat on an examination couch until settled and recording blood pressure and heart rate. In a safe environment, preferably against a wall and with no sharp corners nearby, the patient then stands up and further recordings are made initially, and then at two-minute intervals for 10 minutes. The test can be stopped if the patient experiences severe symptoms or syncope occurs.
The patient should be monitored continuously throughout the test.
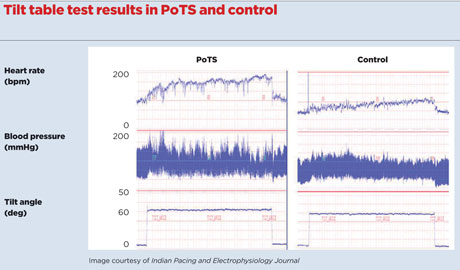
Tilt table test results
Although the active stand test is sometimes called the ‘poor man’s tilt test’, it has fewer false-positive results than a tilt table test and some specialist centres are using the tilt test less to diagnose PoTS, except when it is useful to exclude other conditions such as cardioinhibitory vasovagal syncope and autonomic failure.
Associated conditions
Insufficient research has been conducted to say with certainty what causes PoTS. However, there is clearly an association with the joint hypermobility syndrome, also known as Ehlers-Danlos hypermobility type, and Sjögren’s syndrome (9).
Specialist centres that manage Hughes syndrome and mitochondrial disease are increasingly noting PoTS in their patients and more research is needed in this area.
There have also been individual case reports of PoTS associated with a number of conditions, including multiple sclerosis, Lyme disease, mast cell activation (when flushing is prominent), inappropriate sinus tachycardia syndrome, diabetes, and also following viral illness, pregnancy and immunisation.
Treatment
Patients with PoTS usually have a relative hypovolaemia in that the capacity of their blood vessels is greater than the blood volume. Drinking two to three litres of fluid each day, or until urine is pale straw coloured (in children), is recommended.
From clinician experience, a high salt diet and compression garments (class II) are often advised, although there is no clear evidence yet to support this advice.
While many patients become unwell with PoTS when undertaking regular aerobic exercise, once afflicted by this condition, patients can feel unwell for days after minimal effort and exercise avoidance and deconditioning can ensue. A carefully graded exercise programme has been shown to improve postural tachycardia and quality of life. Horizontal exercise such as Pilates, swimming, recumbent exercise biking and rowing are recommended.
If lifestyle changes do not control symptoms, medication may be required. Examples include fludrocortisone, desmopressin, midodrine, ivabradine, a ß-blocker and pyridostigmine (5).
Referral
If PoTS is suspected, referral should be made to someone with an interest in this condition. Such physicians are usually found in syncope clinics and they will usually see PoTS patients, even though only a third actually show syncope. Cardiologists with an interest in arrhythmias, and some neurologists and medicine for the elderly consultants, have expertise in this area.
There is a list of clinicians with an interest in PoTS on the PoTS UK and STARS websites.
Ideally, patients with PoTS should be managed by a multidisciplinary team. Although this approach has been considered successful in the US, no such NHS service currently exists in the UK.
‘Dustbin’ rating
The diagnostic criteria are based on consensus. The precise underlying mechanism and associated diseases remain unclear, and there have been no large trials to evaluate best management. Nevertheless, much has also been learned about PoTS.
Radioactive labelling of albumen has revealed that patients with PoTS have a relative reduction in their blood volume of around 13%.
Plasma renin and aldosterone activity would be expected to be high in hypovolaemia to promote sodium and water retention, but in fact standing levels are paradoxically low and the reason for this is not clear (5).
This relative hypovolaemia may relate to autonomic peripheral denervation (10), which has been demonstrated in patients, reducing their ability to maintain vascular resistance with increased gravitational stress (9).
There has been work to try to identify the mechanism underlying ‘brain fog’, one of the most distressing symptoms of PoTS. One study demonstrated that patients with PoTS experience increasing neurocognitive impairment as they became more upright, compared with controls who were unaffected by position (11).
Cerebral autonomic dysregulation has been noted in PoTS with increasing upright tilt, which may help to account for this problem.
Some patients have high standing serum levels of noradrenaline, especially in the ‘hyperadrenergic’ form of PoTS, when there is also a hypertensive response to standing (5).
Antibodies to adrenergic receptors were found in two groups of PoTS patients, but few controls, suggesting possible autoimmune aetiology (12).
Misdiagnosis – when to think of PoTS
- Medically unexplained symptoms – especially the triad of palpitations, dizziness and fatigue
- Chronic fatigue syndrome
- Anxiety or panic disorder
- Recurrent vasovagal syncope
Piecing together this jigsaw of clues to understand the mechanism (or more likely, variety of mechanisms) that cause PoTS remains a challenge.
Diagnosing PoTS is not easy and requires a high index of suspicion. However, getting it right is immensely satisfying, as research shows patients are often misdiagnosed and receive psychiatric labels over many years. It is an ‘invisible illness’, and patients often look well despite significant disability and are unable to claim benefits, despite losing their jobs or education. The gratitude is palpable when patients finally receive a diagnosis that makes sense to them, and once it is identified, many patients will improve with appropriate treatment.
Dr Lesley Kavi is a GP in Birmingham and a trustee of the charity PoTS UK
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.











