How to consult remotely: contraception
Continuing our series, Dr Carrie St John Wright advises how to optimise remote consultations for contraception
The way we start and review contraception has transformed in the Covid-19 pandemic. Having adapted to remote consultations through necessity, we are now finding patients appreciate the ease and efficiency of remote contraception checks. New digital tools that allow fast access to information have given us more confidence to prescribe contraception remotely, while the use of self-administered contraception injections in particular can free up clinic time. Here are my tips for using remote consultations to start and review contraception safely and effectively.
Is a remote consultation suitable?1
Begin with this checklist:
- Ask the patient if they are in a private space where they can’t be overheard.
- If they indicate they are not alone, ask if they feel comfortable to talk about personal medical information – are they with a trusted person or support worker?
- Ascertain if the patient might be vulnerable – are they under 16, or is there any recorded prior abuse?
- Be alert to any risk of coercion.
- If in doubt, arrange a face-to-face consultation.
- Check the patient is in the UK. Some indemnifiers do not cover GP consultations if the patient is overseas.
Also establish that the person has enough understanding and capacity to make decisions for themselves. It may be preferable to have the conversation in person, with a support or independent medical capacity advocate. If so, record and check this person’s identity separately.
Starting a combined oral contraceptive (COC) pill
The usual precautions should be taken before initiating the COC. Take a full medical history to exclude venous thromboembolism (VTE), high blood pressure (BP) and other factors in the Faculty of Reproductive and Sexual Healthcare (FRSH) UK Medical Eligibility Criteria for Contraceptive Use (UK MEC).2 Ensure the patient has no prior history of migraine with aura, and document this.
It may be necessary to remotely record weight, body mass index (BMI) and BP for safe prescribing. Patients can self-report these observations with home measurements, or with readings taken in pharmacies or GP practice waiting rooms.
COC prescribing is safest if the BMI is under 34kg/m2; above 35kg/m2 there is increased risk
of VTE.2
The benefits outweigh the risks of treatment at BP measurements up to 140/90mmHg. Above this,
it may not be safe to prescribe, especially if readings are over 160/100mmHg. Remote readings may be worth checking with a calibrated BP monitor.
Key history
- Smoking Age over 35 and smoking more than 15 cigarettes a day is an unacceptable risk to start the COC. Discuss risks and benefits if the patient is over 35 and has stopped smoking in the past year.
- Recent illness In particular, take note of myocarditis due to Covid-19 or as a side-effect of Covid-19 vaccination.2 Note any new or recent diagnoses not yet coded in notes – for example,
a new breast cancer or personal history of VTE (both absolute contraindications for the COC). Family history may also be relevant, as are recent immobility and surgery. - Recent childbirth Current advice is to wait six weeks from birth before starting the COC if breastfeeding, and at least three weeks if not, unless there is a VTE risk, in which case a discussion of risk-balance is required.
- Recent termination of pregnancy There is no recommended time frame for initiation of contraception post termination, and quick starting may be appropriate to reduce the risk of further unwanted pregnancy.
- Medication history COCs can interact with medications, such as lamotrigine.3 Screen for new medications and also recent emergency hormonal contraceptive (EHC) use – with some EHCs, for example ulipristal acetate (UPA), quick starting may reduce the effectiveness of both. Also ask about drugs used off label to enhance concentration, such as modafinil; these are often purchased online, and can reduce COC efficacy.
There is no longer a need to check BP after three months of the COC, according to FSRH guidance,4 so a full year’s script can be issued, provided the patient knows to return with any issues. Although this may result in some medication wastage, overall costs and resource use are reduced by cutting unnecessary follow-up appointments.
It may, however, be appropriate to provide a limited supply – for example, three months – in patients who would benefit from an early follow-up, such as those with significant medical conditions.
Repeat prescribing of COC
If the patient has been on the COC for some time and is happy to continue, it’s still important to have a consultation at each repeat prescription to check nothing has altered in their history. New medications and illnesses or family history should be checked, especially migraine with aura. An up-to-date BP and weight (or BMI, if needed) as well as smoking status should be recorded yearly.
Starting a progesterone-only pill (POP)
There are fewer risks associated with the POP. The main things to rule out before initiation are:
- Current or past breast cancer diagnosis – current is contraindicated, past requires a risk-balance discussion.
- Multiple risk factors for cardiovascular disease, current ischaemic heart disease or a liver tumour – all require risk-balance discussion, but are not totally contraindicated.
Checking medication use is important to flag any enzyme inducers, which affect POP efficacy. Patients wishing to start POP after stopping enzyme-inducing drugs should be advised to use condoms until 28 days after the last dose of the enzyme-inducing drug. Otherwise patients can start POP on days one to five of their menstrual cycle with no extra precautions, but if starting after day five they should use condoms for 48 hours. Quick starting requires a pregnancy test no less than three weeks after the most recent unprotected sexual intercourse (UPSI). Patients can start taking POP straight after EHC with levonorgestrel (LNG) but must wait five days after taking UPA.
Potential side-effects of the POP include an altered bleeding pattern, especially in the first three months. The POP can be prescribed for 12 months at first, with advice to return if there is unwanted bleeding or there are any other issues.
Self-administered contraceptive injections
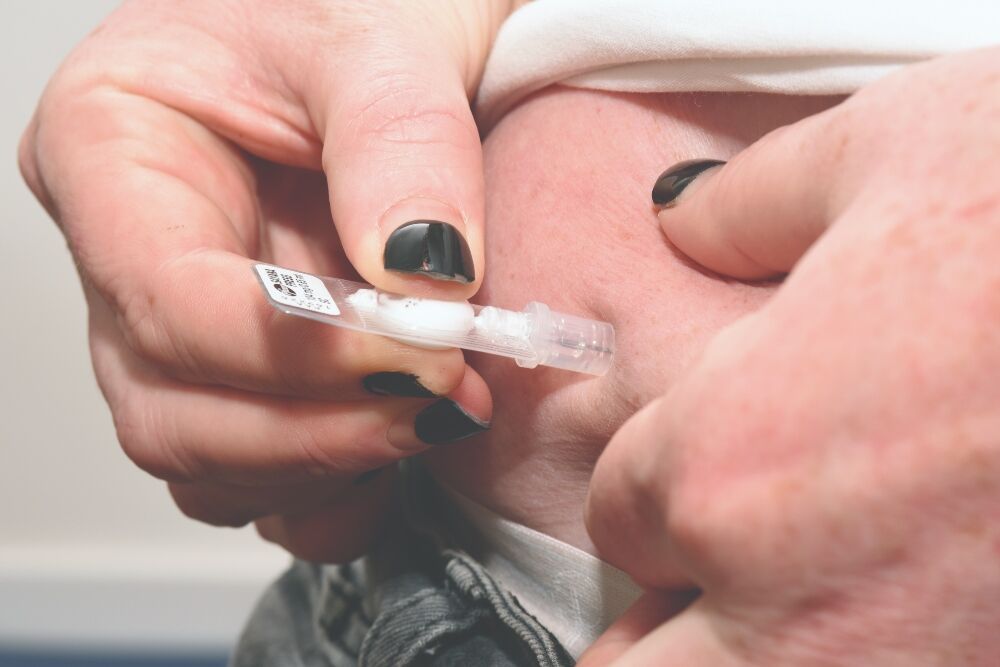
Sayana Press 13-week subcutaneous (SC) injection5 has become more widely used since the pandemic as patients do not have to come into practices to get their next dose. As with intramuscular (IM) depot medroxyprogesterone acetate (DMPA), the SC DMPA injection is highly effective, but takes seven days to become effective if starting after day five (see box below).
Sayana Press comes in a prefilled injector and should be vigorously shaken, then administered into the anterior thigh or abdomen, avoiding bony areas and the umbilicus. A video available online can be used to remotely teach patients.5 A competent adult should be present for the first and second doses in case of an allergic reaction.
Explain that self-administration may cause an injection site reaction (reported in 9% of patients in one study).6 Women should also be informed that return of periods can be slow, and return to fertility can take up to a year after discontinuation of either IM or SC DMPA.6 The FSRH suggests a review every two years to reconsider the risk versus benefit for bone mineral density, particularly for those under 18 and over 40. Other side-effects include amenorrhoea and reduced or erratic unscheduled bleeding. You can prescribe three months of COC (if the patient is eligible) or mefenamic acid for troublesome unscheduled bleeding.
Weight gain can be a problem with DMPA; if more than 5% of body weight is gained in the first six months of use, patients are likely to experience continued weight gain. Acne, decreased libido, mood swings, headache, hot flushes and vaginitis have also been reported with DMPA.
Initiation of self-administered SC DMPA
How to start
- Starting on day one to five – no additional precautions required
- If starting after day five – condoms required for seven days
- Quick starting – requires pregnancy test three weeks from last UPSI. Note amenorrhoea from depot injection may mask pregnancy; intermenstrual bleeding may be mistaken for a period
- Can quick start after EHC if other oral methods are not acceptable (immediately after LNG, five days after UPA)
Dosing and drug interactions
- There is a 13-week interval between doses for SC administration
- Can be given up to one week late without additional precautions
- No increased risk of pregnancy has been demonstrated in DMPA injectable users with higher body weight, although data are limited in women with a BMI ≥40kg/m2
- The efficacy of DMPA is not reduced with concurrent use of enzyme-inducing drugs
Dr Carrie St John Wright is a GP and appraiser in Bristol, and member of the Faculty of Sexual and Reproductive Healthcare
References
- Patel R and Munro M. Standards for online and remote providers of sexual and reproductive health services. Sex Transmit Infect 2019;95:475-476. Link
- FRSH. UK Medical Eligibility Criteria for Contraceptive Use (UK MEC) 2016. Link
- FSRH CEU guidance. Drug interactions with hormonal contraception 2017. Link
- FSRH. Guideline – Combined hormonal contraception. BMJ Sex Reprod Health 2019;45: Supplement 1. Link
- Inject Sayana Press. 2022. Link
- FSRH. Clinical Guideline: Progesterone-only injectable. 2020. Link
Further resources
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.
Related Articles
READERS' COMMENTS [2]
Please note, only GPs are permitted to add comments to articles














Very comprehensive and helpful for these times.
Nice summary. Ultimately, this single entity is chronic waste of GP and nurse resources.