Clinical casebook: sports injuries in general practice (2 CPD hours)
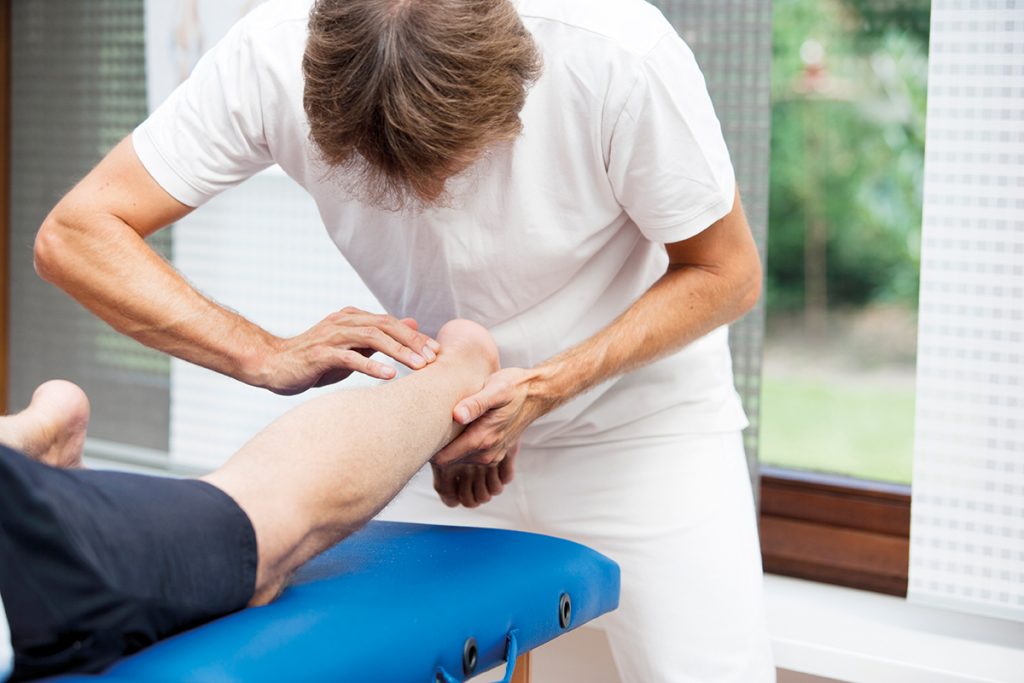
Sports medicine consultant Dr Neil Heron and colleagues Dr Emma Gilmartin and Dr Dáire Rooney advise on the assessment and management of key sports injuries encountered in primary care
Case 1
A 33-year-old semi-professional football player limps into your practice on a Monday morning following a match the day before. This was his first game after a lengthy lay-off due to the Covid-19 pandemic. He explains he jumped to head a ball and experienced an intense pain on the back of his leg, as if he had been kicked. He has been unable to walk without pain since. He thinks he has sprained a ligament and asks you to examine his injured leg.
How do Achilles tendon (AT) ruptures present in general practice?
The AT is one of the most commonly injured tendons, yet 20% of cases are missed by non-specialists.1,2
Rupture of the AT usually follows rapid plantarflexion with the affected limb’s knee extended. Alternatively, it may occur after forceful ankle dorsiflexion of a plantarflexed foot. This is often associated with pushing off from a standing start or jumping, making it a common injury in sports such as football, tennis and athletics. The patient may describe this as if they were kicked in the back of the leg, but when they turned around, no one was there. This may be accompanied by an audible snap.
Nevertheless, almost one-third of patients presenting with this injury do not practise intensive physical activity.3 The initial injury may be followed by residual calf pain and weakness when the patient is ‘pushing off’. The injury is also common in the inactive elderly patient with a less forceful mechanism of injury.4
What risk factors are associated with AT ruptures?
Participation in sport is the main risk factor: 75% of all AT ruptures occur during sport.5 AT ruptures are five times more likely in males and follow a bimodal age distribution, with peaks in those aged between 30-50 and over 60.6,7 In the elderly, quinolone antibiotic use has been shown to increase the risk of AT rupture, especially with concomitant steroid therapy.8 Prior Achilles tendinopathy, for example in those with inflammatory arthritis, also increases the risk of AT ruptures.9
How should I examine a patient with suspected ruptured AT?
The patient should be positioned prone, with their legs hanging over the examination couch. Bruising and swelling may be seen around the AT, but not always. The clinician should then use Simmond’s triad of tests (see Figure 1, left) to assess the likelihood of AT rupture.
The following increase the probability of the diagnosis:
- Injured foot lies in a more dorsiflexed position.
- AT is tender to palpate; may be a palpable gap over the posterior calf or in the AT midportion.
- Loss of plantarflexion when the calf is squeezed (although plantarflexion can still occur if, for example, there is an intact plantaris tendon on the medial aspect of the AT).
Plantarflexion may be weakened in the affected limb, when asking the patient to stand on their toes. However, even in a complete AT rupture, movement may be unaffected because of preservation of secondary muscles of plantarflexion.
How should the GP manage AT ruptures?
The most important initial action is an urgent, same-day referral to orthopaedics for diagnostic imaging (dynamic ultrasound) and treatment planning, often currently accessed through A&E departments. Any delay in treatment leads to poorer outcomes, although prognosis is good with prompt treatment. Studies have shown that patients return to normal walking and stair climbing at a median of 12 weeks and may return to sport between six to nine months.11
Not a Pulse Learning member? Click here to join and gain access to more than 400 CPD modules
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.










