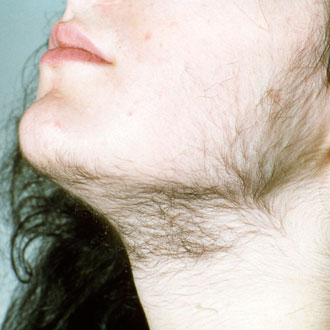
1. Hirsutism is different from hypertrichosis
Hirsutism is the presence of excess hair growth in women as a result of increased androgen production or increased skin sensitivity to androgens, or both, which leads to terminal hair is that is longer, stiff and pigmented, as in scalp hair. It should be distinguished from hypertrichosis, which is androgen independent and causes uniform growth of non-terminal vellus) hair over the body, which is short, soft and lightly pigmented, similar to hair seen on the faces of children.
Hirsutism is associated with male hair pattern temporal balding, full beard distribution and hair over the shoulders, chest, and upper abdomen. The female hair pattern lacks temporal balding and terminal facial hair, other than on the upper lip and chin. It is unusual for women to have terminal hair on the shoulders and chest, other than a few periareolar hairs, and it is uncommon for women to have terminal hair on the upper abdomen. Virilisation is the development of a male hair pattern, increased pectoral musculature, huskiness/deepening of the voice, changes in libido and clitoromegaly. Androgen-mediated hirsutism is rarely, if ever, associated with a normal menstrual pattern.
2. The most common cause of hirsutism is polycystic ovary syndrome (PCOS)
The most common causes of hirsutism are PCOS, idiopathic (no other clinical or biochemical abnormalities) hyperandrogenism with a normal menstrual cycle, non-classic adrenal hyperplasia, medications and, rarely, androgen-secreting tumours. Hirsutism has an ethnic component and is more common in women from the Mediterranean and Indian subcontinent. For a diagnosis of PCOS, other causes of clinical or biochemical hyperandrogenism and menstrual cycle disturbance (hyperprolactinaemia, thyroid dysfunction, Cushing’s syndrome if clinically suspected) need to be excluded. Two of the following three criteria must be fulfilled for a diagnosis of PCOS, as per the Rotterdam Consensus criteria:
a) A clinical diagnosis of oligomenorrhoea or amenorrhoea—menstrual cycles longer than 35 days or fewer than 10 periods per year
b) Clinical (hirsutism, acne, or androgen alopecia) or biochemical (raised free androgen index) evidence of hyperandrogenism
c) Polycystic ovaries on ultrasound examination
Not all patients need an ultrasound scan of the ovaries. Only patients with either menstrual disturbances or clinical or biochemical evidence of hyperandrogenism alone should have transvaginal ultrasonographic imaging of the ovaries to look for polycystic ovaries.
3. History, especially menstrual history, and physical examination looking for virilisation/masculinisation are important in the evaluation of hirsutism
The important elements of the history include the age of menarche and the subsequent menstrual history. The age of onset of hirsutism, and the rate of progression as well as severity, should be determined. The benign forms of hirsutism tend to begin in the pubertal years and then remain stable. Hirsutism that appears clearly before puberty or later after puberty may be caused by medication, such as phenytoin or cyclosporine, or rarely by an ovarian or adrenal neoplasm. Ethnicity should be taken into account as mild hirsutism in Asian women may indicate excess androgen production. It is important to understand the impact of hirsutism on the patient and their expectations of treatment, as these may have profound effects psychologically on self-image.
4. Psychological issues should be considered in all women with PCOS
Depression or anxiety should be screened for and, if present, assessed. Women with PCOS are at an increased risk of psychological and behavioural disorders as well as reduced quality of life (QoL). It has been shown that PCOS has a significant detrimental effect on QoL compared with controls, and weight issues were most likely to affect QoL in women with PCOS. Women with PCOS are at higher risk of developing significant psychological difficulties compared with healthy and other controls, and may also be at risk of eating disorders, sexual and relationship dysfunction. Psychological issues, especially depression, should be screened according to the NICE guidelines.
5. Free androgen index is the first line in biochemical investigation for the evaluation of hirsutism
Measurement of total testosterone, even using modern immunoassays and tandem mass spectrometry, has a low sensitivity for measuring hyperandrogenemia. High (for example, with the use of oral contraceptive pills) or low (for example, in insulin resistance or obesity) concentrations of sex hormone-binding globulin (SHBG) may affect total testosterone values. Measurement of SHBG enables calculation of the free androgen index (total testosterone concentration divided by SHBG concentration, multiplied by 100). In practice, total testosterone is often normal in PCOS, but the free androgen index, which is a measure of bioavailable testosterone, is raised because SHBG is suppressed by increased insulin resistance.
6. Total testosterone concentration more than 1.5-2 times the upper limit of normal, or a history of rapid hirsutism, are likely to be associated with tumour associated hyperandrogenism
A high total testosterone concentration or increased hirsutism within a short (12 month) timeframe may indicate that the hyperandrogenaemia could be caused by an ovarian or adrenal tumour and should trigger referral to secondary care for evaluation.
7. Weight loss and lifestyle advice are very important in the effective treatment of patients with hirsutism linked to obesity
Lifestyle modification for weight loss and increasing physical activity are critical in the treatment of hirsutism in obese patients. Weight loss alone may reduce hirsutism, but also enhances the effect of any medical intervention. Metformin has shown to improve menstrual irregularity in women with PCOS, but usually has a minimal effect on reducing hirsutism.
8. Cosmetic and topical treatments, including bleaching, shaving, depilatory creams, or waxing, are the mainstay of treatment for all forms of hirsutism
Cosmetic treatment such as bleaching, shaving, depilatory creams or waxing are cheap, effective and safe. It is the treatment that will bridge the patient over the period that is required for most medical treatments for hirsutism to achieve a clinical effect. In patients with androgen-mediated hirsutism, no matter how the androgen effect is interrupted, at least one complete hair cycle is required to replace terminal hairs with a new non-medullated hair (around 6 months) before improvement can be appreciated. It should also be noted that the hirsutism will often return on the cessation of medical treatment.
Eflornithine (α-difluoromethylornithine) is a topical agent which can be applied to the face and that can be useful in hirsutism. However, the clinical effects of eflornithine require 8–12 weeks to reach maximum effect, and physical measures are the best bridge for that time.
Electrolysis passes an electrical current to destroy the hair follicle. It can be effective but in view of the time and cost it should be reserved for discrete areas and can be associated with scarring.
Laser treatment, or photoepilation, destroys the hair follicle but is most effective in pigmented hair and less so in blonde unpigmented hair. Care needs to be taken in patients with pigmented skin, and it is an expensive modality that needs multiple sessions for it to be effective.
9. Oral contraceptive pills containing at least 30μg of ethinyl estradiol and 1mg of a synthetic progestin are effective in hirsutism
In addition to lowering plasma testosterone by suppressing gonadotropin effects on the ovary, the estrogen component of the oral contraceptive is an effective stimulus for the synthesis and secretion of SHBG. Because ovarian testosterone secretion in women is not regulated by hypothalamic and pituitary feedback, free testosterone will fall in the early phases of increased SHBG secretion, which is an additional benefit of oral contraceptive therapy.
10. Antiandrogens, including spironolactone, are effective in treating hirsutism due to hyperandrogenism
Antiandrogens are as effective as oral contraceptives for the treatment of hirsutism, but may have an additional benefit in some patients. Often these are treatments reserved for secondary care. Because of the danger of antiandrogen-induced abnormalities of foetal genital development, antiandrogen treatment should only be given to women who are using adequate contraception before and during this therapy. There is a lack of high-quality clinical trials to support combination therapy for hirsutism, although these are prescribed for some patients in greatest need.
Finally, the popular combination of oral contraceptive pills with or without the addition of shaving, eflornithine, or antiandrogens should not be thought of as a substitute for weight loss with patients who have obesity-related insulin resistance, where that weight loss will enhance the response to medical treatment.
Dr Thozhukat Sathyapalan is Reader at Hull York Medical School, Department of academic diabetes, endocrinology and metabolism, and honorary consultant endocrinologist at Hull and East Yorkshire Hospitals NHS Trust
Professor Stephen L Atkin is professor of medicine at Weill Cornell Medical College in Qatar, and was previously an honorary consultant at the department of diabetes and endocrinology at Hull and East Yorkshire Hospitals NHS Trust
Further reading
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens