The information – menopausal flushes
The patient’s unmet needs (PUNs)
A 54-year-old lady attends to discuss her ongoing hormone replacement therapy (HRT) prescription – an oestrogen with a cyclical progestogen. She has been on this treatment for five years, having started it after nine months of amenorrhoea for distressing flushes. ‘I know there are risks, so I keep trying off it,’ she explains, ‘But each time my flushes come back with a vengeance. How serious are the side effects really? Can you prescribe anything else, or are the herbal remedies in the pharmacist any good? And how long do I have to put up with these flushes, anyway?’
The doctor’s educational needs (DENs)
How long do menopausal flushes usually last? When prescribing HRT, how long should the treatment be tried before an attempt is made to stop?
Menopausal flushes and sweats are a common consequence of menopausal oestrogen deficiency, and are thought to affect around 80% of menopausal women. While oestrogen deficiency is the underlying cause, many other factors such as lifestyle, diet, life stresses, access to support, expectations, and perceptions interact to affect their severity, impact and duration. It was previously believed that the average duration of vasomotor symptoms was two to three years, but more recent data suggests that around 50% of women experience these symptoms for seven years, with 42% of women aged 60 to 65 still experiencing symptoms.1
Replacing oestrogen in the form of HRT is still the most effective treatment for menopausal vasomotor symptoms, with a Cochrane review showing a clear beneficial effect with oestrogen replacement compared to placebo.2
Since there is no reliable way of predicting how long symptoms will last, there should be no arbitrary limits placed on the duration of use of HRT. It is reasonable for women to consider a trial without HRT at a time of their choosing. Since the benefits of HRT are thought to outweigh the risks for the majority of symptomatic women under the age of 60, and for many after age 60, there would not appear to be any reason to rush to stop before age 60.
Is recurrence inevitable when women try to stop HRT? Does stopping gradually make any difference?
It is impossible to predict if symptoms will recur on stopping HRT. While stopping HRT from a low dose rather than a high dose is likely to reduce the risk of symptom recurrence, limited evidence has shown that tailing off therapy is unnecessary. If symptoms do persist, the benefits of continued use of HRT usually outweigh the risks.3
What are the main risks of HRT, and how can they be conveyed to the patient in a balanced and accurate way?
HRT is often not initiated or stopped early because of concern among both women and healthcare professionals about the risks involved. The significant media attention around the publication of Women’s Health Initiative trial and Million Women study in 2002 and 2003 respectively has undoubtedly led to a loss of confidence, and significantly reduced use of HRT. After much reanalysis, the current overall view is that HRT prescribed before the age of 60 has a favourable risk-benefit profile.
Summary of risks
| Breast cancer | Possible increased risk with combined HRT if used for more than five years after the age of 50, around three to four extra cases per 1,000 women over five years. Little, if any, effect of oestrogen only. Combined HRT likely a promoter rather than initiator. Different progestogens may have different effects. Association with greater increased risks for two or more units of alcohol per day, and for postmenopausal obesity. |
|---|---|
|
Endometrial cancer |
Increased risk with unopposed oestrogen. Largely avoided by the addition of progestogen. Use of sequential HRT for more than five years may confer small increased risk. Continuous combined protective. |
|
Ovarian cancer |
Either small or no increased risk, possible one extra per 1,000 women over five years. No evidence of causality. |
|
VTE |
Two to four-fold increased risk with oral HRT, greatest risk in first year of use. Risk affected by type of progestogen. No apparent increased risk with transdermal oestrogen. |
|
Cardiovascular |
Increased risk only seen in women starting oral HRT after age of 60. Likely reduced risk when starting below age 60 – ‘window of opportunity’ |
Conveying the magnitude of the risks to women and helping them balance out the benefits for symptom control, as well as bone and heart health against the risks for them can be very difficult. The charts as shown can be helpful, and are available on the Menopause Matters website.
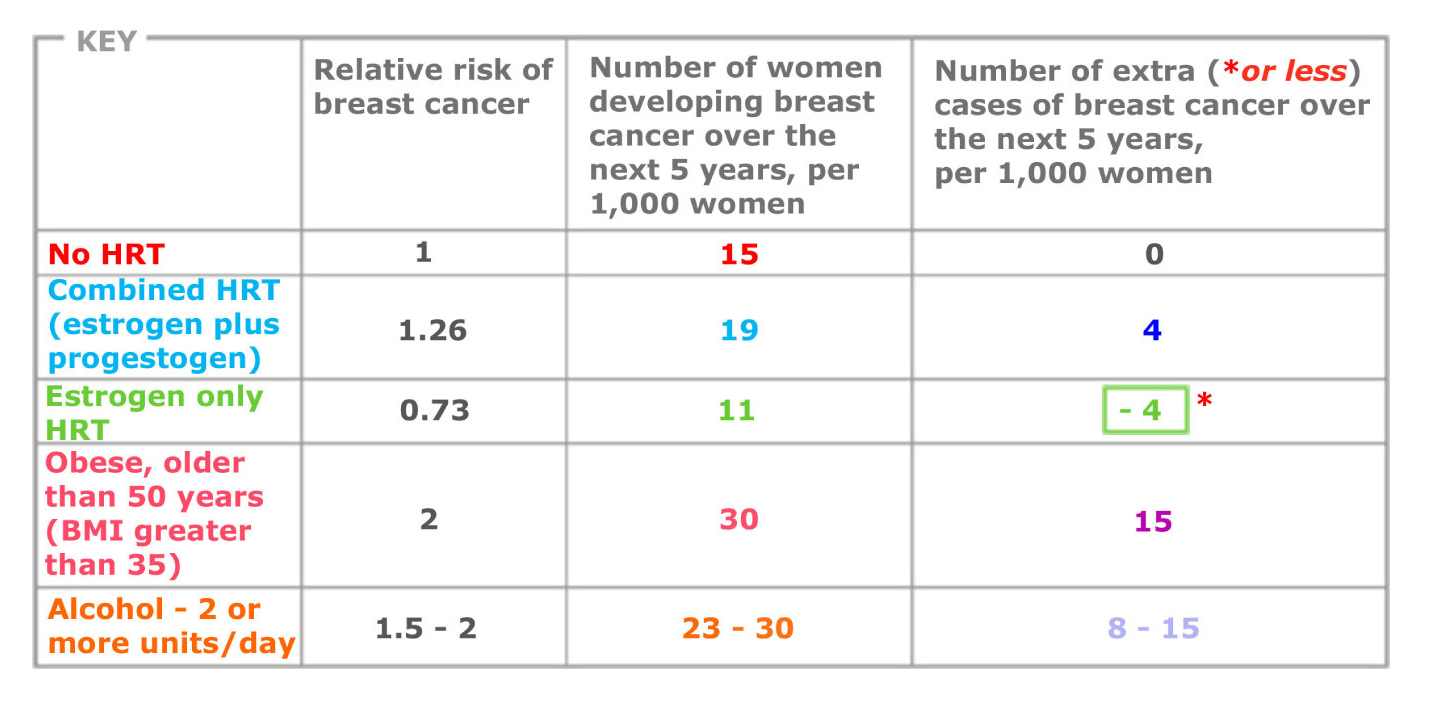
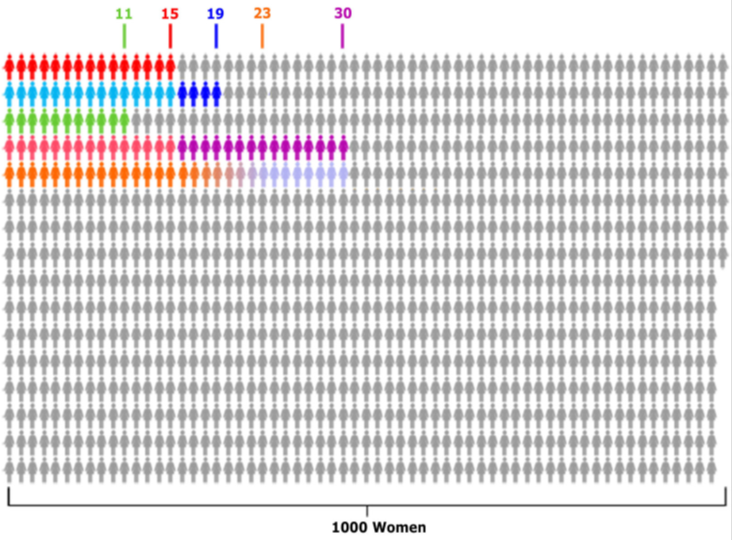
Figures from Women’s Health Initiative trial for women aged 50-79 years
What other prescribed treatments should be considered – and how effective are they?
For women who do not wish to, or are advised not to take HRT, non-hormonal therapies can be prescribed for vasomotor symptoms. Clonidine is the only non-hormonal preparation currently licensed in the UK for this indication, and modest benefit has been shown. Off-license preparations, which have been shown to provide more benefit than placebo, but are less effective than HRT and should only be considered if HRT is contraindicated include SSRIs such as fluoxetine and paroxetine, the SNRI venlafaxine, and gabapentin.4 Fluoxetine and paroxetine should be avoided in women taking tamoxifen because of a possible interaction and subsequent reduced effect of tamoxifen.
How effective – and safe – are ‘herbal’ remedies? Can any be recommended?
A recent survey has shown that 76% of women choose alternative therapies before considering use of HRT, despite the fact that many admitted to not knowing enough to make an informed choice. Alternatives were used due to a fear of the risks involved with HRT, the treatments being perceived to be more natural, desperation, and recommendations from friends.5 Evidence from placebo-controlled trials is limited and results are variable, with a Cochrane review showing no significant benefit.6
Key points
- All women become menopausal
- Women now live more than 30% of their lives in post reproductive, oestrogen-deficient years
- Most women experience oestrogen deficiency symptoms
- For many, symptoms can significantly affect quality of life, and persist for many years
- Management and treatment should be individualised
- For most women under the age of 60 with symptoms or risk for osteoporosis, and for many beyond age 60, HRT provides more benefits than risks
References
1 Hot flashes, night sweats may linger well into a woman’s sixties. Menopause 2015
2 MacLennan AH, Broadbent JL, Lester S et al. Oral oestrogen and combined oestrogen/progestogen therapy versus placebo for hot flushes. Cochrane Database Syst Rev, 2004;4:CD002978
3 Panay N, Hamoda H, Arya R et al. The 2013 British Menopause Society & Women’s Health Concern recommendations on hormone replacement therapy. Menopause International.
4 Sassarini J, Lumsden MA. Hot flushes: are there effective alternatives to estrogen? Menopause International, 2010;16:81-88
5 Cumming G, Currie H, Morris E et al. The need to do better – Are we still letting our patients down and at what cost? Post Reproductive Health, 2015
6 Cochrane review on alternatives
Further resources
The 2013 British Menopause Society & Women’s Health Concern recommendations on hormone replacement therapy. Panay N, Hamoda H, Arya R et al. Menopause International.
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.










