GPs to receive direct-access diagnostics test results within four weeks
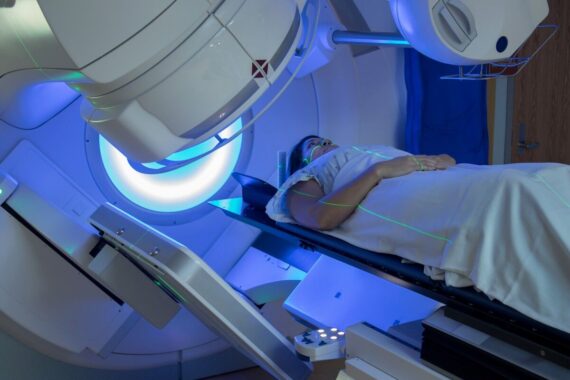
Direct access diagnostic tests requested by GPs should be completed in under four weeks, NHS England has stipulated in new guidance.
GPs can currently access urgent tests such as ultrasounds, X-ray, CT and MRI via hospitals or community diagnostic centres (CDCs).
The guidance, published last week, supports GPs in the ‘first phase’ of the direct access tests rollout which launched in November last year.
This phase sought to increase the use of certain tests when patients have ‘concerning symptoms’ but do not meet the NICE guideline (NG12) for urgent suspected cancer referral.
NHS England has now clarified that these referrals from GPs ‘will aim to be completed, including report, in no more than four weeks’.
The guidance said: ‘This will be achieved through work to increase capacity and enhance digital connectivity across the NHS, to enable results to flow more seamlessly.’
Alongside the guidance, NHSE has recommended the use of iRefer, a clinical decision support tool, which can help GPs choose the right test.
Providers will receive funding, ‘up to 2024/25’, in order to implement the iRefer system and make licences available to primary care.
The guidance added: ‘We will also provide support to ensure that all GP order communications systems are compatible with iRefer-CDS.
‘This aims to ensure best practice in GP referrals for imaging tests, so that patients receive the most appropriate tests and diagnostic capacity is managed.
‘GPs can continue to use existing direct access workflow, but our expectation is that practices with compatible order communications systems will migrate to iRefer-CDS as soon as licences become available.’
NHS England also emphasised the importance of escalation pathways and appropriate safety netting processes at GP practices to ensure that any results ‘indicative of a malignancy’ are referred via an urgent suspected cancer pathway.
Summary of urgent referral pathways and the eligible populations for each
Urgent referral pathway Eligibility Site-specific suspected urgent cancer referral High-risk, with specific symptoms and meet thresholds set out in NICE referral for suspected cancer guidelines (NG12) for referral to specialist or urgent GP direct access to tests Non-specific symptoms referral High-risk, with non-specific symptoms that could indicate more than one type of cancer/do not align with only one urgent cancer referral pathway Urgent GP direct access referral (this guidance) Low-risk, with specific symptoms but do not meet the thresholds set out in NG12, or GP-assessed higher risk not included in NG12
According to the guidance, phase two of the rollout will begin later this year and will aim to ‘support systems to make a wider range of direct access tests available’, such as spirometry and fractional exhaled nitric oxide (FeNO).
Last month, the Government announced the launch of 13 new CDCs in England, eight of which will be led by the private sector.
And health secretary Steve Barclay later confirmed that he is considering plans for patients to bypass the GP and directly access some diagnostic tests for suspected cancer themselves.
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.
Related Articles
READERS' COMMENTS [6]
Please note, only GPs are permitted to add comments to articles












I still miss the days when you’d dip your finger in a patient’s urine and taste for sugar.
Indeed I recall the days 😉 .
Wiser heads would dip the middle finger in the urine and taste the index finger.
In truth one of my early experiences in a long term psychiatric hospital as a holiday nursing auxillary was lining up the urines in test tubes, adding Benedict’s solution and heating over a bunsen burner. “Sister this one’s gone orange”
Yes Dr Munro, we’ll be back there soon enough. Then followed by TV charity ads and concerts raising money to help our failing health service.
‘This will be achieved through work to increase capacity and enhance digital connectivity across the NHS, to enable results to flow more seamlessly.’
Ahh yes. Adding “digital” makes everything better. Digital connectivity for results? How the hell do they think results are sent currently? Carrier pigeon?
By switching to “puters” I’m sure they could do 1.8 extra scans per day.
‘This will be achieved through work to increase capacity and enhance digital connectivity across the NHS, to enable results to flow more seamlessly.’
This sentence is all that is wrong with the NHS. What does this actually mean. ?
It means you’ll receive the same result in your investigations inbox, PDF, email, fax and paper. Seamless