Flagship NHS diabetes scheme under scrutiny
It was all meant to be Zumba dancing and cookery classes, but health chiefs are being urged to rethink the flagship national diabetes prevention programme to increase the numbers taking part.
The NHS England ‘Healthier You’ pilot schemes were announced in 2015 and rolled out last year. They were designed to encourage GP practices to refer at-risk patients to lifestyle programmes, paving the way for a national rollout of the scheme.
GP success
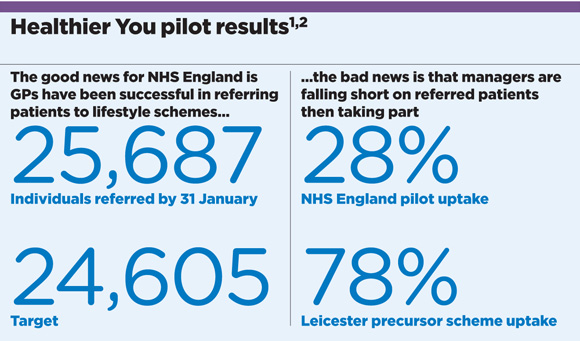
NHS England claims that, one year after rollout, the pilots are meeting targets for the number of patients referred to the programmes. And official figures presented at the Diabetes UK annual conference last month reveal that by the end of January, GPs had referred 25,687 at-risk individuals to the programme, against a target of 24,605.
However, the number actually taking part in the programme is far lower, with only 7,232 of 20,000 places filled. An evaluation of one of the precursor schemes, published by the National Institutes of Health Research, also casts doubt on the way the pilots are set up.1
The study looked at a prevention programme that, as with the national pilots, involved GPs identifying patients with raised glucose levels but not overt diabetes, and referring them to locally run diet and exercise classes.
We haven’t thought through how to retain people who are referred
Professor Kamlesh Khunti
The evaluation found that, after three years, there was no difference in incidence of diabetes between people who had originally been referred and those who hadn’t.
However, when the researchers did a sub-analysis of the 29% of people who stuck with the initial programme and also attended the complete course, including follow-up refresher sessions, they found a highly significant 88% reduction in the incidence of diabetes.
Co-investigator Professor Kamlesh Khunti, professor of primary care at the University of Leicester and a member of the steering committee of the NHS Diabetes Prevention Programme, told Pulse: ‘The lesson here for the national programme is, we haven’t thought through how we retain people who attend the programme.’
So far only 28% of those referred by GPs subsequently attend the pilot schemes, compared with a fill rate of 78% in the Leicester scheme.
Professor Khunti added: ‘There isn’t much happening in terms of engagement and getting people through, and this is an area of intense research – how can we keep people going on the programme? A lot of this is keeping them engaged through regular feedback, regular texting that sort of thing.’
Tailored programmes
Professor Khunti explained: ‘We may need to tailor our programmes – for example, not everyone wants to come to face-to-face sessions, but once they have been to one face-to-face meeting, maybe they can get online programmes.’
NHS England has recognised this need to tailor programmes. It is testing an online approach – under the tag ‘digital DPP’ – in 11 areas, which will be offered to people who previously declined to attend an initial consultation.
The national scheme is in the process of rollout to a further 20 sites across England (see box, left) but it has emerged that one – Gloucestershire – has yet to find a provider for the lifestyle programme.
NHS England said in a bulletin that ‘the contract for Gloucestershire will be re-tendered once the outcome for other Year 2 sites is known – allowing the possibility of the establishment of economies of scale by providers – following the receipt of no bids’.
NHS England national clinical director for diabetes and obesity Professor Jonathan Valabhji said: ‘The Healthier You NHS Diabetes Prevention Programme is based on the best evidence from RCTs and pragmatic trials carried out in real-world settings, and our intervention is significantly more intense than that delivered in the Leicester trial.
‘What the Leicester trial did show is the importance of duration of patient participation, which is precisely why providers of our new Healthier You programme are paid on that basis.’
GP practices to be given part of £44m funding to hire diabetes GPSIs and nurses
GP practices will be asked to spend more ‘dedicated time’ with patients with type 2 diabetes, under a major NHS programme to improve care of the condition, Pulse revealed last month.
Pulse has learned that NHS England is soon to launch schemes to increase the number of GPSIs working in diabetes management and provide funding to enable practices to hire more specialist nurses, via a £44m funding pot designed to improve treatment and outcomes for people with diabetes.
NHS England’s associate clinical director for diabetes Dr Partha Kar, a consultant in diabetes and endocrinology, told Pulse the funding is likely to see practices offer ‘more dedicated GP time’ to their patients. The funding plans, which are currently being rubber stamped by NHS England, are aimed at getting more practices to meet NICE-recommended goals on care for people with type 2 diabetes, as well as reducing variations in diabetes care across CCGs.
Dr Kar said the drive was to improve care for ‘existing patients that practices don’t have the staff to look after’.
He would not be drawn on how much of the £44m will go into general practice, but told Pulse: ‘What we’re trying to avoid is CCGs turning round and saying “we are just going to give it to hospitals”.’
NHS England chief executive Simon Stevens said last year that the NHS would be ‘upping its game’ on diabetes.
What is the Healthier You programme?
Under the national programme run by NHS England and Public Health England, GPs are being encouraged to target people with non-diabetic dysglycaemia who are at high risk of developing diabetes and refer them to intensive lifestyle programmes, involving group activities like cookery and Zumba classes.
The scheme launched last year at seven pilot – or ‘demonstrator’ – sites and was rolled out to a further 20 sites this year, with a view to getting 20,000 at-risk people starting the programme in 2016/17. Further expansion is planned to reach 100,000 people a year by 2020.
The programme has come under criticism from some GP experts for exaggerating the potential benefits of intensive lifestyle intervention in ‘real world’ patients, who they say may be less able or motivated to take up exercise or modify their diet than trial participants.
Evidence to date has suggested the impact has been limited, with uptake of the programme disappointing in demonstrator sites. However, some have highlighted the positive influence of GPs; uptake has been as high as 60% in places where GPs have been highly proactive in encouraging participation.
healthier you figs 580px
References
1 Davies MJ et al. A community-based primary prevention programme for type 2 diabetes mellitus integrating identification and lifestyle intervention for prevention Programme Grants Appl Res: 2017;5;2
2 Official figures presented at Diabetes UK conference 2017
Pulse July survey
Take our July 2025 survey to potentially win £1.000 worth of tokens

Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.










