Are you a diagnostic genius?
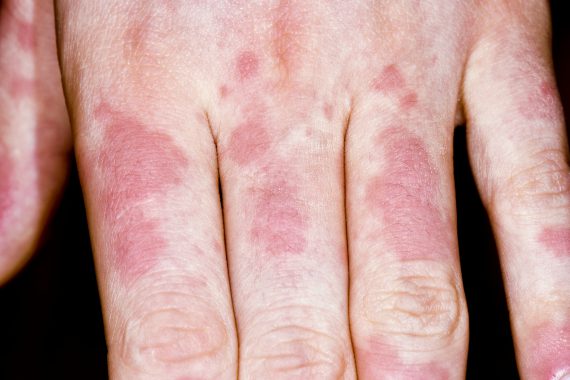
1. ‘I think I must be allergic to water.’
This 23-year-old lady says that, for the past year or so, every time she is in contact with water, she develops ‘hives’. She shows you a picture on her phone that confirms urticaria. This happens irrespective of whether she’s having a bath or showering and seems unrelated to soaps or bubble baths. It has also happened while swimming. The rash is itchy and takes about half an hour to fade.
2. ‘There must be some reason why I keep getting kidney pain and blood in my urine.’
This 30-year-old woman has just been discharged following her third episode of loin pain and frank haematuria. You look back through the correspondence for each occasion, and the pattern is the same – renal colic-type pain with visible haematuria. However, all hospital investigations are normal and in between episodes, she seems fine.
3. ‘The dentist says it’s not my jaw joint – so what now?’
You saw this 40-year-old man a month or so ago. On the basis that his sharp jaw and throat pains seemed linked to jaw movements, you suspected temporomandibular joint dysfunction, although the symptoms weren’t typical, and advised him to see his dentist. Now the pain is worse, is happening on swallowing and is putting him off eating. Examination of his neck and pharynx reveals no abnormality.
4. ‘So what’s my thyroid doing this time?’
About three months ago, this lady presented with a two-week history of ‘sore throat and swollen glands’. She was referring to her thyroid, which was swollen and tender. TFTs suggested hyperthyroidism but when you repeated them a few weeks later, to clinch the diagnosis prior to treatment, to your surprise, they suggested hypothyroidism. A further repeat now reveals them to be normal.
5. ‘It’s good news that I haven’t got bowel cancer, but I’m still suffering with diarrhoea.’
This 65-year-old lady presented with persistent diarrhoea of around six to nine months’ duration. Blood tests, including coeliac screen and faecal calprotectin, were all normal and the colonoscopy done at the local hospital to exclude bowel cancer showed no abnormalities. Her medical history includes osteoarthritis, COPD, GORD and two surgical procedures – a knee replacement and a cholecystectomy.
Answers
1. Aquagenic urticaria
This is not technically an allergy to water but rather a very rare form of physical urticaria (now classified as inducible urticaria) where hives develop immediately on contact with water regardless of temperature. It is not IgE-mediated. It typically presents in early teens and tends to affect young women. Reactions tend to occur with activities such as bathing, swimming or walking in the rain. The response to antihistamines is variable.
2. Primary loin pain haematuria syndrome.
This affects less than 0.1% of the population and usually presents like renal colic, with loin pain and haematuria, which may or may not be visible. The pain can be bilateral. Typically, all investigations are normal – this is a diagnosis of exclusion. The cause is unknown, and management mainly revolves around pain management.
3. Eagle syndrome
Also known as stylohyoid syndrome, this is a rare condition that causes severe pain on swallowing to the point that patients stop eating because the pain can be so intense. It is due to an elongated styloid process that irritates the glossopharyngeal nerve. Excision of the styloid process can help.
4. Subacute (viral, De Quervain’s) thyroiditis
A painful, destructive thyroiditis characterised by hyperthyroidism due to release of pre-formed hormones. There is usually a preceding viral illness, acute neck pain, often radiating to the ear, and raised inflammatory markers. The duration of hyperthyroidism is generally one to three months. Hypothyroidism is common after the hyperthyroid phase but rarely permanent. Specific therapy is not usually necessary during the hyperthyroid phase, although beta-blockers can be helpful. Thionamides are contraindicated; glucocorticoids may decrease the duration of the clinical syndrome.
5. Bile acid malabsorption related diarrhoea
A cholecystectomy quite commonly leads to consistent bile acid diarrhoea. This can continue indefinitely unless treated appropriately with resins such as colestyramine. It is important to conduct the usual basic investigations to exclude other causes – particularly as colestyramine can mask symptoms due to it’s constipating effect.
How did you rate on the diagnostic genius scale? Score one point for each correct diagnosis:
| Score | You are a…. |
| 5 | Dr House – you’ve solved every pathological enigma |
| 4 | Dr Watson – Sherlock-level clinical sleuthing |
| 3 | Dr Feelgood – you’re a diagnostic star. In Canvey |
| 2 | Dr Lecter – you’ve no appetite for clinical oddities |
| 1 | Dr Dolittle – does a 20% hit rate even entitle you to a coffee break? |
| 0 | Dr Frank-N-Furter – a Rocky Horror Show of a clinic |
These cases are taken from Instant Wisdom for GPs, available from 20 October at Amazon.co.uk, priced £24.99
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.



 What do people really know about rare diseases?
What do people really know about rare diseases?










