GPs told to catch up on face-to-face health checks for the severely mentally ill
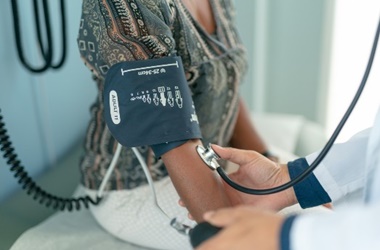
NHS England has said that GPs should work with mental health services to catch up on physical health checks for patients with severe mental illness, delivering them face-to-face where possible.
Practices should also ensure they bring any vulnerable patients in for face-to-face consultations if they have safeguarding concerns that make remote care inappropriate, NHS England added.
The latest update to the GP standard operating procedures said: ‘Practice staff should work proactively with secondary mental health care services to identify which individuals on the severe mental illness (SMI) register are due a physical health check.
‘Where face-to-face checks are not possible, practices should complete elements remotely, where practicable.’
NHS England added that ‘reasonable adjustments’ should be made to accommodate the needs of patients with severe mental illness when delivering the health checks.
The document also said GPs should have a ‘low threshold’ for bringing a patient in for a face-to-face consultation if there are safeguarding concerns.
It said: ‘Clinicians should consider when remote, video and face-to-face consultations are appropriate, particularly for vulnerable patients.
‘All clinicians need to remain vigilant and professionally curious and should retain a low threshold for bringing in a patient for a face-to-face consultation if there are safeguarding concerns.’
Practices should ensure their safeguarding policy is updated to accurately reflect issues around remote consultations and managing digital imagery, NHS England added.
Dr Tim Cooper, a GP partner in Hampshire and clinical lead for mental health at North Hampshire CCG, said it was important for GPs to continue SMI check-ups but that physical monitoring should involve secondary colleagues who historically ‘defer’ this back to practices.
He said: ‘We have to recognise the SMI patients are as important as those we are prioritising for other proactive services such as vaccination.
‘Where I think we should and could work better with our secondary health colleagues is on the physical monitoring of the SMI check – such as bloods, ECG, BMI, BP etc.
‘This is often a challenge throughout the year where it is often deferred back to practices.’
He added: ‘Locally, our clinical leads have been working proactively with our mental health trust to manage this, but more should be done to integrate these services.
‘It doesn’t make sense for patients to have to attend multiple appointments, which in a world of Covid-19 does increase everyone’s potential risk, particularly if there are elements of the health check that could be done with our providers and referred back to us.’
NHS England has revealed that mental health referrals have seen a sharp decline of an estimated 30-40% during the pandemic – while GPs have warned of an ‘imminent’ surge in mental health issues in the aftermath of Covid-19.
Pulse voluntary donation scheme
Since the outbreak of this pandemic, Pulse has strived to support you, whether it be through our resources page, our ‘Clinical Crises’ series, holding policymakers to account with exclusives such as practices being supplied with faulty masks, or GPs being told to stop routine services in the hardest hit areas.
However, good journalism cannot be done on the cheap and, like the whole publishing industry, we have been affected by the economic slowdown. We also strongly believe the content we produce should remain free as we feel it is essential for you. Because of this, we have set up a voluntary donation scheme. There is no compulsion whatsoever to donate. But if you feel we are helping you, and you would like to support us, anything you can spare would be greatly appreciated. Read more here.
Visit Pulse Reference for details on 140 symptoms, including easily searchable symptoms and categories, offering you a free platform to check symptoms and receive potential diagnoses during consultations.









