Revealed: GP representation on CCGs being eroded

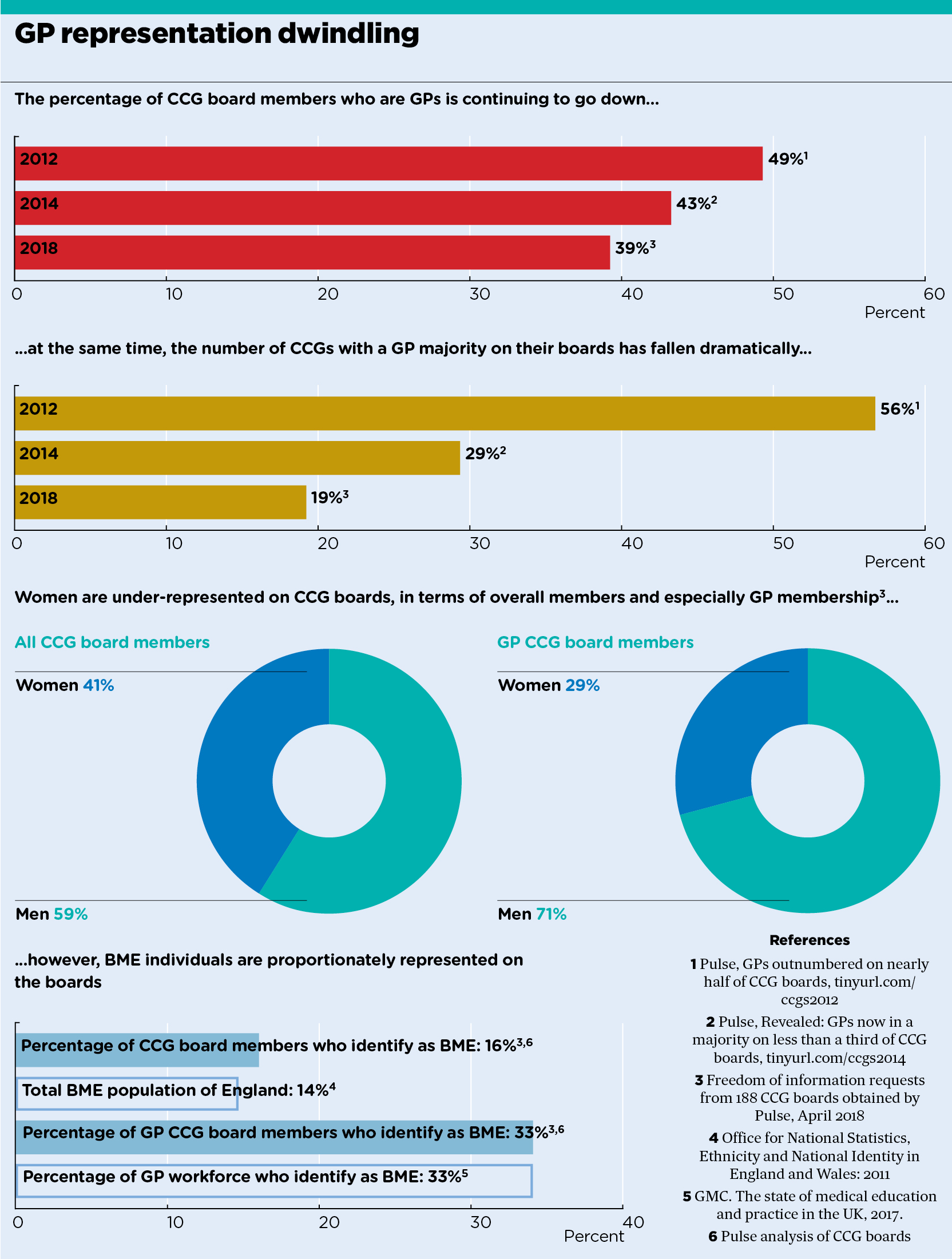
Exclusive GP representation on CCG boards has continued to decline with GPs now forming just 39% of all CCG board positions, new figures exclusively obtained by Pulse reveal.
This compares with 49% in 2012 – when CCGs were first set up – and 43% in 2014. Meanwhile, only one in five CCG boards have a GP majority now, compared with more than half in 2012.
GP leaders say that we have ‘reverted back to the equivalent of primary care trusts’.
The figures – obtained through freedom of information responses from 188 of the 207 CCGs in England – also reveal that only 29% of GPs on CCG boards are female, despite women making up more than 50% of the GP workforce.
However, the percentage of CCG board members who are black or minority ethnic are proportionate to general practice as a whole.
CCGs were established as part of Andrew Lansley’s Health and Social Care Act in 2012, with the then-health secretary telling GPs the point of the reform was to ‘give you and your colleagues in general practice the responsibility to shape services’.
But Pulse’s investigation reveals that in certain areas, GP presence on CCG boards is minimal. For example, in the north-east – where there are major GP recruitment problems – GPs are in a minority on every CCG board, constituting only 32% of board members. In the north region, GPs make up a majority on 8% of CCG boards.
However, in London the 32 CCGs reported a 47% of board members were GPs, with 44% of the boards boasting majority GP composition.
BMA GP Committee chair Dr Richard Vautrey said: ‘The idea of it being clinical-led commissioning is clearly not the case, we’ve reverted back to the equivalent of primary care trust with predominantly professional NHS managers leading the organisations.”
Dr Vautrey said it was clear from the beginning that GPs would have limited impact in CCGs, due to “tension between maintaining a clinical involvement and having time and capacity doing management roles”.
He added that many GPs are frustrated by NHS ‘bureaucracy’, and warned that the decline of GP involvement is likely to continue.
But NHS Clinical Commissioning co-chair Dr Graham Jackson said that GP involvement on CCGs is still strong.
He said: ‘When the CCGs were started back in 2012 there was a definite surge of GP interest, and I think it’s typical to use that as a yardstick. There was a freedom to set things up in any way you wanted to and I think that’s been rationalised down and it’s become more balanced across the country.’
Dr Jackson added: ‘The reality is CCGs are still GP-led organisation in statute… the important thing is, you need strong clinical leadership, but you need a high level of experience and competence in management.’
However, BMA GPC commissioning policy lead Dr Simon Poole said: ‘I think that many GPs that were involved with CCGs at the beginning were optimistic that they could make a difference, but many would agree they haven’t had the influence they were hoping for because of the structural and transactional constraints in the system as well as chronic underfunding and an increase in demand for services.’
NHS England said it is the CCG’s responsibility to manage the composition of board members. NHS England outlines a minimum membership asking boards to include at least one clinical leader who is either the chair of the board or the accountable officer, alongside executive positions including chief finance officer and chief operating officer.
june data lowdown for website









