Revealed: 450 GP surgeries have closed in the last five years

Exclusive Over a million patients have had to move surgeries in the last five years due to practice closures, a major Pulse investigation has revealed.
According to figures obtained by Pulse, 1.3m patients have seen their surgery closed as a result of practice closures or mergers.
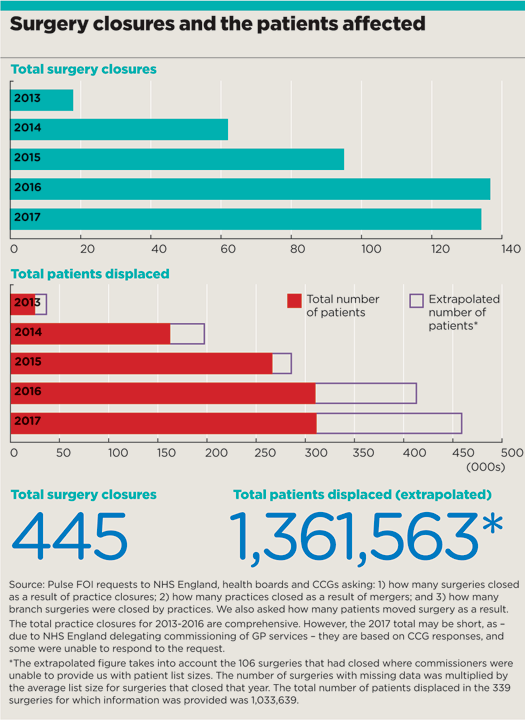
In all, nearly 450 GP surgeries have closed during the time period.
This has accelerated in the past two years, with 450,000 patients being displaced in 2017 as a result of 134 surgeries closing.
Practices have closed due to problems with recruitment and funding, with some practices facing huge cuts due to Government reforms.
It has also come despite NHS England and devolved governments putting more money into saving vulnerable practices.
GP leaders said the figures ‘will resonate with the experience of GPs across the country’ and show ‘a serious failure of the system’.
The figures, which were obtained through freedom of information requests, show that in 2017 alone around 460,000 patients had to find a new surgery after 134 practices either closed or merged. In 2016, 136 surgeries closed their doors, leading to 400,000 patients being displaced.
This is compared with figures from 2013, when just 18 practices shut their doors, impacting only 37,000 patients.
The figures show a mix of practice closing and GPs having to close branch surgeries as a result of recruitment and financial problems.
Official figures released this month revealed that the GP workforce in England had reduced by 1,000 since September 2015 – when health secretary Jeremy Hunt announced plans to increase the workforce by 5,000 by 2020.
Furthermore, the most recent data could be an underestimate as – due to NHS England’s delegating commissioning of GP services – they are based on responses from CCGs, and some were unable to respond to the request.
BMA GP Committee chair Dr Richard Vautrey said: ‘These new figures will resonate with the experience of GPs across the country as the recruitment and retention crisis in general practice is impacting practices of all sizes and all situations, as doctors face the pressures of rising workload, increasing administrative burden and a lack of resources.
‘Practices in rural and coastal regions, where the distance from large cities becomes a major obstacle in drawing in new recruits, have been particularly badly hit.’
He added that national initiatives to recruit GPs into these areas ‘will take some time before producing results’.
RCGP chair Professor Helen Stokes-Lampard said: ‘Sometimes, a closure is due to a practice merging, or becoming part of a federation, so that it can pool resources in the best interests of patient care.
But when it is because the practice team simply can’t cope with the resource and workforce pressures they are facing, it’s a serious failure of the system.’
She added that GPs handing back their contracts ‘is becoming increasingly common up and down the country, but particularly in rural and other ‘under-doctored’ areas where practices are finding it more difficult to recruit new GPs.’
Pulse has spoken to GPs in many of these areas, including Folkestone where GPs have said there is one GP for every 2,500 patients and Bridlington where withdrawn premises funding could be a ‘death knell’ for general practice in the area.
An NHS England spokesperson said: ‘More than 3,000 GP practices have received extra support thanks to a £27 million investment over the past two years and there are plans to help hundreds more this year.
‘NHS England is beginning to reverse historic underinvestment with an extra £2.4bn going into general practice each year by 2021, a 14% rise in real-terms.’
The Labour Party’s shadow health secretary Jonathan Ashworth said: ‘Falling numbers of family doctors and ever more GP closures have forced 1.3mn patients to find a new surgery. This exposes the real crisis in primary care after eight years of grinding Tory austerity across the NHS.
‘Labour has long called for primary care to be given greater priority and investment. A key test for Theresa May in the coming weeks will be whether or not she finally delivers the level of investment and support that primary care so obviously needs.’