GPs face increasing restrictions as NHS rations care to save money
Exclusive GPs face increasingly tighter restrictions on their ability to refer for specialist care, reveals an investigation by Pulse into plans drawn up by the most cash-strapped CCGs in the country.
The investigation reveals that CCGs are introducing policies that cap surgical referrals, require overweight patients to go a on a ‘weight loss programmes’ before an operation and deny hard-of-hearing patients hearing aids and audiological care.
The investigation comes as GPs say they are finding it harder to refer for surgical treatment of conditions like ganglions or carpal tunnel and, in one area, requests for hysterectomies are simply being ‘fobbed off with a Mirena coil’.
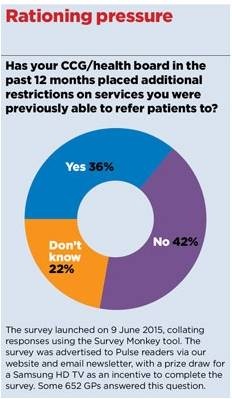
More than a third (36%) of GPs told Pulse they are facing new constraints on services to which they were previously able to refer.
The investigation comes as the health service prepares to implement £22bn of efficiency savings by 2020. But only two years after coming into existence, 19 CCGs have been ordered by NHS England to devise emergency plans to cut their budget deficits. A Pulse analysis of their recovery plans reveals:
- NHS Luton CCG says, ‘when appropriate, patients must stop smoking and/or undergo a weight loss programme’ before certain elective procedures.
- NHS North Staffordshire CCG said hearing aids will no longer be routinely provided for patient diagnosed with a mild hearing loss. Campaigners from Action on Hearing Loss labelled the decision ‘cruel’
- NHS Great Yarmouth and Waveney CCG demands that smokers give up, and obese people lose weight prior to hip and knee replacement therapy and this could be ‘rolled out to other surgical procedures’.
- NHS Basildon and Brentwood CCG has capped the numbers of vasectomy referrals that individual practices can make.
- NHS North East Essex CCG has a £22m funding shortfall and has had to put in a range of restrictions on vasectomies, female sterilisation and spinal physiotherapy to save £1m.
- NHS Mid Essex CCG has a ‘restriction policy’ for 2015/16 on services including acupuncture, facet joint injections and hip and knee operations.
NHS North East Essex CCG chair Dr Gary Sweeney explained: ‘We have no choice other than to stay within budget. If we do not implement these decisions we will have to select other services to restrict.’
Austerity NHS: What are GPs saying?
‘Women needing a hysterectomy are being fobbed off with a Mirena coil.’
GP in Hampshire
‘Referrals are downgraded regularly and we are increasingly scrutinised to ensure ‘appropriate’ referrals
GP in Neath
‘We have seen a rise in follow-up waiting times with patients being told by their consultant they’ll be seen in x months, but it’s increasingly quite unrealistic leading to patients making unnecessary appointments with GPs because they’ve not heard anything.’
Dr Richard Vautrey, GPC deputy chair
‘A grossly obese woman (BMI 60) had a request for lifesaving bariatric surgery refused, meaning further hoops, hurdles and delays.’
Dr Chris Nevill, Powys
NHS Alliance chair Dr Michael Dixon, agrees: ‘CCGs are caught between a rock and a hard place. They try to meet tough budgets and get vilified in the process.’
But Dr James Kingsland, president of the National Association of Primary Care, says that such moves are ‘unacceptable’. He said: ‘The idea of rationing necessary care in a service that is free at the point of use is just unacceptable. Any health commissioning body looking at rationing services need to question whether they are fit for purpose.’
GPC deputy chair Dr Richard Vautrey says the financial pressure is often hidden. He says: ‘Where patients may have waited three months, they now wait six – this sort of thing is difficult to measure. Until we get new funding into the NHS we will continue to come under financial pressure and it will get worse.’