GPs to publish grid of 42 different Ofsted-style ratings in waiting rooms

All GP practices will be given 42 different CQC ratings as part of proposals for the regulator’s new-style inspection regime, which they will have to publish in their waiting rooms as a contractual requirement.
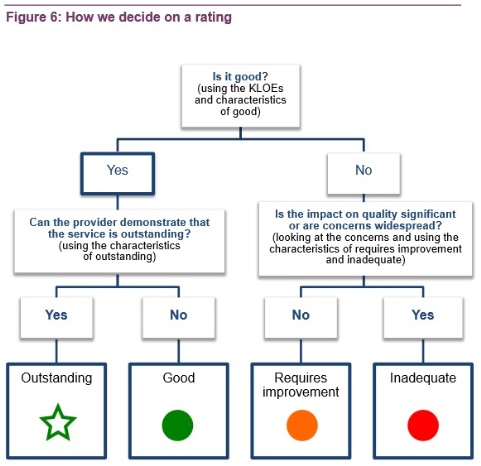
The CQC released its 100-page handbook yesterday, which sets out how practices will achieve ratings of ‘outstanding’, ‘good’, ‘requires improvement’ or ‘inadequate’ – a system that has been likened to the Ofsted-regime for the education sector.
The consultation period finishes in June, and will be informed by the first wave of inspections, which begin at the end of this month. Practices will be given ratings from October onwards.
It reveals that practices will be given ratings on how well they treat six different ‘population groups’: older people; patients with long-term conditions; mothers, babies and children; the working age population; people in vulnerable circumstances such as the homeless; and those with mental health problems.
Practices will also be given ratings for how effective, caring, responsive, safe and well-led they are – five ratings in all.
Finally, they will give practices ratings based on how effective, caring, responsive, safe and well-led they are for each population group – totalling 30 more ratings. All together, this will inform their single overall rating.
As part of the 2014/15 contract settlement, it was agreed that each practice should display their ratings in their waiting rooms and on their website.
The handbook says that inspectors should follow key lines of enquiry (KLOES) for each domain. For example, in the safety domain, questioning of practices will focus on how well they have learned from previous safety incidents, safeguarding, and staffing levels and suitability. The handbook sets out prompts for inspectors in each of these areas.
Practices will also have to demonstrate ease of access to out-of-hours appointments as part of the assessment of their care for working age patients.
Related stories
In full: CQC checklist for practices
They will be able to appeal their ratings under the terms set out in the Health and Social Care Act. They will also be able to take any CQC decisions they are unhappy with to a first-tier tribunal.
CQC chief executive David Behan said: ‘Over the past six months we set out proposals for different types of care services and we have been testing our new style inspections in hospitals, mental health and community health services and will be testing them in adult social care services and GP practices from this month.’
‘The changes we are making are vital to ensuring that we are able to make sure that health and social care services provide people with safe, effective, compassionate, high quality care and encourage care services to improve. Throughout these changes, we will always be on the side of people who use services and it is important to us that we hear what people think of our plans.’
Health secretary Jeremy Hunt said: ‘A new, independent and rigorous inspection regime will give the public vital information on health and social care performance, and the chief inspectors will shine a light on areas where improvement is needed. The CQC is seeking views on important elements of their inspection programme and I would encourage patients and all other interested parties to respond. This will help to drive up quality.’
The summary of the changes to the contract this year state: ‘It has been agreed that when the CQC new inspection arrangements are introduced from October 2014, practices will be required to display the inspection outcome in their waiting room(s) and on the practice website.’
‘These changes will be implemented through changes to the CQC regulations meaning the requirement will be on GP practices as a registered provider rather than as a requirement of holding a GMS contract. Further details and guidance will be available once the regulations have been finalised later in the summer of 2014.’