
child safeguarding 3×2 SUO
The high-profile deaths of Victoria Climbié and Baby P shook public and professional faith in the systems that should protect the most vulnerable in society.1,2 Every area of the system came under scrutiny, including GPs’ role in the tragedies; a GP who saw Baby P shortly before he died was criticised by the official report and suspended for 12 months for failing to act on his fears (although he was later reinstated).
Amid the recriminations, the reports on the two deaths concluded GPs and practice staff should refer earlier in cases of suspected abuse. This approach has now been formalised by the CQC, which is enforcing a regime of regular training and procedural checks in practices.
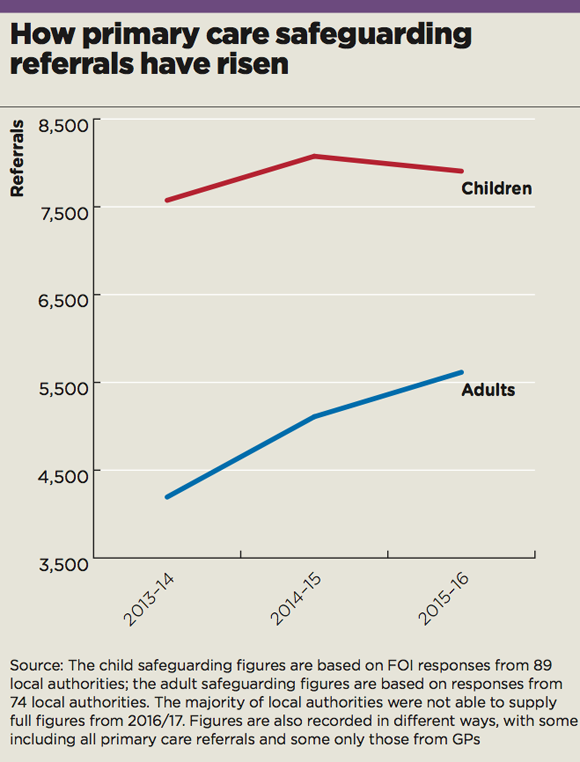
And GPs have responded. Figures obtained by Pulse reveal safeguarding referrals from primary care have risen by 15% in recent years.
But the increase in referrals has come at the same time as huge cuts to social care funding. This often leaves GPs unable to contact social services or enduring long waits on the phone. Even when they are able to get through, the level of demand means urgent cases often get overlooked, which puts the GP at risk; medical defence organisations say GPs must follow up on referrals, even if they are unable to contact social services. Failure to do this could result in serious consequences for a GP’s career.
And at the centre of this is a vulnerable patient who is being left at risk.
Data obtained by Pulse via Freedom of Information responses from 117 local authorities across England reveal safeguarding referrals from primary care continue to rise – by 4% between 2014/15 and 2015/16, with a startling 33% increase in referrals for adults over the same period. Extrapolated across England, this means around 25,000 adults and children who are suspected of being at risk of neglect or abuse are being referred by primary care each year.
Former RCGP lead on child safeguarding Dr Janice Allister, who helped to develop the college’s Safeguarding Children Toolkit for General Practice,3 says this rise is due in large part to the CQC’s intervention.
Dr Allister says: ‘There’s been an incremental change over time – but with the CQC’s intervention, every practice now has to have processes and show they are up to date. It means GPs are taking more responsibility for it, and where they have struggled to do this on their own in the past, there is now more support from the rest of the practice.’
GPs have had a legal requirement since 1989 to refer a child to social care if they believe there is a possibility of significant harm,4 but the Baby P investigation emphasised the importance of sharing early concerns, and this duty was included in NICE guidance on child maltreatment, issued in 2009.5 More recently, revalidation requires GPs to demonstrate they are up to date on safeguarding training.
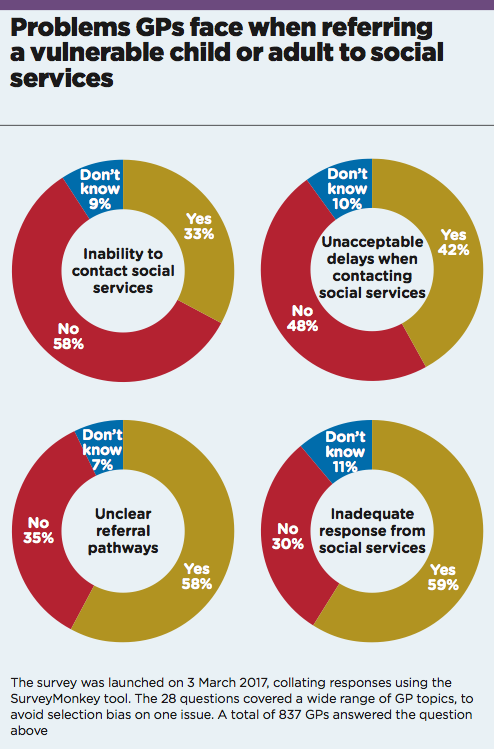
Yet it seems GPs’ efforts are being frustrated by the lack of response from social services. A Pulse survey of more than 800 GPs reveals they face significant hurdles when they try to raise concerns.
One-third of respondents report being unable to contact social services at all, while more than two-fifths experience unacceptable delays. And shockingly, three in five respondents feel social services fail to respond adequately.
This is despite government guidelines stating social services should acknowledge receipt and make a decision about the response required within one working day of a referral.6 As one GP from Hampshire, who asked not to be named, says: ‘They never reply and you have no idea what, if anything, has been done.’
Another GP from East Anglia, who also wishes to remain anonymous, tells Pulse there is ‘a lack of capacity’ in social services. ‘At a level-three child protection training recently, participants – including the trainer – agreed identifying need was useless if there was no effective response.’
figures box july 2017
Figures box, July 2017 cover
Many respondents to Pulse’s survey also described their frustration. Six out of 10 said they are hampered by unclear referral pathways. One GP from the north-west, who specialises in child safeguarding and also asked not to be named, tells Pulse of ‘failures to allocate social workers in a timely fashion’ and ‘frequent changes and a lack of experience’ among social work staff.
And the rising pressure on GPs to refer leads to defensive medicine, which heaps further pressure on social services.
Leicester GP Dr Grant Ingrams, who has expertise in forensic medicine, explains GPs are now being encouraged ‘to just refer on’, rather than making a decision on a case themselves.
Dr Ingrams says referral may not always be ‘appropriate’, fearing that, as a result, social services ‘have not taken other referrals seriously when I was very concerned’.
GP leaders say some of these problems stem from social care budget cuts; for example, for adult social care £4.6bn was cut between 2010 and 2016.
RCGP chair Professor Helen Stokes-Lampard says: ‘When this process isn’t as smooth as it should be, it’s frustrating – but this must not be used as an excuse to scapegoat social workers. We need a properly funded health and social care sector with general practice, hospitals and social care all working together.’
‘Tipping point’
Last year, the CQC said social care had reached a ‘tipping point’, with its annual report concluding cuts to services were ‘now beginning to impact both the people who rely on these services and the performance of NHS care.’7
But GPs could be held responsible if anything happens to a vulnerable patient further down the line. Medical defence bodies say GPs still have a responsibility to protect the patient if social services are not available – and advise GPs to call the police if all else fails (see box, above).
Izzi Seccombe, chair of the community wellbeing board of the Local Government Association, which represents councils, said: ‘Legislation and guidance are clear on the responsibilities of councils and health services working together to protect vulnerable adults and children. Both have membership of local safeguarding boards to ensure pathways and individual responsibilities are clear.’
But GPC regulation lead Dr Robert Morley warns these conflicting pressures are leaving GPs in an impossible situation. ‘Increasingly, GPs are the scapegoats of first choice for failures elsewhere in a system that is rapidly disintegrating.’
What GPs should do when faced with delays
If a GP cannot reach their usual social services contact they should take other steps to protect their patient. They can contact the local designated safeguarding lead or a senior person in social services, such as the local director. If that fails then, depending on the risk to the patient, the GP should consider speaking to the police. The GP should keep records of steps taken, including calls that have not been answered, in case they are called upon later to explain. A failure either to follow national safeguarding guidance or to take reasonable and robust steps to report concerns promptly could lead to criticism.
Dr Catherine Wills is deputy head of advisory services at the MDU
References
1 The Victoria Climbié Inquiry: report of an inquiry by Lord Laming, 2003. tinyurl.com/laming-climbie
2 Serious case review: Baby Peter. Haringey LSCB, 2009. tinyurl.com/Haringey-babyP
3 Safeguarding Children Toolkit for General Practic. RCGP/NSPCC, 2013. tinyurl.com/RCGP-NSPCC
4 Children Act 2009. tinyurl.com/children-act
References continued
5 Child maltreatment: when to suspect maltreatment in under 18s. NICE, 2009 tinyurl.com/Nice-cg89
6 Working together to safeguard children. HM Government, 2015. tinyurl.com/govt-safeguard
7 GP’s role in responding to child maltreatment: time for a rethink? NSPCC, 2014. tinyurl.com/NSPCC-GProle
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens















