Revalidation paperwork equivalent to 390,000 days’ worth of GP appointments

Exclusive GPs spend on average 55 hours a year on the revalidation process – equivalent to 1,300 full-time GPs working eight sessions a week – a Pulse survey has revealed.
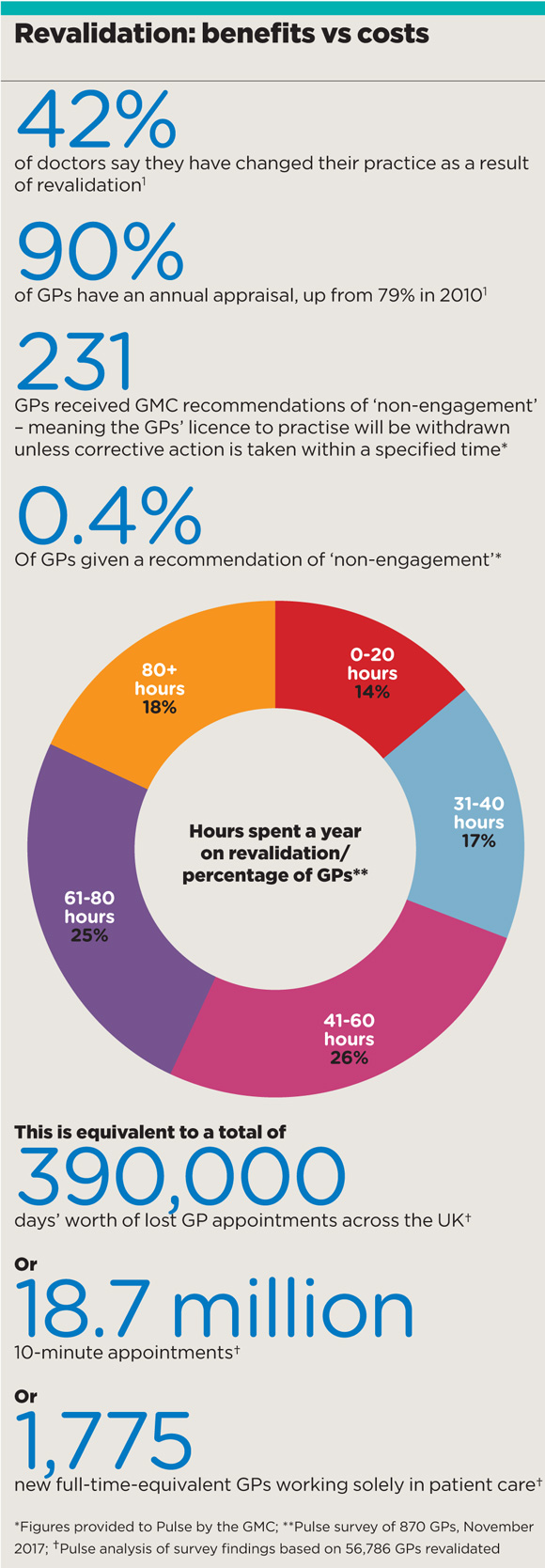
The survey of 870 GPs found that more than a quarter spend more than 70 hours on revalidation, while only 15% spend less than 20 hours – which is how long it is supposed to take.
This is equivalent to 390,000 days’ worth of appointments lost to patients at a time when many are waiting at least two weeks for an appointment.
A Pulse investigation has also revealed that only 231 – or 0.4% – of all the revalidation recommendations made for GPs were serious enough for the regulator to threaten to withdraw a licence to practise. And that there is little evidence that revalidation improves patient care.
The survey, carried out last November, asked GPs how long they spend on the overall process of revalidation. A midpoint analysis revealed that they spend on average 55 hours a year. However, this is far greater that the two sessions a year cited by the RCGP for preparation and appraisal.
Dr Alan Woodall, a GP in Powys, Wales and the founder of the pressure group GP Survival, said: ‘For every hour of learning you can add another hour of recording and collating information. I spent three hours the other night going through information governance and child protection, none of which required any real learning.’
Meanwhile, the deputy chair of the BMA’s GP Committee, Dr Mark Sanford Wood, said although the union is supportive of the principle of revalidation, ‘considerable improvements’ need to be made.
He said that the 55 hours identified in Pulse’s survey was higher than the BMA’s findings, but added: ‘The time originally set aside was two sessions a year, one for preparation and one for the appraisal. But we know anecdotally that GPs are spending considerably more than that in putting together appraisal and evidence, probably in the region of four or five sessions a year which is a significant chunk of time taken away from patient contact.’
He added: ‘We need a national discussion about the evidence that’s required versus the delivery of patient care, particularly at the moment where we just don’t have enough GPs to do that job.’
But the GMC said this is bringing about positive change. A spokesperson said: ‘Revalidation has helped to strengthen the way we regulate doctors and embed a consistent approach to appraisal. Indeed, appraisal rates have risen steeply in all four countries of the UK since its introduction.
‘Doctors have said that the feedback they get from patients is particularly valuable for identifying areas for improvement. Revalidation in turn plays a vital role in assuring patients that their doctors are keeping up to date and have regular checks, maintaining confidence in the profession.’
But neither the GMC or the Department of Health were able to point to any evidence that revalidation has reduced avoidable deaths, harm caused by doctor or litigation costs, as claimed before revalidation was rolled out.
A DH spokesperson said: ‘As highlighted in the Taking Revalidation Forward review in January, the process has delivered significant benefits through its appraisal system and strengthened clinical governance procedures.’
Please note: the orginal version of this article mistakenly said it included the ’ten hours a year spent on CPD’. This was incorrect. The survey question referred to time spent on the ‘revalidation process’. We’re sorry for any confusion caused
revalidation benefits vs costs 580x1668px
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens










