GP workload ‘not cut by social prescribing’
Referring patients for social activities, such as gardening or cooking, did not cut subsequent GP consultations or improve patients’ health outcomes, an evaluation of a pilot scheme in east London practices has found.
Patients seen by ‘link workers’ in the practice, who then referred them to programmes involving gardening or cooking, continued to have higher GP consultation rates and use more prescription medicine than controls a year after referral.
Referred patients consulted their GP more than eight times a year before and one year after referral, compared with four times a year for control patients.
But the authors said more research was needed to evaluate the approach fully, and suggested the scheme may have had wider societal benefits.
Lead author Dr Sally Hull, a GP and reader in primary care development at Queen Mary University of London, told Pulse ‘there was no demonstrable impact on GP consultation rates’, and that ‘we were not able to show a change in outcomes such as levels of depression, anxiety or confidence in self-management’.
But she added: ‘That does not mean we should stop the schemes, but that we need better ways of evaluating them.’
SAPC 2016, abstract 1D.4
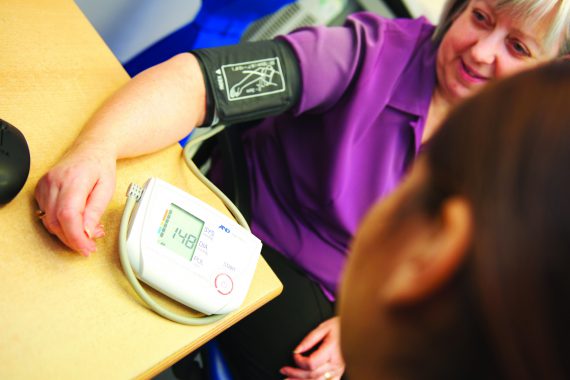
Risk tool ‘could detect missed hypertension’
GPs could identify thousands of missed cases of hypertension with the help of a simple blood pressure risk tool.
The Predicting Out-of-Office Blood Pressure (PROOF-BP) risk algorithm looks at measures such as clinic BP, age, gender and history of CVD to help GPs decide if someone with relatively normal clinic blood pressure readings might still be at risk of hypertension and should undergo ambulatory blood pressure monitoring (ABPM).
Currently, NICE guidelines recommend ABPM in people with a raised clinic blood pressure of 140/90mmHg. But researchers from the University of Birmingham said this excludes around 10-15% with masked hypertension. It also means those with white-coat hypertension undergo ABPM unnecessarily.
Using computer modelling to assess use of PROOF-BP to help guide ABPM, they estimated that using the tool in this way would pick up 14,623 additional cases of hypertension for every 100,000 people with clinic blood pressure of 130/80mmHg or above. It would also cut out 18,578 unnecessary ABPM investigations, compared with the current NICE approach.
The authors calculated that the algorithm would be cost effective ‘compared to the conventional blood pressure diagnostic options in primary care’ and would lead to reduced death and disability.
SAPC 2016, abstract 1C.3
Recalcitrant reception staff ‘hit satisfaction’
Unhelpful GP practice receptionists drive a decline in patient satisfaction, a new study claims.
Researchers from the University of Loughborough analysed recorded conversations between receptionists and patients, and cross-referenced their findings with results from the GP Patient Survey.
They revealed that where receptionists left it to patients to lead the conversation and ensure they get the service they requested, satisfaction suffered.
The paper said: ‘Analysis identified a burden on patients to drive calls forward and achieve service. “Patient burden” occurred when receptionists failed to offer alternatives to patients whose initial requests could not be met, or to summarise relevant next actions at the end of calls’.
They concluded the findings have implications for how GP practices train reception staff.
But RCGP chair Dr Maureen Baker said: ‘It is not an easy job, and all-too often receptionists bear the brunt of criticism if a patient is not satisfied with their care. Yet in the majority of cases, dissatisfaction may be as a result of circumstances out of their control.’
BJGP 2016, online 16 Aug
GPs ‘must share blame for rising demand’
GPs have to take some responsibility for levels of patient demand because they overprescribe and ‘fan the flames’ of society’s health concerns.
Glasgow GP Dr Des Spence made the claim in a BJGP editorial, adding that GPs should ‘prescribe less, intervene less and refer less’, as they are ‘fanning health anxiety’ by handing out antibiotics unnecessarily.
Dr Spence said: ‘The current clinical practice of us GPs is responsible for the increasing demands on general practice in the UK.’
He concluded that the debate on workload should instead be a debate about clinical practice, because ‘good medicine can only be achieved through good access, and good access can only be achieved by less medicine’.
BJGP 2016, online 1 Aug
Feedback can ‘reduce high-risk prescribing’
Offering practices feedback on prescribing safety data can reduce high- risk prescribing, according to a new study.
Practices in Scotland that received feedback on their prescribing and how it compared with a benchmark based on the top 25% of safest-prescribing practices the previous year were 12% more likely to reduce high-risk prescribing compared with usual care.
Those who received this feedback, plus information that encouraged them to search for and review patients who might be vulnerable to high-risk prescribing, were 14% more likely to reduce high-risk prescribing, compared with usual care.
Some 262 practices in Scotland were randomised to deliver either one of the two interventions, or usual care.
Lead author Professor Bruce Guthrie, GP and professor of primary care research at the University of Dundee, concluded: ‘The potential for feedback interventions to improve prescribing safety is considerable, and many healthcare systems could deploy similar interventions now.’
BMJ 2016, online 18 Aug
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens