Exclusive More than one quarter of black and minority ethnic GPs experience discrimination from patients at least monthly, with some stating that it’s a daily occurrence, Pulse can reveal.
A Pulse survey found that three quarters of all BME GP respondents have faced racial discrimination from their patients at some point.
And one quarter said that they felt discriminated against by a practice they had applied to join.
GPs told Pulse that the discrimination ranged from overt abuse to subtle behaviours that made consultations difficult, leading to complaints.
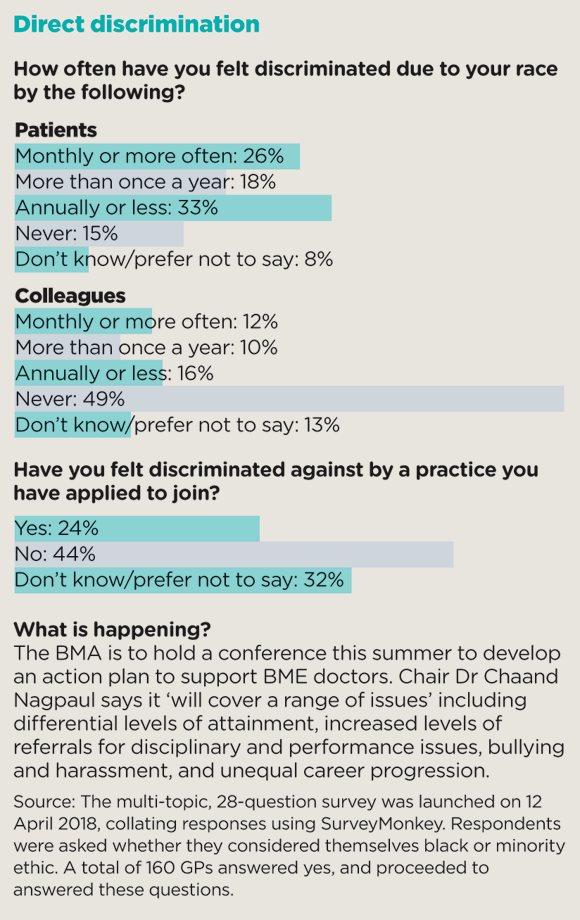
According to the findings, 26% of BME GPs experienced discrimination due to their race by patients at least monthly, while an additional 18% said it happened more than once a year, and 33% reported it as annually or less.
The results also showed that just over one in three BME GPs faced the same discrimination from some of their colleagues, with 12% stating it occured monthly or more often.
When asked whether they had felt discriminated against by a practice they had applied to join, 24% said yes, 44% said no and 32% said they didn’t know or preferred not to say.
Accrington GP partner Dr Murthy Motupalli, who originally trained in India, told Pulse: ‘Some patients speak to me as if they can wipe their feet on me, but the same person will speak very politely to my white colleagues.
‘I can see the very clear difference in the way I’m treated.’
One GP, who wished to remain anonymous, said: ‘Most of the time the discrimination can be subtle, where one loyal patient had informed me that patients in the waiting room had been discussing amongst themselves that they would refuse to see, “a coloured doctor.”
‘Others were apparently fearful that the doctor wouldn’t be able to speak English to an adequate level.’
He also recalled that ‘in one incident, a patient was less subtle and had shouted: “You fucking black bastard”, having not gotten what they wanted’.
The GP said that this ‘overt abuse’ is less common, and that what usually occurs is that the patient will ‘show dissatisfaction from the outset, either in their body language or tone of voice, leading to a difficult consultation and communications despite my best efforts to build rapport’.
He explained that this results in ‘erroneous’ complaints to the practice manager, such as ‘the doctor doesn’t know what he was doing, he was having to look up the drug in a book’.
He added that these experiences have been disheartening, as he was ‘born and brought up in Yorkshire’ and chose to return to practice there amongst ‘working class folk that I also originally belong to’.
Another GP told Pulse that on his practice’s google reviews patients are ‘openly commenting they cannot see a white doctor’ and that ‘for such patients due to your colour you can never do anything right in their eyes’.
The BMA responded to the survey, calling the results were ‘very concerning’.
BMA chair, and GP partner in North London, Dr Chaand Nagpaul added: ‘The BMA will be holding an important event in the summer looking at concerns of racial bias in the NHS affecting the medical profession.’
He explained that it will ‘cover a range of issues’ including differential levels of attainment, increased levels of referrals for disciplinary and performance issues, concerns regarding bullying and harassment, and unequal levels of achievement and career progression.
The event will focus on tackling these issues with ‘defined action and solutions’.
These findings come as the GMC has announced a review looking at why BME doctors are more likely to face complaints from employers than their white colleagues.
Chief executive Charlie Massey told the attendees at the British Association of Physicians of Indian Origin conference last month that it will look at conscious and unconscious bias, workplace cultures and representation in fitness-to-practice investigations.
Pulse October survey
Take our July 2025 survey to potentially win £1.000 worth of tokens













